Medicare in Virginia
Original Medicare, Medicare Advantage, Part D prescription drug, and Medigap coverage in Virginia

In this article
- Medicare enrollment in Virginia
- Medicare Advantage plan availability and enrollment in Virginia
- Medicare supplement (Medigap) plan availability in Virginia
- Medicare Part D availability and enrollment in Virginia
- What additional resources are available for Medicare beneficiaries and their caregivers in Virginia?

Medicare enrollment in Virginia
Centers for Medicare & Medicaid Services report that 1,741,246 residents were covered by Medicare in Virginia as of January 2026.1
Most beneficiaries become eligible for Medicare enrollment when they turn 65. But after receiving Social Security disability benefits for two years, a person will become eligible for Medicare even if they’re under 65, and Medicare eligibility is also triggered if a person is diagnosed with end-stage renal disease (ESRD) or amyotrophic lateral sclerosis (ALS).
As of early 2026, nearly 161,000 Medicare beneficiaries in Virginia were under the age of 65 – or about 9% of the state’s Medicare population.1 This is roughly the same as the nationwide percentage of Medicare beneficiaries who are under the age of 65.2
Medicare Advantage plan availability and enrollment in Virginia
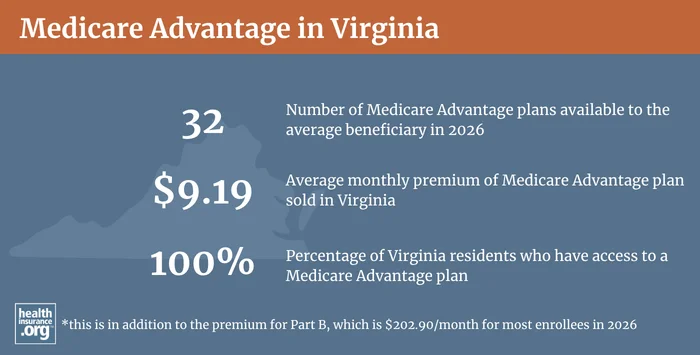
Medicare Advantage plans are offered by private insurers, so plan availability varies from one area to another. There are a total of 143 Medicare Advantage plans offered in Virginia for 2026.3 But plan availability varies from one area to another, and the average Medicare beneficiary in Virginia has access to 25 plans for 2026.4
As of January 2026, total Medicare Advantage plan enrollment in Virginia stood at 683,300 people, amounting to about 39% of Virginia’s Medicare population.5 The rest of Virginia’s Medicare beneficiaries, amounting to 1,057,946 people, had Original Medicare as of January 2026.1
Learn more about Medicare Advantage, Medicare’s annual open enrollment period, and the Medicare Advantage open enrollment period.
Learn about Medicare plan options in Virginia by contacting a licensed agent.



Medicare supplement (Medigap) enrollment and regulations in Virginia
According to AHIP, 429,467 Virginia residents had Medigap plans in 2023,6 supplementing their Original Medicare coverage.
Learn how Medigap plans are regulated and standardized.
The Virginia State Corporation Commission has a Medigap plan comparison tool that residents can use to see available plans and premiums.
Virginia’s Medigap birthday rule
Federal rules only provide a guaranteed-issue right to Medigap coverage during a person’s initial six-month enrollment window (starting when they’re at least 65 and enrolled in Medicare Part A and B), and during limited special enrollment periods. Federal rules do not provide any sort of annual Medigap enrollment window. Federal rules also do not ensure access to Medigap policies for beneficiaries under the age of 65.
But states can establish more enrollment and plan change opportunities. Quite a few states have implemented Medigap “birthday rules” to provide an annual plan change opportunity, and Virginia joined them in 2025.
Since July 2025, Virginia has allowed Medigap enrollees to switch to any other insurer’s version of the policy they already have, during a 60-day window that starts on the enrollee’s birthday.7 The new policy is guaranteed-issue (meaning medical underwriting is not used) as long as it offers the same benefits as the old policy. So for example, someone with Medigap Plan N can use their birthday window to switch to another insurer’s Plan N. Virginia’s birthday rule is due to legislation that the state enacted in 2025.8
Virginia Medigap access for beneficiaries under age 65
Virginia is also among the states where at least some Medigap plans are guaranteed-issue for beneficiaries under age 65.
Since 2021, Virginia has required all Medigap insurers to make at least one policy available to disabled Medicare beneficiaries under age 65, at the same premium charged for age-65 applicants.9 Almost all of the insurers choose to offer Medigap Plan A,10 which is the least comprehensive policy.11 Virginia Medicare beneficiaries under age 65 have a six-month Medigap enrollment window that begins when they’re enrolled in Medicare Part A and Part B.
As of 2024, Virginia’s Medigap access rule was expanded to include beneficiaries with end-stage renal disease (ESRD/kidney failure).7
When enrollees turn 65, they qualify for the federally required Medigap open enrollment period, which allows them access to all Medigap plans (as opposed to Virginia’s rule for under-65 applicants, which only requires each insurer to make one plan available).9
Medicare Part D plan availability and enrollment in Virginia
Medicare beneficiaries can enroll in Medicare Part D prescription drug plans on a stand-alone basis, or obtain Medicare Part D prescription drug coverage integrated with a Medicare Advantage plan. (Almost all Medicare Advantage plans include Medicare Part D prescription drug benefits.)
There are 9 stand-alone Medicare Part D prescription drug plans in Virginia for 2026, with premiums that start at $0 per month.12
As of January 2026, there were 687,071 Virginia beneficiaries with stand-alone Medicare Part D prescription drug coverage, and another 606,432 with Medicare Advantage plans that included integrated Medicare Part D prescription drug coverage.1
Learn how Medicare Part D prescription drug coverage works, what it pays for, how and when to enroll.

