Home > Health Insurance Marketplace > Michigan Heath Insurance Marketplace
Find Michigan Health Insurance Marketplace Coverage for 2026

Compare ACA plans and check subsidy savings from a licensed third-party health insurance agency.

Michigan Marketplace quick facts
Michigan health insurance Marketplace guide
We created this guide, including the FAQs below, to help you choose the right health insurance plan in Michigan for you and your family. An ACA Marketplace plan may be a good choice for many consumers, including those who do not have access to Medicare, Medicaid, or an employer’s health plan.
Michigan’s ACA Marketplace plans – also known as Obamacare plans – are available on the federally-facilitated HealthCare.gov platform.
The Michigan Marketplace provides access to health insurance products from seven private insurers for 2026,4 down from ten in 2025 (details below about carrier participation and premium changes for 2026). As is the case in most states, plan availability varies by area.
Depending on your income and circumstances, you may qualify for financial assistance that can offset the cost of the coverage you obtain through the Michigan Health Insurance Marketplace.
Frequently asked questions about health insurance in Michigan
Who can buy Marketplace health insurance in Michigan?
You can purchase individual/family coverage in the Michigan Marketplace (exchange) if you meet these criteria:5
- You must be a resident of Michigan and lawfully present in the U.S.
- You must not have Medicare coverage.
- You must not be incarcerated.
Although most people are thus eligible to enroll in a Marketplace plan, there are additional criteria to qualify for financial assistance in the Marketplace. To be eligible for subsidies:6
- You must not have access to an affordable employer health plan. Use our employer health plan affordability calculator to see if you may be eligible for subsidies to offset the cost of a Marketplace plan.
- You must not be eligible for Medicaid/CHIP.
- You must not be eligible for premium-free Medicare Part A.7
- If you’re married, you must file a joint tax return.
- You must not be able to be claimed as a dependent on someone else’s tax return.
Subsidy eligibility is also based on how your income compares with the premium for the second-lowest-cost Silver plan in the Marketplace (for premium subsidies) and whether your income is more or less than 250% of the federal poverty level (for cost-sharing reductions).
When can I enroll in an ACA-compliant plan in Michigan?
In Michigan, the open enrollment period for 2026 individual and family insurance ended on January 15, 2026.
For 2026 coverage, enrollments or plan changes now require a special enrollment period (SEP). Most SEPs require a qualifying life event, but American Indians and Alaska Natives can enroll year-round without a qualifying event.
The next open enrollment period, for coverage effective in 2027, will run from November 1, 2026 to December 15, 2026. This will be a shorter enrollment period than the one used for the last several years, due to a federal rule change. And all plans selected during open enrollment will take effect January 1.
Where do I enroll in a Marketplace plan in Michigan?
Michigan residents use HealthCare.gov to enroll in individual and family health plans. You can also sign up with a licensed agent/broker or a Navigator. There is also an option to enroll through various third-party websites authorized by the Centers for Medicare & Medicaid Services.8
How can I find affordable health insurance in Michigan?
In Michigan, consumers may find affordable health insurance by enrolling through the ACA Marketplace (HealthCare.gov).
More than eight out of ten people who enrolled through the Michigan Marketplace for 2026 were eligible for advance premium tax credits (APTC), which reduce the amount that they have to pay each month for their coverage. In 2026, the average premium subsidy in the Michigan Marketplace amounted to $536/month. Subsidy-eligible enrollees in Michigan paid an average net premium of $127/month after subsidies in 2025.1
Michigan Marketplace enrollees can still qualify for APTC in 2026, but the benefits aren’t as robust as they were from 2021 through 2025. The “subsidy cliff” has returned, making premium subsidies unavailable to households earning more than 400% of the federal poverty level. And for those who are still subsidy-eligible, the subsidies don’t cover as much of the total premium as they did in 2025. These changes happened because Congress failed to extend the federal subsidy enhancements that expired at the end of 2025.
People with household incomes up to 250% of the federal poverty level also qualify for cost-sharing reductions (CSR) that may reduce your deductibles and out-of-pocket expenses when you buy a Silver plan.9
Both the premium tax credits and the CSR benefits are only available in Michigan if you enroll in a Marketplace plan.
 Source: CMS.gov1
Source: CMS.gov1
Depending on your household income, you may be eligible for Medicaid/CHIP. Michigan is among the states where Medicaid has been expanded under the ACA, making it easier for low-income adults to qualify for coverage. Learn more about Michigan Medicaid.
How many insurers offer Marketplace coverage in Michigan?
For 2026 coverage, seven insurers offer Marketplace plans in Michigan.4
- Blue Care Network of Michigan
- Blue Cross Blue Shield of Michigan Mutual Insurance Company
- Oscar Insurance Company
- McLaren Health Plan Community
- Meridian Health Plan of Michigan, Inc.
