Home > Health Insurance Marketplace > Arizona Heath Insurance Marketplace
Find Arizona Health Insurance Marketplace Coverage for 2026

Compare ACA plans and check subsidy savings from a licensed third-party health insurance agency.

Arizona Health Insurance Marketplace Guide
This guide, including the FAQs below, was created to help you better understand the Arizona health insurance Marketplace and pick the right health plan for you and your family. For many, an Affordable Care Act Marketplace plan – also called an Obamacare plan – may be a good choice.
Arizona uses the federally-facilitated Marketplace, so residents enroll through HealthCare.gov. Seven private insurance companies offer coverage through Arizona’s health insurance Marketplace for 2026, with varying coverage areas1 (see details below about changes in insurer participation and premiums for 2026).
Marketplace plans are used by people who need to buy their own insurance, including those who are self-employed, workers at small businesses without health benefits, and early retirees under 65 who need coverage until Medicare.
Metal level details in your state
Affordable Care Act plan costs and subsidy savings vary by metal level. Select your state to see average premiums and subsidy savings for each metal level – and see the percentage of your state’s enrollees who bought plans at each metal level.
Marketplace plan cost comparison (by metal level*)
Click “Find plans” to take a look at premium and benefit options offered by our agency partners.
Click “Find plans” to take a look at premium and benefit options offered by our agency partners.
Provide information above to get an estimate.
*Values displayed by this tool are from data generated by CMS and reflect 2026 Marketplace health plans purchased in each state. The values returned are averages based on the plans purchased by consumers of each selected state: subsidy and premium values vary based on factors such as zip code, age, household size, and income.
*Values displayed by this tool are from data generated by CMS and reflect 2026 Marketplace health plans purchased in each state. The values returned are averages based on the plans purchased by consumers of each selected state: subsidy and premium values vary based on factors such as zip code, age, household size, and income.
Arizona Marketplace quick facts
Frequently asked questions about health insurance in Arizona
Who can buy Marketplace health insurance in Arizona?
To buy Marketplace health coverage in Arizona:5
- You must live in Arizona.
- You must be lawfully present in the U.S.
- You can’t be incarcerated.
- You can’t be enrolled in Medicare.
To qualify for financial assistance (which depends on your household income) through the Arizona Health Insurance Marketplace:
- You can’t be eligible for affordable coverage offered by an employer. You can use this tool to see if the employer-sponsored coverage available to you is considered affordable.
- You can’t be eligible for AHCCCS (Medicaid) or KidsCare (CHIP)
- You can’t be eligible for premium-free Medicare Part A.6
- If married, file a joint tax return.7
- Not be able to be claimed by someone else as a tax dependent.7
When can I enroll in an ACA-compliant plan in Arizona?
Arizona’s open enrollment period for 2026 coverage ended on January 15, 2026.
The next open enrollment period, for coverage effective in 2027, will run from November 1, 2026 to December 15, 2026. This is shorter than the window that was used for the past several years, due to a federal rule change.
Outside of open enrollment, you may still be able to sign up for or make changes to an ACA Marketplace health plan (or an off-exchange plan) during a special enrollment period (SEP). To qualify for a SEP, you’ll generally need a qualifying life event, although American Indians and Alaska Natives can enroll year-round without a specific qualifying life event.
How do I enroll in a Marketplace plan in Arizona?
Here are the main ways to enroll in a Marketplace health plan in Arizona:
- Directly through HealthCare.gov
- By phone at (800) 318-2596 (TTY: 1-855-889-4325). Talk to an agent 24 hours a day, seven days a week, except for holidays.
- With the help of a local agent/broker, Navigator, or certified application counselor.
- Via an approved enhanced direct enrollment entity (EDE).8 (Make sure you request an on-exchange enrollment if that’s your preference, as EDEs can also generally enroll you in off-exchange coverage if you prefer that. Subsidies are only available if your enrollment is on-exchange.)
How can I find affordable health insurance in Arizona?
In Arizona, individuals and families can generally find affordable health insurance coverage by shopping on HealthCare.gov, which is Arizona’s health insurance Marketplace. The Marketplace offers two different types of income-based subsidies:
- Premium subsidies: Depending on your household income, you could be eligible for subsidies known as Advance Premium Tax Credits (APTC) that help lower your monthly premiums.
About 83% of Marketplace enrollees in Arizona qualified for premium subsidies in 2026, saving an average of $555 monthly. Subsidy-eligible enrollees paid an average of $133 per month for health coverage.9 But subsidy enhancements expired at the end of 2025, resulting in 2026 premium subsidies that aren’t as widely available and that cover a smaller share of premiums. - Cost-Sharing Reductions: If your income is no more than 250% of the federal poverty level10 and you select a Silver-level plan, you can receive cost-sharing reductions (CSR) in addition to APTC. CSRs help reduce your out-of-pocket costs, making medical care more affordable when you need it.11

Source: CMS.gov9
Medicaid: If you’re eligible for Medicaid, you can enroll through the Arizona Health Care Cost Containment System (azahcccs.gov) or Health-e-Arizona (healthearizonaplus.gov).
