Home > Health Insurance Marketplace > Nevada Heath Insurance Marketplace
Find Nevada Health Insurance Marketplace Coverage for 2026

Compare ACA plans and check subsidy savings from a licensed third-party health insurance agency.

Nevada ACA Marketplace quick facts
Nevada health insurance Marketplace guide
We’ve created this Nevada health insurance guide and the FAQs below to help you understand the health coverage options and possible financial assistance available to you and your family.
Nevada created its own state-based exchange, called Nevada Health Link, which is overseen by the Silver State Health Insurance Exchange.4 (Nevada had a state-based exchange platform in 2014, switched to the federally-facilitated HealthCare.gov platform for 2015 through 2019, then switched back to a state-based platform in 2020.)
Ten private insurance companies offer Marketplace plans through Nevada Health Link for 2026,5 including three Anthem affiliates and CareSource Nevada, which was new for 2026.6 But Aetna exited the Nevada Marketplace at the end of 2025, as was the case in all states where Aetna participated in 2025, so enrollees with Aetna coverage had to pick a new plan for 2026. (See details below about Nevada Marketplace premium changes for 2026.)
Income-based subsidies are available through Nevada Health Link, making coverage much more affordable than it would otherwise be.
Nevada’s Market Stabilization Program (previously known as the Public Option) took effect in 2026, with “Battle Born State Plans” available for purchase starting in November 2025. This program is described in more detail below, in the section about affordable health insurance in Nevada. Nevada also has a reinsurance program as of the 2026 plan year, which helps to keep unsubsidized premiums lower than they would otherwise be. This is important for people with household income above 400% of the federal poverty level, who are no longer eligible for premium subsidies.
A Nevada Health Link plan can be a great coverage option if you aren’t eligible for Medicare or Medicaid, and also don’t have an offer of affordable health insurance from your employer.
Frequently asked questions about health insurance in Nevada
Who can buy Marketplace health insurance in Nevada?
In order to sign up for private health coverage through Nevada Health Link, you must:7
- Live in Nevada
- Be lawfully present in the United States
- Not be incarcerated
- Not be enrolled in Medicare8
By those rules, most Nevada residents qualify to use the exchange. But a bigger question for most people is financial assistance, and there are a few additional parameters to be eligible for subsidies in Nevada’s exchange.
To qualify for income-based Advance Premium Tax Credits (APTC) or cost-sharing reductions (CSR), you must:
- Not have access to affordable health coverage through an employer. If you have access to an employer’s plan but it seems too expensive, you can use our Employer Health Plan Affordability Calculator to see if you might qualify for premium subsidies via Nevada Health Link.
- Not be eligible for Medicaid or Check Up (CHIP).
- Not be eligible for premium-free Medicare Part A.9
- If married, file a joint tax return.10
- Not be able to be claimed by someone else as a tax dependent.10
Beyond those basic parameters, qualifying for Nevada Health Link subsidies depends on your household income, which is an ACA-specific calculation of MAGI.
When can I enroll in an ACA-compliant plan in Nevada?
The open enrollment period for 2026 health coverage ended on January 15, 2026 in Nevada.
Starting in the fall of 2026, open enrollment will have to end no later than December 31, under new federal rules that were finalized in 2025. And all plans selected during open enrollment will take effect January 1.
Outside of the annual open enrollment window, you may be eligible to enroll if you experience a qualifying life event, such as giving birth or losing other health coverage. Native Americans can enroll year-round, without a specific qualifying life event.
Enrollment in Nevada Medicaid/Check Up (CHIP) is available year-round.
A note about off-exchange enrollment: From 2014 through 2019, Nevada law required plans sold outside the exchange to be available for purchase year-round, with a waiting period of up to 90 days before the coverage would take effect. But Section 56 of Nevada SB482, enacted in 2019,11 eliminated the requirement that health plans be available year-round outside the exchange.
The law took effect October 1, 2019, bringing Nevada’s rules into line with the rest of the country: Both on-exchange and off-exchange, individual major medical plans can only be purchased outside of open enrollment if the applicant qualifies for a special enrollment period (most special enrollment periods are triggered by a qualifying life event).