What additional resources are available for Medicare beneficiaries and their caregivers in Virginia?
You can contact VICAP (Virginia Insurance Counseling and Assistance Program), with questions related to Medicare eligibility, enrollment, and coverage in Virginia.
The Virginia State Corporation Commission/Bureau of Insurance website offers a variety of information and resources about Medicare Advantage, Medicare Part D, and Medigap plans that are sold in Virginia. They can provide customer service, answer questions, and address complaints about entities they regulate, including health insurance companies and the brokers/agents who sell policies in the state.
The Virginia Insurance Counseling & Assistance Program serves as a resource for Medicare beneficiaries in the state. They can help with questions related to Medicare enrollment, eligibility, or coverage in Virgina.
This guide to Medicaid assistance for Medicare beneficiaries in Virginia is a useful resource that explains the various programs available to people with low income and asset levels, and how to apply for assistance.
Medicare Rights Center is a nationwide service, with a website and call center, where Medicare beneficiaries can get answers to their questions and assistance with understanding the eligibility and enrollment process for Medicare.

Looking for more information about other options in your state?
Need help navigating health insurance options in Virginia?
Explore more resources for options in VA including ACA coverage, short-term health insurance, dental and Medicaid.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- “Medicare Monthly Enrollment – Virginia” Centers for Medicare & Medicaid Services Data. Accessed April 2026. ⤶ ⤶ ⤶ ⤶
- “Medicare Monthly Enrollment – US” Centers for Medicare & Medicaid Services Data. Accessed, April 2026 ⤶
- “Fact Sheet: Medicare Open Enrollment for 2026” Centers for Medicare & Medicaid Services. Sep. 26, 2025 ⤶
- “Medicare Advantage 2026 Spotlight: First Look” KFF.org. Dec. 9, 2025 ⤶
- “Medicare Monthly Enrollment – Virginia” Centers for Medicare & Medicaid Services Data. Accessed Apr. 28, 2026 ⤶
- “The State of Medicare Supplement Coverage” AHIP. May 2025. Accessed Apr. 28, 2026 ⤶
- “Consumer’s Guide to Medigap Insurance in Virginia” Virginia State Corporation Commission. Accessed Oct. 5, 2025 ⤶ ⤶
- “Virginia SB1199” and “Virginia HB2100” BillTrack50. Enacted Mar. 24, 2025 ⤶
- “FAQ: What’s New for Medicare Eligible Individuals Under Age 65” Virginia State Corporation Commission. Accessed Apr. 28, 2026 ⤶ ⤶
- “Find a Medigap policy that works for you” Medicare.gov. Accessed Oct. 5, 2025 ⤶
- “Compare Medigap Plan Benefits” Medicare.gov. Accessed Oct. 5, 2025 ⤶
- “Fact Sheet: Medicare Open Enrollment for 2026” Centers for Medicare & Medicaid Services. Sep. 26, 2025. ⤶