- Priority Health
- UnitedHealthcare Community Plan, Inc.
As is the case in most states, carrier participation varies by area, as not all carriers offer plans in all areas of the state.
There were ten participating insurers for 2025, but as announced in late 2024, UM Health Plan/Michigan Care (formerly Physicians Health Plan or PHP) stopped offering coverage at the end of 2025.10
In addition, HAP CareSource and Molina exited the market in Michigan at the end of 2025.11
Are Marketplace health insurance premiums increasing in Michigan?
The following average rate changes were approved for 2026 for Michigan’s Marketplace insurers,12 amounting to an overall average increase of about 20% before any subsidies are applied.13 (As explained below, average after-subsidy premium increases were much larger, due to the expiration of the federal subsidy enhancements at the end of 2025.)
Michigan’s ACA Marketplace Plan 2026 APPROVED Rate Increases by Insurance Company |
|
|---|---|
| Issuer | Percent Increase |
| Blue Care Network of Michigan | 23.3% |
| Blue Cross Blue Shield of Michigan Mutual Insurance Company | 24% |
| Oscar Insurance Company | 9.3% |
| McLaren Health Plan Community | 19.2% |
| Meridian Health Plan of Michigan, Inc. | 16.9% |
| Molina Healthcare of Michigan, Inc. | Exited market |
| UM Health/Michigan Care (formerly Physicians Health Plan) | Exited market |
| Priority Health | 19.2% |
| UnitedHealthcare Community Plan, Inc. | 25.8% |
| HAP CareSource | Exited market |
Source: Michigan Department of Insurance and Financial Services4
Your plan’s pre-subsidy premium change might be quite different from the average that applies to your insurer, as it also depends on where you live (rates vary by region for each carrier), the specific plan you have, and your age.
The average premium changes described above are for full-price (unsubsidized) premiums. However, most Marketplace enrollees qualify for subsidies, so they do not pay full price.14 For these enrollees, net premium changes depend on changes in their own plan’s price as well as changes in their subsidy amount from one year to the next.
It’s important to understand that because Congress allowed the federal subsidy enhancements to expire at the end of 2025, after-subsidy premiums increased sharply in 2026. So although the average pre-subsidy premium increase was about 20% in Michigan, the increase in after-subsidy premiums was much larger.13
Because the subsidy enhancements expired, the “subsidy cliff” returned in 2026, meaning subsidies are no longer available to households earning more than 400% of the federal poverty level.
And while subsidies are still available to those with income below that level, the subsidies don’t cover as much of the total premium as they did in 2025.
As a result of the expiration of the subsidy enhancements, here are some examples of after-subsidy premium increases in Detroit, Michigan:15
- 40-year-old earning $40,000:
- Lowest-cost plan in 2025 was $78/month
- Lowest-cost plan in 2026 is $128/month
- 60-year-old earning $63,000:
- Lowest-cost plan in 2025 was $287/month
- Lowest-cost plan in 2026 is $740/month (due to the subsidy cliff)
For perspective, here’s an overview of how average premiums have changed in Michigan’s individual/family market over the years:
- 2015: Average decrease of 1%.16
- 2016: Average increase of 6.5%.17
- 2017: Average increase of 16.7%.18
- 2018: Average increase of 26.9%.19
- 2019: Average increase of 1.7%.20
- 2020: Average decrease of 2.1%.21
- 2021: Average increase of 1.1%.22
- 2022: Average increase of 4.7%.23
- 2023: Average increase of 5.5%.24
- 2024: Average increase of 5.3%.25
- 2025: Average increase of 10.5%.26
How many people are insured through Michigan's Marketplace?
497,064 people selected private health plans through the Michigan exchange during the open enrollment period for 2026 coverage.1
This was a drop of about 6% from the year before, when a record-high 531,083 people signed up during the open enrollment period for 2025 coverage.27
The enrollment in 2025 was a significant record high (see graph below for prior year enrollment totals). The increases in recent years were driven in large part by the subsidy enhancements created by the American Rescue Plan and Inflation Reduction Act. The expiration of those subsidy enhancements was the primary reason for the drop in enrollment for 2026.