How do I enroll in a Nevada Marketplace plan?
To enroll in an ACA Marketplace/exchange plan in Nevada, you can:
- Visit Nevada Health Link, which is Nevada’s health insurance exchange (another word for Marketplace). Nevada Health Link is an online platform where you can compare plans, determine whether you’re eligible for financial assistance, and enroll in the plan that best meets your needs.
- Purchase Nevada Health Link coverage with the help of an insurance broker or navigator who is certified with the exchange.12
You can reach the Nevada Health Link call center by calling 1-800-547-2927, Monday to Friday, 9 am to 5 pm.
How can I find affordable health insurance in Nevada?
The Affordable Care Act (ACA) provides income-based subsidies that can help lower your premium payments each month. These subsidies are available to Nevada residents who meet the eligibility requirements and enroll in coverage through Nevada Health Link.
Of the more than 100,000 people who enrolled via Nevada Health Link during the open enrollment period for 2026 coverage, nearly 82% were receiving premium subsidies that reduced their health insurance premiums by an average of $516 per month. After subtracting subsidies, the average enrollee’s premium was about $148 per month.1

Source: CMS.gov1
If your household income is no more than 250% of the federal poverty level, you may also be eligible for cost-sharing reductions (CSR), which will reduce your deductible and other out-of-pocket expenses. These benefits are built into Silver-level plans if the applicant is eligible for them. Of the people who selected plans through Nevada Health Link during the open enrollment period for 2026 coverage, 46% were receiving CSR benefits.1
You can use both APTC and CSR benefits if you’re eligible for both and you select a Silver-level plan through Nevada Health Link (APTC can be used with plans at any metal level, but CSR benefits are only available on Silver plans).
Market Stabilization Program (Public Option) with reinsurance debuted for 2026
Nevada S.B.420, signed into law in June 2021,13 called for the state to create a public option health plan that would be available in the individual market as of 2026. The idea is to create premium reduction targets, similar to the approach that Colorado is using.
Gov. Lombardo, who took office in 2023, was critical of the public option approach, and worked to transform it into a “market stabilization program” instead. Under Lombardo’s plan there is still a public option component, with a quality incentive payment program for insurers to prevent reimbursement cuts for medical providers due to the premium reduction targets. Lombardo’s plan also called for a reinsurance program that would use federal funding to reduce premiums in the individual market.14 (Reinsurance programs were already in use in 17 other states; Nevada became the 18th as of 2026.)
In early 2025, Nevada received approval from CMS for a 1332 waiver for the reinsurance program and the Market Stabilization Program plans (Battle Born State Plans) both of which debuted for the 2026 plan year.15
Depending on your income and circumstances, you may be able to enroll in free or low-cost health coverage through Medicaid or Check Up (Nevada’s CHIP). Learn more about whether you might meet the criteria for Medicaid in Nevada.
How many insurers offer Marketplace coverage in Nevada?
Ten carriers are offering Marketplace plans in Nevada for 2026.5 This includes three Anthem affiliates (one of which was new for 2026), as well as CareSource Nevada, which was also new for 2026.6 But Aetna exited the Nevada Marketplace at the end of 2025, as was the case in all states where Aetna offered Marketplace coverage.
Carrier participation in Nevada’s Marketplace was unchanged from 2024 to 2025, but the 2024 carrier list included two new carriers: Imperial Insurance Companies and Molina Healthcare of Nevada.16
Are Marketplace health insurance premiums increasing in Nevada?
For 2026 coverage, the following average rate changes were approved for the insurers that offer plans in Nevada’s Marketplace,17 amounting to an average rate increase of 22.3% (including carriers that only offer plans outside the exchange)18 before any subsidies are applied.
