Medicare in Indiana
Original Medicare, Medicare Advantage, Part D prescription drug, and Medigap coverage in Indiana

Key takeaways
- In Indiana, more than 1.3 million residents are enrolled in Medicare.1
- About 49% of Indiana Medicare beneficiaries are enrolled in Medicare Advantage plans.1
- Since 2020, Indiana has required Medigap insurers to offer at least Plan A to people under age 65, but the premiums are significantly higher than the premiums for a 65-year-old.
- About 82% of Indiana Medicare beneficiaries have Part D prescription coverage, either under a stand-alone plan or as part of their Medicare Advantage plans.1

Medicare enrollment in Indiana
As of August 2024, Medicare enrollment in Indiana stood at 1,372,886 people,1 which is nearly 18% of the state’s population.2
For most Americans, turning 65 is the path to Medicare enrollment. But younger Americans become eligible for Medicare if they have been receiving disability benefits for 24 months, or if they have ALS or end-stage renal disease. Nationwide, a little less than 11% of all Medicare beneficiaries are under age 65;3 in Indiana, about 12% of Medicare beneficiaries were under age 65 as of mid-2024.1
Read about Medicare’s open enrollment period and other important deadlines for Medicare coverage enrollment.
Indiana lawmakers passed legislation in 2024 (not yet signed into law as of February 2024) that would improve access to Medigap plans for beneficiaries under the age of 65.4This is described in more detail below, along with the state’s current rule for Medigap access when a beneficiary is younger than 65.
Learn about Medicare plan options in Indiana by contacting a licensed agent.



Explore our other comprehensive guides to coverage in Indiana

The ACA Marketplace allows individuals and families to shop for and enroll in ACA-compliant health insurance plans. Subsidies may be available based on household income to help lower costs.


Hoping to improve your smile? Dental insurance may be a smart addition to your health coverage. Our guide explores dental coverage options in Indiana.


Learn about Indiana’s Medicaid expansion, the state’s Medicaid enrollment and Medicaid eligibility.


Short-term health plans provide temporary health insurance for consumers who may find themselves without comprehensive coverage. Learn more about short-term plan availability in Indiana.

Frequently asked questions about Medicare in Indiana
What is Original Medicare?
Original Medicare is a federally-run program that does not vary from one state to another. So general Medicare eligibility in Indiana and Medicare enrollment in Indiana work the same way they do in every other state. For residents who aren’t yet receiving Social Security retirement benefits and thus aren’t automatically enrolled when they turn 65, the Medicare application in Indiana is done via the Social Security Administration, as is the case throughout the United States.
Available options for private Medicare coverage, including Medicare Advantage plans, Medigap plans, and Medicare Part D plans, do vary from state to state.
What is Medicare Advantage?
Medicare Advantage is available as a private alternative to Original Medicare. Medicare Advantage includes all of the benefits of Original Medicare (hospital and outpatient/physician coverage), although the out-of-pocket healthcare costs can be very different, as Medicare Advantage plans can set their own coinsurance, copays, and deductible levels (within parameters set by CMS).
Most Medicare Advantage plans also include Part D coverage for prescription drugs, as well as extra programs like dental and vision coverage. But Medicare Advantage plans tend to have localized healthcare provider networks, as opposed to Original Medicare’s nationwide access to healthcare providers. There are pros and cons to either option.
Twenty-eight percent of Medicare beneficiaries in Indiana were enrolled in Medicare Advantage plans as of 2018, compared with an average of 34% nationwide. As of August 2024, there were 678,862 Indiana Medicare beneficiaries enrolled in private Medicare plans.1
That’s in keeping with the national trend of increasing enrollment in Medicare Advantage plans over the last several years; Medicare Advantage accounted for about 50% of all Medicare beneficiaries nationwide as of August 2024.3
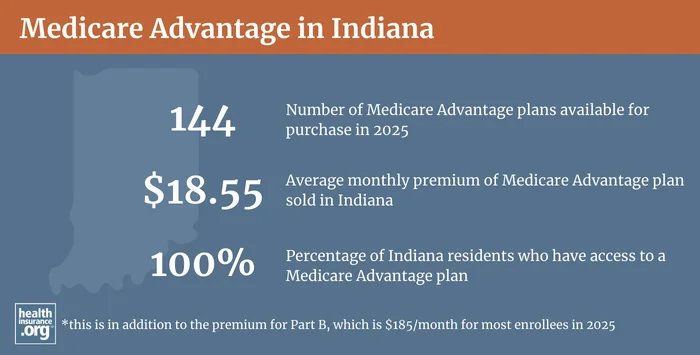
Medicare Advantage plan availability varies from one country to another. For 2024, Indiana residents can choose from among at least 44 Medicare Advantage plans, and up to 77 plans, depending on where they live (these numbers are a dramatic increase from 2020, when plan availability ranged from 11 to 30 plans, depending on the county).5
Medicare’s annual election period (October 15 to December 7 each year) allows Medicare beneficiaries to switch between Medicare Advantage and Original Medicare (and add or drop a Medicare Part D prescription plan). There is also a Medicare Advantage Open Enrollment Period (January 1 to March 31), during which a person who already has a Medicare Advantage plan can pick a different Advantage plan or switch to Original Medicare.
Indiana Medigap enrollment and regulations
According to AHIP, 370,851 Indiana Medicare beneficiaries were enrolled in Medigap plans (also known as Medicare Supplement insurance) in 2023,6 to supplement their Original Medicare coverage.
You can compare Medigap plans on Medicare.gov’s plan finder tool, or by using Indiana’s plan comparison tool. As of 2025, 39 insurers offered Medigap plans in Indiana.7
Unlike other private Medicare coverage (Medicare Advantage and Medicare Part D plans), federal rules do not provide an annual open enrollment window for Medigap plans. Instead, federal rules provide a one-time six-month window when Medigap coverage is guaranteed issue. This window starts when a person is at least 65 and enrolled in Medicare Part B. (You must be enrolled in both Part A and Part B to buy a Medigap plan.)
Federal rules do not guarantee access to Medigap plans for people who are under 65. However, the majority of the states have rules to ensure that disabled Medicare beneficiaries have at least some access to Medigap plans. Indiana requires Medigap insurers to make all policies guaranteed-issue for Medicare beneficiaries under the age of 65, during a six-month window when they’re first enrolled in Medicare.8,9
- For Medigap plans A, B, and D, the under-65 premiums must be the same as age-65 premiums.
- For other plans, such a Plan G or Plan N, the premium can be up to 200% of the age-65 premium.
Indiana also enacted legislation in 2025 to add a “birthday rule” starting in 2026. This will allow Medigap enrollees (who are at least 65) to switch to another Medigap policy within 60 days of their birthday, without medical underwriting. The new policy must have the same benefits as their existing policy (so someone with Plan N can only switch to another Plan N, for example).10
What is Medicare Part D?
Original Medicare does not cover outpatient prescription drugs. Some Original Medicare beneficiaries have supplemental coverage via an employer-sponsored plan (from a current or former employer or spouse’s employer), and these plans often include prescription coverage. But Medicare enrollees without drug coverage through an employer-sponsored plan need to obtain Medicare Part D prescription coverage (note that people who are dually eligible for both Medicare and Medicaid also get their drug coverage through Part D, rather than the Medicaid program). Part D coverage can be purchased as a stand-alone plan, or as part of a Medicare Advantage plan that includes Part D prescription drug coverage.
In Indiana, there are 16 stand-alone Part D plans for sale for 2025, with premiums as low as $0/month.11
As of August 2024, there were 1,150,227 Indiana Medicare beneficiaries who had Part D prescription coverage.1 About 45% had coverage under stand-alone Part D plans, while about 55% had Part D prescription coverage as part of their Medicare Advantage plans.1
Medicare Part D enrollment is available when a beneficiary first becomes eligible for Medicare. And the annual Medicare election period each fall (October 15 to December 7) allows beneficiaries the opportunity to switch to a different Medicare Part D plan or enroll for the first time if they didn’t do so when they were first eligible, although a late enrollment penalty can be assessed if they didn’t have creditable coverage before enrolling.