Short-Term Health Insurance: Consider short-term health insurance if you need a more budget-friendly option and are either ineligible for Marketplace subsidies or Medicaid, or missed the enrollment window for a Marketplace plan (in that case, you’ll want to make sure you go back to the Marketplace to enroll during the next open enrollment window, which begins November 1 each year).
How many insurers offer Marketplace coverage in Arizona?
Seven private insurance companies offer coverage through Arizona’s health insurance Marketplace for 2026, with varying coverage areas.1
There were a couple of important changes for 2026:
- Aetna exited the market at the end of 2025, as was the case in all states where Aetna offered individual market coverage.
- Blue Cross Blue Shield of Arizona is continuing to offer Marketplace coverage in 2026, but only HMOs.12 The carrier did not renew its PPO plans, so people with BCBSAZ PPO coverage had to select a new plan for 2026.13
Are Marketplace health insurance premiums increasing in Arizona?
The following average rate increases were approved for Arizona’s Marketplace insurers, applicable to full-price plans (meaning before subsidies are applied):
Arizona’s ACA Marketplace Plan 2026 APPROVED Rate Increases by Insurance Company |
|
|---|---|
| Issuer | Percent Increase |
| Aetna CVS Health/Banner Health | Exited the market |
| Cigna HealthCare of AZ, Inc. | 33.8% |
| Blue Cross and Blue Shield of Arizona HMO | 48.7% |
| Blue Cross and Blue Shield of Arizona PPO | Exited the market |
| Imperial Insurance | 19.3% |
| Arizona Complete Health (Health Net of AZ) | 48.9% |
| Oscar Health Plan, Inc. | 26.1% |
| UnitedHealthcare of Arizona, Inc. | 44.3% |
| Antidote Health Plan of Arizona | 18% |
Source: Arizona Department of Insurance1
The weighted average rate increase was 46.3%, before subsidies are applied.14
When looking at overall average rate changes, it’s important to understand:
- The rate increases show above are for full-price plans. Most Arizona Health Insurance Marketplace enrollees received premium subsidies in 2025,15 so their net rate change also depended on how much their subsidy changed.
- Federal subsidy enhancements expired at the end of 2025 (this issue was still under consideration by lawmakers as of January 2026). As a result, subsidies aren’t available in 2026 to enrollees with household income over 400% of the federal poverty level. And for people with income below that, subsidies don’t cover as much of the premium as they did in 2025. So the net premium percentage increase for most enrollees was much higher than the 46% average increase in full-price premiums.14
- Averages don’t account for premiums increasing with age. People pay more each year as they get older (subsidies are larger for older enrollees to account for this, but as noted above, 2026 subsidies don’t cover as much of enrollees’ premiums as 2025 subsidies did).
- A weighted average lumps all plans together. But rate changes vary by insurer (as noted above) and plan.
For perspective, here’s a summary of how average pre-subsidy premiums have changed over time in Arizona’s individual/family health insurance market:
- 2015: Average decrease of 3%16
- 2016: Average increase of 12.3%17
- 2017: Average increase of 57%18
- 2018: Nearly flat rate for the two on-exchange insurers19
- 2019: Average decrease of 6.3%20
- 2020: Average decrease of 0.2%21
- 2021: Average increase of 0.4%22
- 2022: Average increase of 0.5%23 (three new insurers joined the exchange)
- 2023: Average increase of 4.3%24
- 2024: Average increase of 0.3%25
- 2025: Average increase of 4.2%26
How many people are insured through Arizona’s Marketplace?