Nevada’s ACA Marketplace Plan 2026 APPROVED Rate Increases by Insurance Company |
|
|---|---|
| Issuer | Percent Increase |
| CareSource Nevada | New for 2026 |
| HMO Nevada (Anthem Blue Cross Blue Shield) | 25.7% |
| Rocky Mountain Hospital & Medical Service, Inc. (Anthem Blue Cross) | 13% |
| Community Care Health Plans of Nevada (Anthem Blue Cross and Blue Shield) | New for 2026 |
| Health Plan of Nevada | 20.7% |
| SelectHealth | 18% |
| Silver Summit | 26.7% |
| Aetna Health | Exited market |
| Hometown Health Plan | 10.4% |
| Imperial Insurance Companies | 12.8% |
| Molina Healthcare of Nevada | 18.5% |
Source: Nevada Division of Insurance17
It’s important to remember that these average rate increases are for full-price plans, and most enrollees do not pay full price: As of 2025, 87% of Nevada Health Link enrollees were receiving premium subsidies that reduced their monthly payments.19 (That fell to 82% in 2026, after subsidy enhancements expired at the end of 2025.)1
The subsidy amount is different for each enrollee and changes each year depending on the cost of the second-lowest-cost Silver plan relative to the enrollee’s household income. But becasue the American Rescue Plan/Inflation Reduction Act subsidy enhancements were allowed to expire at the end of 2025, subsidies cover a smaller portion of enrollees’ premium in 2026, resulting in higher after-subsidy premiums.
For perspective on the impact of the expiration of the federal subsidy enhancements, here are examples of how premiums changed in Reno, Nevada, after Congress failed to extend the federal subsidy enhancements:20
- 40-year-old earning $40,000:
- Lowest-cost plan in 2025 was $62/month
- Lowest-cost plan in 2026 is $176/month
- 60-year-old earning $63,000:
- Lowest-cost plan in 2025 was $251/month
- Lowest-cost plan in 2026 is $856/month (due to the subsidy cliff)
Here’s an overview of how average full-price premiums have changed over the years in Nevada’s individual/family market:
- 2015: Average increase of 4%.21
- 2016: Average increase of 9.6%.22
- 2017: Average increase of 10.6%.23
- 2018: Average increase of 38.2%.24
- 2019: Average increase of 0.4%.25
- 2020: Average increase of 1.7%.26
- 2021: Average increase of 4.9%.27
- 2022: Average increase of 4.1%.28
- 2023: Average increase of 9.2%.29
- 2024: Average increase increase of 2.8% (3.6% including off-exchange plans).30
- 2025: Average increase of 7.3%31
How many people are insured through Nevada’s Marketplace?
According to Centers for Medicare & Medicaid Services (CMS) data, 104,286 people selected private plans through Nevada Health Link during the open enrollment period for 2026 coverage.1
This was lower than the record-high enrollment the year before (see chart below). Most states experienced a decline in enrollment in 2026,32 due to the expiration of federal subsidy enhancements at the end of 2025, and the resulting increase in premiums.
