Medicare in Nevada
Original Medicare, Medicare Advantage, Part D prescription drug, and Medigap coverage in Nevada

Key takeaways
-
- More than 600,000 residents are enrolled in Medicare in Nevada.1
- 51% of Nevada Medicare beneficiaries are enrolled in Medicare Advantage plans.1
- Some counties in Nevada have no Medicare Advantage plans available; plan availability ranges depending on the county.2
- There are 16 stand-alone Part D prescription plans available in Nevada in 2025, with premiums that start at $0 per month.3
- More than 165,000 of the state’s Medicare beneficiaries have stand-alone Part D coverage.1

Medicare enrollment in Nevada
As of September 2024, there were 602,788 people enrolled in Medicare in Nevada,1 amounting to about 17% of the state’s population.4
Most Americans become eligible for Medicare enrollment when they turn 65. But Medicare eligibility is also triggered for younger people if they’re disabled and have been receiving disability benefits for 24 months (people with ALS or end-stage renal disease do not have to wait 24 months for their Medicare coverage to begin).
In Nevada, about 9% of Medicare beneficiaries (roughly 53,000 people) are younger than 65 and eligible for Medicare due to a disability rather than age.1 Nationwide, about 11% of all Medicare beneficiaries — roughly 7.1 million people — are eligible due to disability.5
Learn about Medicare plan options in Nevada by contacting a licensed agent.



Explore our other comprehensive guides to coverage in Nevada

The ACA Marketplace allows individuals and families to shop for and enroll in ACA-compliant health insurance plans. Subsidies may be available based on household income to help lower costs.


Hoping to improve your smile? Dental insurance may be a smart addition to your health coverage. Our guide explores dental coverage options in Nevada.


Learn about Nevada’s Medicaid expansion, the state’s Medicaid enrollment and Medicaid eligibility.


Short-term health plans provide temporary health insurance for consumers who may find themselves without comprehensive coverage. Learn more about short-term plan availability in Nevada.

Frequently asked questions about Medicare in Nevada
What is Medicare Advantage?
In most areas of the United States, private Medicare Advantage plans are available as an alternative to Original Medicare.
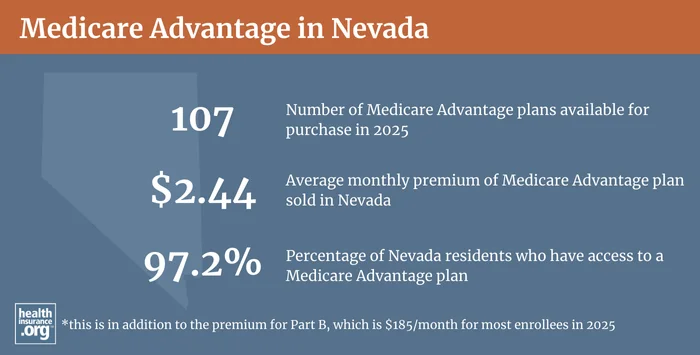
In 2025, some of Nevada’s counties have no Medicare Advantage plans available for purchase.2
Medicare Advantage plan availability in 2025 in Nevada ranges from zero plans in several rural counties, to 38 plans in Clark County.2
By early 2023 the number of people enrolled in private Medicare plans in Nevada stood at 308,144 people;1 the other 294,644 beneficiaries had Original Medicare.1
People who enroll in Original Medicare get their coverage directly from the federal government, and have access to a nationwide network of providers. But Original Medicare enrollees need supplemental coverage (from an employer-sponsored plan, Medicaid, or privately purchased Medigap plans) for things like prescription drugs and out-of-pocket costs.
Original Medicare includes Medicare Part A (hospital inpatient services) and Part B (outpatient services). Medicare Advantage includes all of the benefits of Medicare Parts A and B, and the plans usually also have additional benefits, such as integrated Part D prescription drug coverage, dental and vision coverage, and extra programs like gym memberships and a 24-hour nurse hotline. But provider networks and service areas are limited with Medicare Advantage, and out-of-pocket costs (deductible, copays, and coinsurance) are often higher than they would be under Original Medicare plus a Medigap plan. There are pros and cons to either option, and no single solution that works for everyone.
Medicare’s annual election period (October 15 to December 7 each year) allows Medicare beneficiaries opportunities to switch between Medicare Advantage enrollment and Original Medicare (and add, drop, or change to a different Medicare Part D prescription plan). Medicare Advantage enrollees also have the option to switch to a different Advantage plan or to Original Medicare during the Medicare Advantage open enrollment period, which runs from January 1 to March 31 (only one plan change may be made during this window).
Medigap enrollment and regulations in Nevada
According to AHIP, 99,601 Nevada residents had Medigap coverage as of 2023,6 which supplemented their Original Medicare coverage.
Learn how Medigap plans are regulated and standardized.
Medigap coverage is offered in Nevada by 21 insurers. Nearly all of them use attained age rating,7 which means that enrollees’ monthly premiums increase as they get older, regardless of how old they were when they purchased the policy.8
Unlike other private Medicare coverage (Medicare Advantage and Medicare Part D plans), federal rules do not provide an annual open enrollment window for Medigap plans. Instead, there’s a one-time six-month window when Medigap coverage is guaranteed-issue. This window starts when a person is at least 65 and enrolled in Medicare Part B (you must be enrolled in both Part A and Part B to buy a Medigap plan). If you apply for a Medigap plan after it ends, federal rules allow insurers to use medical underwriting to determine your eligibility for coverage and your monthly premium.
Nevada’s Medigap birthday rule
But Nevada enacted legislation in 2021 that provides Medigap enrollees with an annual “birthday rule” opportunity to switch to a different plan, starting in 2022.9 It ensures that Medigap enrollees in Nevada have a 60-day window, starting the first day of their birthday month, during which they can switch to any other available Medigap plan that has equal or lesser benefits. Medigap plan change applications submitted during this window are guaranteed-issue, which means the application cannot be rejected and the insurer cannot increase the premium due to medical history (equal or lesser value means the plan can be at the same letter level as the one they have, or any of the lower levels, but not a higher level).
Medigap access for beneficiaries under age 65
Federal rules do not require Medigap insurers to offer coverage to Medicare beneficiaries under the age of 65, so coverage access for this population varies from state to state.
Nevada enacted legislation in 2025 to address this issue.10 Starting in 2026, Medigap insurers in Nevada are required to make all of their policies available to applicants who are under age 65. For Medigap Plans A, B, and D, premiums must be the same as the premiums for an enrollee who is 65. For other Medigap plans, premiums can’t exceed 200% of the age-65 rates. Nevada is offering a one-time enrollment window, from Oct. 1, 2025 to Apr. 1, 2026, so that existing under-65 Medicare beneficiaries can enroll in Medigap coverage.11
What is Medicare Part D?
Original Medicare does not provide coverage for outpatient prescription drugs. More than half of Original Medicare beneficiaries have supplemental medical coverage via an employer-sponsored plan (from a current or former employer or spouse’s employer) and these plans often include prescription coverage.
But Medicare beneficiaries who do not have drug coverage through an employer’s insurance plan need to obtain Medicare Part D prescription coverage (Medicare beneficiaries who are dually-eligible for Medicaid will also have Part D coverage for their drugs). It can be purchased as a stand-alone plan, or as part of a Medicare Advantage plan with integrated Medicare Part D enrollment.
In 2025, there are 16 stand-alone Medicare Part D plans for sale in Nevada, with premiums that start at $0/month.3
As of September 2024, there were 168,431 Medicare beneficiaries in Nevada who were covered under stand-alone Medicare Part D plans.1 Another 294,483 had Part D prescription coverage integrated with their Medicare Advantage plans (this number has been increasing sharply as enrollment in Medicare Advantage plans has grown faster than overall Medicare enrollment in Nevada).1
Medicare Part D enrollment is available during the annual election period from October 15 to December 7. You may change your mind more than once during this window; the last plan you pick will take effect January 1 of the coming year.