During the open enrollment period for 2026 coverage, 357,144 people signed up for private health plans through Arizona’s exchange.2
The increase in enrollment in prior years was driven in large part by the enhanced premium subsidies available as a result of the American Rescue Plan and Inflation Reduction Act.27
But the subsidy enhancements expired at the end of 2025. As a result, enrollment for 2026 was trending lower than enrollment had been at the same time the year before.28
The enrollment spike in 2024 and 2025 was also driven by the “unwinding” of the pandemic-era Medicaid continuous coverage rule. According to CMS, more than 134,000 people transitioned from Arizona Medicaid to a Marketplace plan during the unwinding process.29
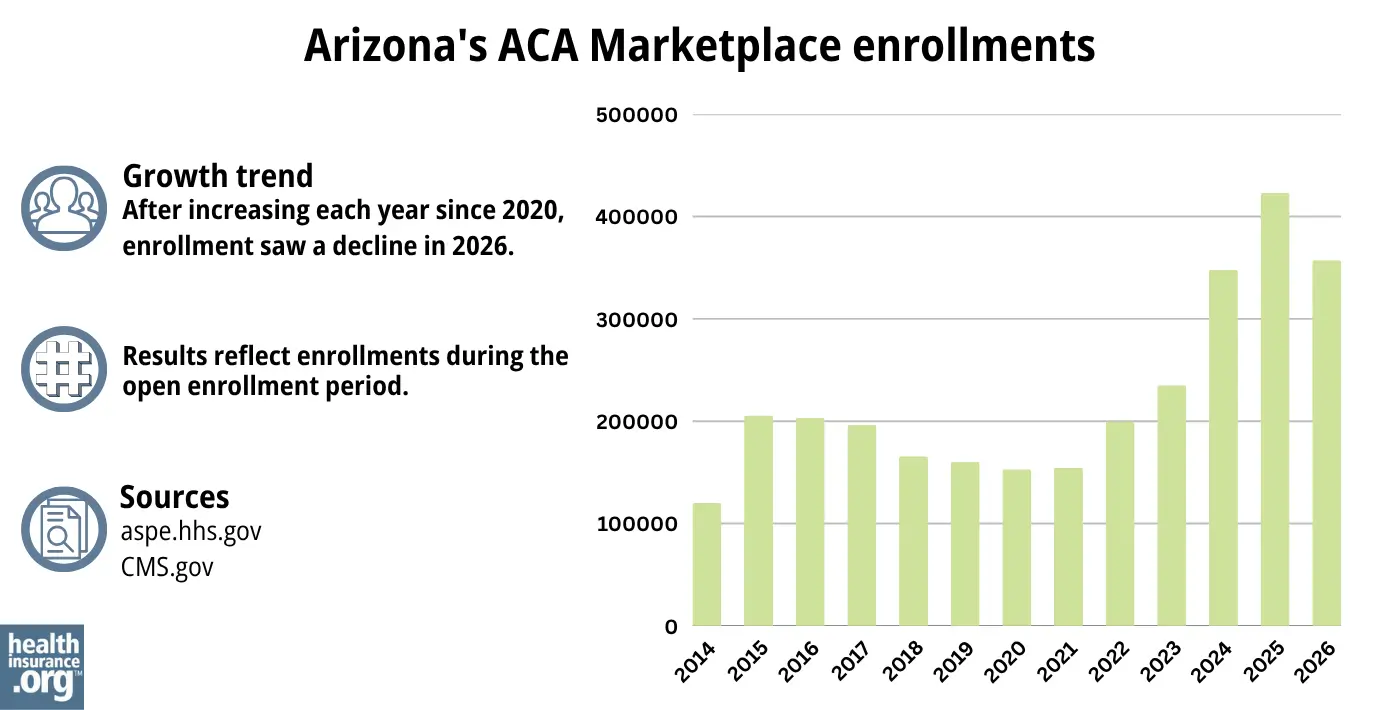
Source: 2014,30 2015,31 2016,32 2017,33 2018,34 2019,35 2020,36 2021,37 2022,38 2023,39 2024,40 202541 20262
What health insurance resources are available to Arizona residents?
HealthCare.gov
The official federal website where you can sign up for health insurance plans through the ACA Marketplace.
Arizona Department of Insurance
Regulates and licenses health plans, agents, and brokers. Provides consumer information about insurance.
Arizona Health Matters
A resource that provides information about health concerns in Arizona.
Arizona Association of Community Health Centers/Arizona Alliance for Community Health Centers
Community health centers that are also Arizona’s federally-funded Navigator. Help with exchange enrollments.
Arizona Health Care Cost Containment System
Administers Medicaid in Arizona. Provides coverage to low-income residents.
Medicare Rights Center
National service with a website and call center to assist Medicare beneficiaries and their caregivers.
Arizona State Health Insurance Assistance Program
Local counseling, advice, and assistance with Medicare issues.

Looking for more information about other options in your state?
Need help navigating health insurance options in Arizona?