What additional resources are available for Medicare beneficiaries and their caregivers in Indiana?
Do you have questions about Medicare eligibility or need help enrolling in Medicare in Indiana?
- The Indiana Department of Insurance (IDOI) website is good resource for eligibility, enrollment, and other general Medicare information.
- The Indiana State Health Insurance Assistance Program offers free assistance for Medicare beneficiaries. Call their central office at 1-800-452-4800 or find a local office.
- The Medicare Rights Center has a comprehensive national website and a helpful call center that can provide a variety of assistance with Medicare-related questions.
- Programs of All-Inclusive Care for the Elderly (PACE): A Medicare and Medicaid program that helps seniors receive the care they need in their homes and local communities, without having to move into a nursing home.

Looking for more information about other options in your state?
Need help navigating health insurance options in Indiana?
Explore more resources for options in IN including ACA coverage, short-term health insurance, dental and Medicaid.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- “Medicare Monthly Enrollment – Indiana.” Centers for Medicare & Medicaid Services Data. Accessed December, 2024. ⤶ ⤶ ⤶ ⤶ ⤶ ⤶ ⤶ ⤶
- U.S. Census Bureau Quick Facts: United States & Indiana.” U.S. Census Bureau, July 2023. ⤶
- “Medicare Monthly Enrollment – US” Centers for Medicare & Medicaid Services Data, December 2024. ⤶ ⤶
- Indiana Senate Bill 215. BillTrack50. Passed February 2024. ⤶
- ”Medicare Advantage 2024 Spotlight: First Look” KFF.org Nov. 15, 2023 ⤶
- “The State of Medicare Supplement Coverage” AHIP. May 2025. Accessed Oct. 3, 2025 ⤶
- “Medicare Supplements Indiana” Indiana Department of Insurance, SHIP. Updated Sep. 23, 2025 ⤶
- “Indiana SB215” BillTrack50. Enacted Mar. 11, 2024 ⤶
- “Medicare Supplement Plans” Indiana Department of Insurance. Accessed Oct. 3, 2025 ⤶
- “Indiana HB1226” BillTrack50. Enacted Apr. 10, 2025 ⤶
- ”Fact Sheet: Medicare Open Enrollment for 2025” (44) Centers for Medicare & Medicaid Services. Sep. 27, 2024 ⤶