What additional resources are available for Medicare beneficiaries and their caregivers in Nevada?
Need help with your Medicare application in Nevada? Got questions about Medicare eligibility in Nevada? You can contact the Nevada State Health Insurance Assistance Program with questions related to Medicare enrollment in Nevada.
The Nevada Aging and Disability Services Division offers a variety of resources for Nevada Medicare beneficiaries.
The Governor’s Office for Consumer Health Assistance (OCHA) is part of the Nevada Department of Health and Human Services, and can provide advice, guidance, and information on a variety of health-related issues.
The Nevada Department of Health and Human Services website also has a resource page with information on programs available to help lower-income Medicare beneficiaries afford their coverage and healthcare.
The Medicare Rights Center is a national resource that includes a website and a call center where consumers throughout the United States can get answers to a wide range of questions about Medicare.

Looking for more information about other options in your state?
Need help navigating health insurance options in Nevada?
Explore more resources for options in NV including ACA coverage, short-term health insurance, dental and Medicaid.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- “Medicare Monthly Enrollment – Nevada.” Centers for Medicare & Medicaid Services Data. Accessed January, 2025. ⤶ ⤶ ⤶ ⤶ ⤶ ⤶ ⤶ ⤶ ⤶
- ”Medicare Advantage 2025 Spotlight: First Look” KFF.org Nov. 15, 2024 ⤶ ⤶ ⤶
- ”Fact Sheet: Medicare Open Enrollment for 2025” (86) Centers for Medicare & Medicaid Services. Sep. 27, 2024 ⤶ ⤶
- U.S. Census Bureau Quick Facts: United States & Nevada.” U.S. Census Bureau, July 2024. ⤶
- “Medicare Monthly Enrollment – US” Centers for Medicare & Medicaid Services Data. Accessed, January, 2025. ⤶
- “The State of Medicare Supplement Coverage” AHIP. May 2025. Accessed Oct. 3, 2025 ⤶
- “2025 Medicare Supplement Insurance Premium Comparison Guide” Nevada Division of Insurance. Accessed Oct. 4, 2025 ⤶
- “Choosing a Medigap Policy” Medicare.gov. Accessed Oct. 4, 2025 ⤶
- “Nevada AB250” BillTrack50. Enacted May 28, 2021 ⤶
- ”Nevada SB292” BillTrack50. Enacted June 6, 2025 ⤶
- ”Bulletin 25-002, Related to; Requiring Medicare Supplement issuers to offer a Medicare Supplement policy for purchase to certain Medicare eligible persons who are below age 65” Nevada Division of Insurance. Sep. 30, 2025 ⤶