The enrollment growth in 2024 and 2025 was also due in part to the fact that Medicaid disenrollments resumed in 2023, after being paused for three years during the pandemic (a process known as “unwinding” of the pandemic-era continuous coverage rule). CMS reported that 160,114 Michigan residents transitioned from Medicaid to Marketplace coverage during the unwinding process.28
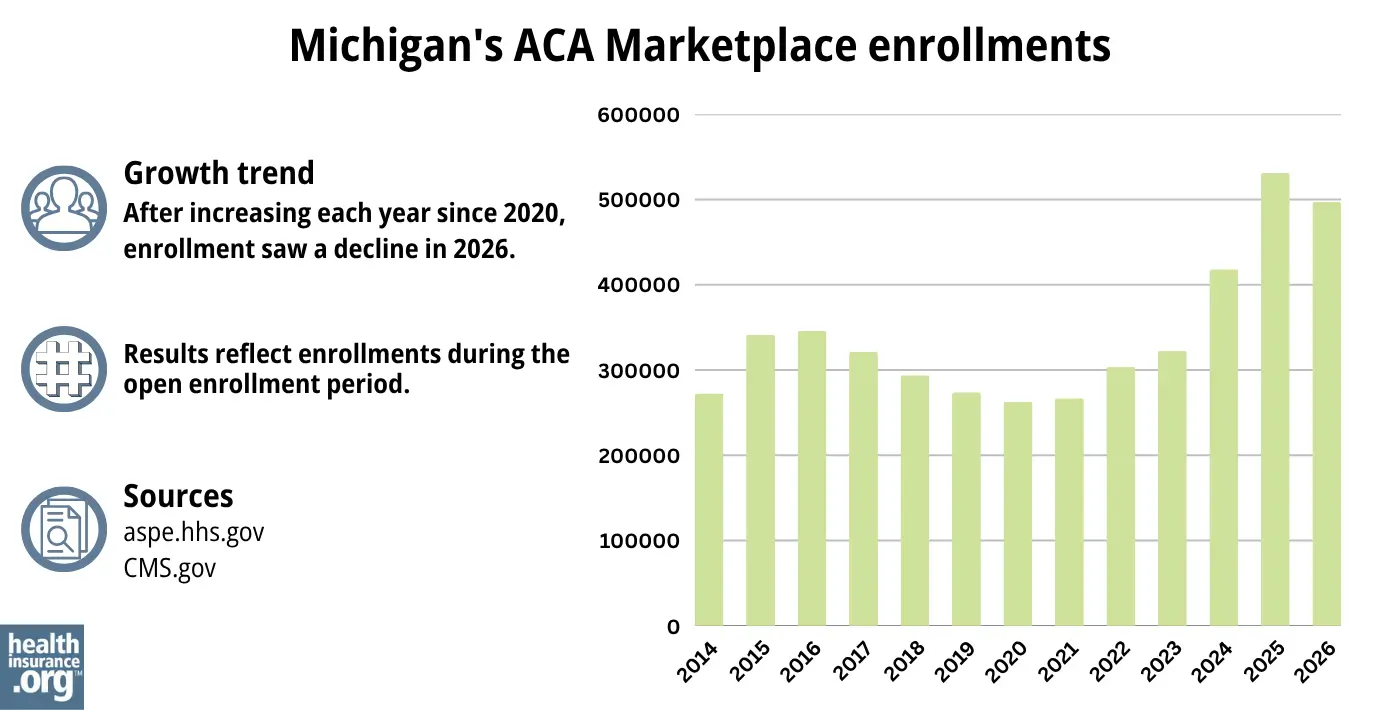
Source: 2014,29 2015,30 2016,31 2017,32 2018,33 2019,34 2020,35 2021,36 2022,37 2023,38 2024,39 202527 20261
What health insurance resources are available to Michigan residents?
- Michigan health insurance Marketplace – HealthCare.gov (800) 318-2596
- Michigan Health Insurance Consumer Assistance Program (HICAP) – (877) 999-6442
- Michigan Department of Insurance and Financial Services – Serves as a resource for Michigan residents with questions or complaints related to health insurance.
- Arab Community Center for Economic & Social Services (ACCESS) – A federally funded Navigator organization that provides outreach and enrollment assistance to Michigan residents who need help obtaining health insurance.
- Michigan Medicare/Medicaid Assistance Program (MMAP) – A local service that provides health benefits counseling and assistance to Medicare beneficiaries, including those who are eligible for both Medicaid and Medicare.
- Medicare Rights Center – A nationwide service (website and call center) that can provide a wide variety of assistance to Medicare beneficiaries who have questions about enrollment, eligibility, benefits, and claims.

Looking for more information about other options in your state?
Need help navigating health insurance options in Michigan?