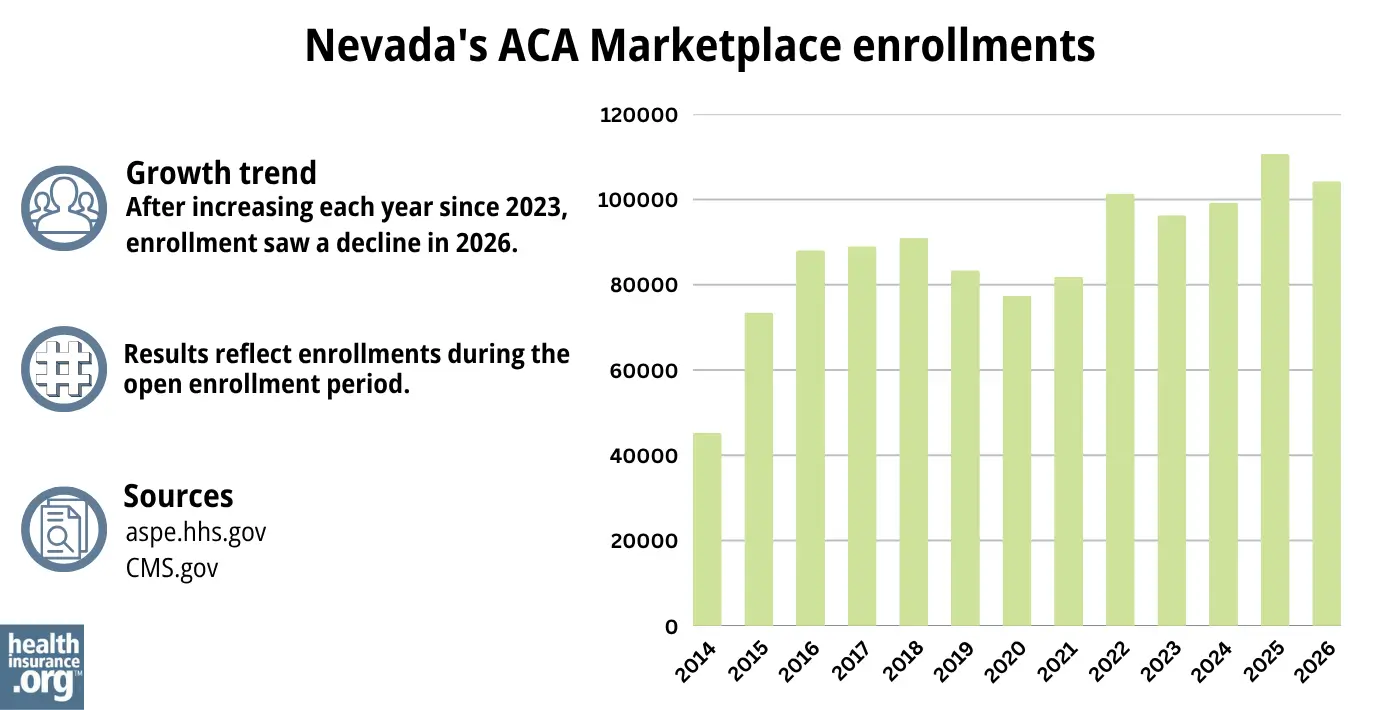
Source: 2014,33 2015,34 2016,35 2017,36 2018,37 2019,38 2020,39 2021,40 2022,41 2023,42 2024,43 202544 20261
What health insurance resources are available to Nevada residents?
Nevada Health Link: This is Nevada’s Marketplace, used to enroll in individual/family health plans and receive income-based subsidies. You can contact Nevada Health Link at 800-547-2927.
Nevada Department of Health and Human Services: The Nevada Department of Health and Human Services (DHHS) administers Medicaid and Check Up (CHIP), as well as other social services programs. You can reach Nevada DHHS by phone at (775) 684-4000 or by email at [email protected]
Nevada Division of Insurance: Regulates Nevada’s insurance industry, and assists consumers and businesses with insurance-related questions and concerns.
Nevada State Health Insurance Assistance Program: A local service for Medicare beneficiaries and their caregivers. Provides information and assistance with questions related to Medicare eligibility, enrollment, and claims.

Looking for more information about other options in your state?
Need help navigating health insurance options in Nevada?
Explore more resources for options in NV including short-term health insurance, dental, Medicaid and Medicare.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- ”2026 Marketplace Open Enrollment Period Public Use Files” CMS.gov. April 2026 ⤶ ⤶ ⤶ ⤶ ⤶ ⤶ ⤶
- ”July 31, 2025 – Nevadans Get a Preview of 2026 Proposed Health Insurance Rate Changes for Upcoming Open Enrollment” Nevada Division of Insurance. July 31, 2025 *The above is based on the most current data available. ⤶
- ”2026 Marketplace Open Enrollment Period Public Use Files” and “Marketplace 2025 Open Enrollment Period Report: National Snapshot” Centers for Medicare & Medicaid Services, April 2026 ⤶
- “Silver State Health Insurance Exchange” nevadahealthlink.com, Accessed August 2023 ⤶
- ”July 31, 2025 – Nevadans Get a Preview of 2026 Proposed Health Insurance Rate Changes for Upcoming Open Enrollment” Nevada Division of Insurance. July 31, 2025 ⤶ ⤶
- ”Broker Brief, Q2, 2025” CareSource. Accessed Aug. 2, 2025 ⤶ ⤶
- ”Who can use Nevada Health Link?” Nevada Health Link, Accessed August 2023 ⤶
- Medicare and the Marketplace, Master FAQ. Centers for Medicare and Medicaid Services. Accessed Apr. 10, 2026 ⤶
- Medicare and the Marketplace, Master FAQ. Centers for Medicare and Medicaid Services. Accessed Apr. 10, 2026 ⤶
- Premium Tax Credit — The Basics. Internal Revenue Service. Accessed Apr. 10, 2026 ⤶ ⤶
- Nevada Senate Bill 482. BillTrack50. Enacted May 2019. ⤶
- ”Find Local Assistance at No Cost to You” Nevada Health Link. Accessed Nov. 15, 2025 ⤶
- Nevada Senate Bill 420. BillTrack50. Enacted June 2021. ⤶