Explore more resources for options in AZ including short-term health insurance, dental, Medicaid and Medicare.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- ”Individual and Small Group ACA Health Insurance Rate Changes” Arizona Department of Insurance. Oct. 8, 2025 ⤶ ⤶ ⤶
- ”2026 Marketplace Open Enrollment Period Public Use Files” Centers for Medicare & Medicaid Services. Accessed March 2026 ⤶ ⤶ ⤶
- ”Arizona Rate Review Submissions” RateReview.HealthCare.gov. Accessed Sep. 17, 2025 *The above is based on the most current data available. ⤶
- ”2026 Marketplace Open Enrollment Period Public Use Files” and “Marketplace 2025 Open Enrollment Period Report: National Snapshot” Centers for Medicare & Medicaid Services, Accessed March 2026 ⤶
- “A quick guide to the Health Insurance Marketplace” HealthCare.gov ⤶
- Medicare and the Marketplace, Master FAQ. Centers for Medicare and Medicaid Services. Accessed Jan. 22, 2026 ⤶
- Premium Tax Credit — The Basics. Internal Revenue Service. Accessed Jan. 22, 2026 ⤶ ⤶
- “Entities Approved to Use Enhanced Direct Enrollment” CMS.gov, Dec. 8, 2025 ⤶
- “2026 Marketplace Open Enrollment Period Public Use Files” CMS.gov, March 2026 ⤶ ⤶
- “Federal Poverty Level (FPL)” HealthCare.gov, 2023 ⤶
- APTC and CSR Basics. Centers for Medicare and Medicaid Services. June 2023. ⤶
- ”Arizona Rate Review Submissions” RateReview.HealthCare.gov. Accessed Sep. 17, 2025 ⤶
- ”2026 Blue Cross Blue Shield PPO Plan Exit” Phoenix Health & Life Insurance. Sep. 16, 2025 ⤶
- ”2026 Final Gross Rate Changes – Arizona: +46.3% (updated)” ACA Signups. Oct. 10, 2025 ⤶ ⤶
- ”Effectuated Enrollment: Early 2025 Snapshot and Full Year 2024 Average” CMS.gov, July 24, 2025 ⤶
- Analysis Finds No Nationwide Increase in Health Insurance Marketplace Premiums. The Commonwealth Fund. December 2014. ⤶
- FINAL PROJECTION: 2016 Weighted Avg. Rate Increases: 12-13% Nationally* ACA Signups. October 2015. ⤶
- Avg. UNSUBSIDIZED Indy Mkt Rate Hikes: 25% (49 States + DC). ACA Signups. October 2016. ⤶
- Major Medical Health Insurance Rate Filings and Final Rate Changes Effective Date January 1, 2018. Arizona Department of Insurance. October 2017. ⤶
- 2019 Rate Hikes. ACA Signups. October 2018. ⤶
- 2020 Rate Changes. ACA Signups. October 2019. ⤶
- Calculated by healthinsurance.org, based on approved rates and enrollment data in SERFF filings: Market share was as follows: 28% BCBSAZ; 15% Bright Health; 5% Cigna; 49% Health Net; 3% Oscar. Accessed December 2023. ⤶
- 2022 Rate Changes. ACA Signups. October 2021. ⤶
- UPDATED: FINAL Unsubsidized 2023 Premiums: +6.2% Across All 50 States +DC. ACA Signups. Accessed November 2023. ⤶
- So How’d I Do On My 2024 Avg. Rate Change Project? Not Bad At All! ACA Signups. December 2023. ⤶
- ”Arizona: *Final* avg. unsubsidized 2025 #ACA rate changes: +4.2% (updated)” ACA Signups. Oct. 15, 2024. And
“Individual and Small Group ACA Health Insurance Rate Changes” Arizona Department of Insurance and Financial Institutions. Sep. 16, 2024 ⤶ - Health Insurance Marketplaces 2023 Open Enrollment Report. Centers for Medicare and Medicaid Services. Accessed December 2023. ⤶
- ”Breaking: CMS posts claimed 2026 Open Enrollment: 22.8M QHPs, down 3.5% y/y so far” ACA Signups. Jan. 13, 2026 ⤶
- ”HealthCare.gov Marketplace Medicaid Unwinding Report” Centers for Medicare & Medicaid Services. Data through April 2024; Accessed Aug. 14, 2024. ⤶
- “ASPE Issue Brief (2014)” ASPE, 2015 ⤶
- “Health Insurance Marketplaces 2015 Open Enrollment Period: March Enrollment Report”, HHS.gov, 2015 ⤶
- “HEALTH INSURANCE MARKETPLACES 2016 OPEN ENROLLMENT PERIOD: FINAL ENROLLMENT REPORT” HHS.gov, 2016 ⤶
- “2017 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2017 ⤶
- “2018 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2018 ⤶
- “2019 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2019 ⤶
- “2020 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2020 ⤶
- “2021 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2021 ⤶
- “2022 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2022 ⤶
- “Health Insurance Marketplaces 2023 Open Enrollment Report” CMS.gov, 2023 ⤶
- ”HEALTH INSURANCE MARKETPLACES 2024 OPEN ENROLLMENT REPORT” CMS.gov, 2024 ⤶
- “2025 Marketplace Open Enrollment Period Public Use Files” CMS.gov, May 2025 ⤶