Explore more resources for options in MI including short-term health insurance, dental, Medicaid and Medicare.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- ”2026 Marketplace Open Enrollment Period Public Use Files” CMS.gov. April 2026 ⤶ ⤶ ⤶ ⤶ ⤶
- ”2026 Michigan Health Insurance Rate Change Requests” Michigan Department of Insurance and Financial Services. July 14, 2025 *The above is based on the most current data available. ⤶
- ”2026 Marketplace Open Enrollment Period Public Use Files” and “Marketplace 2025 Open Enrollment Period Report: National Snapshot” Centers for Medicare & Medicaid Services, April 2026 ⤶
- ”2026 Michigan Health Insurance Rate Change Requests Individual Market (APPROVED)” Michigan Department of Insurance and Financial Services. Oct. 28, 2025 ⤶ ⤶ ⤶
- ”Are you eligible to use the Marketplace?” HealthCare.gov. Accessed Nov. 2, 2025 ⤶
- ”Explaining Health Care Reform: Questions About Health Insurance Subsidies” KFF. October 6, 2023. ⤶
- Medicare and the Marketplace, Master FAQ. Centers for Medicare and Medicaid Services. Accessed November 2, 2025 ⤶
- ”Entities approved to use enhanced direct enrollment” Centers for Medicare and Medicaid Services. Dec. 8, 2025 ⤶
- APTC and CSR Basics. Centers for Medicare and Medicaid Services. June 2023. ⤶
- ”UM Health Plan, Michigan Care to end after 2025” University of Michigan. Nov. 27, 2024 ⤶
- ”Breaking News – Molina Healthcare Announces Significant Changes to 2026 ACA Marketplace Service Area” And “HAP CareSource Exiting 2026 ACA Marketplace” Agility Insurance Services. Sep. 2025 ⤶
- ”2026 Michigan Health Insurance Rate Change Requests” Michigan Department of Insurance and Financial Services. July 14, 2025 ⤶
- ”2026 Final Gross Rate Changes – Michigan: +20.1%; 2 more carriers leaving market (update)” ACA Signups. Oct. 16, 2025 ⤶ ⤶
- ”Effectuated Enrollment: Early 2025 Snapshot and Full Year 2024 Average“ Centers for Medicare and Medicaid Services. July 24, 2025 ⤶
- ”See Plans & Prices” (zip 48127) HealthCare.gov Accessed Nov. 2, 2025 ⤶
- Analysis Finds No Nationwide Increase in Health Insurance Marketplace Premiums. The Commonwealth Fund. December 2014. ⤶
- Health insurance rate hikes approved for 2016: 1% rise for Michigan small businesses. Crains Detroit Business. August 2015. ⤶
- Michigan Department of Insurance and Financial Services Release 2017 Health Plans Rates. TV6. October 2016. ⤶
- Obamacare rates will skyrocket 27% in Michigan in 2018. Detroit Free Press. October 2017. ⤶
- 2019 Rate Hikes. ACA Signups. October 2018. ⤶
- 2020 Rate Changes. ACA Signups. October 2019. ⤶
- 2021 Health Insurance Marketplace Rates Now Available to Preview; Open Enrollment Begins Nov. 1. Office of Governor Gretchen Whitmer. October 2020. ⤶
- Big rate hikes coming in 2022 for some Michigan health insurance plans. Detroit Free Press. October 2021. ⤶
- 2023 Michigan Health Insurance Rate Change Requests Michigan SERFF Filing Access Individual Market (Approved). Michigan Department of Insurance and Financial Services. Accessed November 2023. ⤶
- 2024 Michigan Health Insurance Rate Change Requests. Michigan Department of Insurance and Financial Services. Accessed November 1, 2023. ⤶
- ”Michigan: Preliminary Avg. Unsubsidized 2025 #ACA Rate Change: +10.5%” ACA Signups. (data from Michigan SERFF filings) June 17, 2024 ⤶
- “2025 Marketplace Open Enrollment Period Public Use Files” CMS.gov, May 2025 ⤶ ⤶
- HealthCare.gov Marketplace Medicaid Unwinding Report. Centers for Medicare and Medicaid Services. Data through February 2024. ⤶
- “ASPE Issue Brief (2014)” ASPE ⤶
- “2015 OEP Snapshot Public Use File (ZIP)” CMS.gov ⤶
- “2016 OEP Snapshot Public Use File (ZIP)” CMS.gov ⤶
- “Health Insurance Marketplaces 2017 Open Enrollment Period Final Enrollment Report: November 1, 2016 – January 31, 2017” CMS.gov ⤶
- “Health Insurance Exchanges 2018 Open Enrollment Period Final Report” CMS.gov ⤶
- “Health Insurance Exchanges 2019 Open Enrollment Report” CMS.gov ⤶
- “Health Insurance Exchanges 2020 Open Enrollment Report” CMS.gov ⤶
- “2021 Open Enrollment Report” CMS.gov ⤶
- “2022 Open Enrollment Report” CMS.gov ⤶
- “Health Insurance Marketplaces 2023 Open Enrollment Report” CMS.gov ⤶
- ”HEALTH INSURANCE MARKETPLACES 2024 OPEN ENROLLMENT REPORT” CMS.gov, 2024 ⤶