- Governor Joe Lombardo Announces Plan to Transform the Nevada Public Option into Market Stabilization Program. Nevada Governor Joe Lombardo. October 2023. ⤶
- ”Nevada: State Innovation Waiver under Section 1332 of the ACA” Centers for Medicare & Medicaid Services. Jan. 10, 2025 ⤶
- Nevada: *Final* Avg. Unsubsidized 2024 #ACA Rate Changes: +3.8%; Molina & Imperial Joining Market. ACA Signups. October 2023. ⤶
- ”Health Insurance Rate Change Search Results” Nevada Division of Insurance. Accessed Nov. 15, 2025 ⤶ ⤶
- ”2026 Final Gross Rate Changes – Nevada: +22.3% (updated – significant increase from preliminary)” ACA Signups. Sep. 2, 2025 ⤶
- ”Effectuated Enrollment: Early 2025 Snapshot and Full Year 2024 Average” CMS.gov, July 24, 2025 ⤶
- ”Estimate Your Premiums For 2025 and 2026” (zip code 89439) Nevada Health Link. Accessed Nov. 15, 2025 ⤶
- Analysis Finds No Nationwide Increase in Health Insurance Marketplace Premiums. The Commonwealth Fund. December 2014. ⤶
- FINAL PROJECTION: 2016 Weighted Avg. Rate Increases: 12-13% Nationally* ACA Signups. October 2015. ⤶
- Avg. UNSUBSIDIZED Indy Mkt Rate Hikes: 25% (49 States + DC). ACA Signups. October 2016. ⤶
- 2018 Rate Hikes. ACA Signups. October 2017. ⤶
- 2019 Rate Hikes. ACA Signups. October 2018. ⤶
- 2020 Rate Changes. ACA Signups. October 2019. ⤶
- 2021 Rate Changes. ACA Signups. October 2020. ⤶
- 2022 Rate Changes. ACA Signups. October 2021. ⤶
- UPDATED: FINAL Unsubsidized 2023 Premiums: +6.2% Across All 50 States +DC. ACA Signups. Accessed November 2023. ⤶
- OCTOBER 2, 2023 – Discover Your Best Health Plan: 2024 Rates and Options Now Available. Nevada Division of Insurance. October 2023. ⤶
- ”Nevada: *Final* avg. unsubsidized 2025 #ACA rate changes: +7.3% (updated)” ACA Signups. Oct. 4, 2024 ⤶
- ”EXCLUSIVE! FINAL 2026 Open Enrollment Report published: 23.1M QHP selections; 25.0M w/BHPs, down 1.2M y/y (Part 1)” ACA Signups. Mar. 27, 2026 ⤶
- “ASPE Issue Brief (2014)” ASPE, 2015 ⤶
- “Health Insurance Marketplaces 2015 Open Enrollment Period: March Enrollment Report”, HHS.gov, 2015 ⤶
- “HEALTH INSURANCE MARKETPLACES 2016 OPEN ENROLLMENT PERIOD: FINAL ENROLLMENT REPORT” HHS.gov, 2016 ⤶
- “2017 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2017 ⤶
- “2018 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2018 ⤶
- “2019 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2019 ⤶
- “2020 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2020 ⤶
- “2021 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2021 ⤶
- “2022 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2022 ⤶
- “Health Insurance Marketplaces 2023 Open Enrollment Report” CMS.gov, 2023 ⤶
- ”HEALTH INSURANCE MARKETPLACES 2024 OPEN ENROLLMENT REPORT” CMS.gov, 2024 ⤶
- “2025 Marketplace Open Enrollment Period Public Use Files” CMS.gov, May 2025 ⤶

