Home > Health Insurance Marketplace > Connecticut Heath Insurance Marketplace
Find Connecticut Health Insurance Marketplace Coverage for 2026

Compare ACA plans and check subsidy savings from a licensed third-party health insurance agency.

Connecticut ACA Marketplace quick facts
Connecticut health insurance Marketplace guide
This guide, including the FAQs below, can help you find the right health plan in Connecticut for you and your family. For many, an Affordable Care Act (ACA) health insurance Marketplace plan, also called Obamacare, can be an affordable and robust coverage solution.
Connecticut runs its own state-based exchange called Access Health CT. Individual and family plans on the ACA Marketplace are offered by two private insurance companies (one of which offers plans under two separate entities),4 for people who don’t have access to Medicaid, Medicare, or employer-sponsored health insurance. This includes:
- Self-employed people
- Early retirees needing coverage until Medicare
- Workers at small businesses without health benefits
Connecticut is among the states where state-funded subsidies are available in addition to federal subsidies. In Connecticut, this is known as the Covered Connecticut program, and it’s available to adults with household incomes up to 175% of the federal poverty level (FPL).5
In addition, Connecticut is spending $70 million to offset some of the reduction in federal subsidies for 2026, which was announced after the U.S. Senate failed to pass a measure that would have extended the federal subsidy enhancements that are expiring at the end of 2025. Connecticut residents are losing about $295 million in federal subsidies due to the expiration of the federal subsidy enhancements, so Connecticut’s state funding will only make up a portion of the lost federal funding. But they will keep premiums more affordable than they would otherwise have been.6
Access Health CT announced the details of the new state subsidies in early January, and along with an announcement that open enrollment was being extended until January 31, 2026 to give people more time to enroll in 2026 coverage.7 Connecticut’s new state subsidies will:
- fully offset the reduced federal subsidies for enrollees with household income between 100% and 200% of FPL (who aren’t enrolled in Covered Connecticut).
- Offset 50% of the reduction in federal subsidies for enrollees with household income between 400% and 500% of FPL (who are losing all federal subsidies due to the expiration of the federal subsidy enhancements).
Connecticut subsequently announced a special enrollment period, starting February 1 (end date not yet set), for people eligible for the new state-funded subsidies.8
Several other states are using their own funds to offset some or all of the reduction in federal premium subsidies for 2026.
Frequently asked questions about health insurance in Connecticut
Who can buy Marketplace health insurance in Connecticut?
To qualify for Marketplace coverage in Connecticut, you must:9
- Live in Connecticut
- Be a U.S. citizen, national, or lawfully present in the U.S.
- Not be incarcerated
- Not be enrolled in Medicare
Although that makes most people in Connecticut eligible to use the Marketplace, eligibility for financial assistance (premium subsidies and cost-sharing reductions) also depends on income. In addition, to be eligible for financial assistance through Access Health CT, you must:
- Not be eligible for employer-sponsored coverage that’s considered affordable and provides minimum value.
- Not be eligible for HUSKY (Medicaid/CHIP)
- Not be eligible for premium-free Medicare Part A.10
- If married, file a joint tax return with your spouse11 (with very limited exceptions)12
- Not be able to be claimed by someone else as a tax dependent.11
When can I enroll in an ACA-compliant plan in Connecticut?
Connecticut’s open enrollment period for individual and family health plans normally runs from November 1 to January 15. But for 2026 coverage, the deadline has been extended to January 31, 2026.13
Enrollments completed by January 31, 2026 will have coverage effective February 1, 2026.
Starting in the fall of 2026, for coverage effective in 2027, open enrollment will end no later than December 31, and all plans selected during open enrollment will take effect January 1.
Outside of open enrollment, you generally need a qualifying life event, such as losing coverage, getting married, or permanently moving to enroll or make changes. And Connecticut is among several states where pregnancy is considered a qualifying event.14
The qualifying event will trigger a special enrollment period (SEP) that will allow you to sign up for coverage or switch to a different plan.
But some people can sign up without a qualifying life event. For example:
Native Americans can enroll year-round.15
People eligible for the Covered Connecticut program can enroll anytime.16
Anyone eligible for HUSKY (Medicaid/CHIP) in Connecticut can also enroll year-round.
How do I enroll in a Marketplace plan in Connecticut?
There are multiple ways to enroll in an ACA Marketplace plan in Connecticut:17
- Online: Go to AccessHealthCT.com to create an account and apply.
- Phone: Contact the Call Center at 855-805-4325.
- Get help from a navigator, certified application counselor, or agent/broker certified with Access Health CT. These individuals can provide help over the phone, in-person, or online.
How can I find affordable health insurance in Connecticut?
You can find affordable individual and family health plans in Connecticut through AccessHealthCT.com, the state’s ACA exchange.
Access Health CT is where you can:
- Shop, compare, and sign up for health and dental plans
- Qualify for financial help to lower your costs
- Enroll in HUSKY (Medicaid/CHIP) or the Covered Connecticut Program if eligible
Almost eighty percent of Access Health CT enrollees receive subsidies, saving an average of $952 each month on their 2026 premiums.1 These subsidies are called Advance Premium Tax Credits (APTC). Subsidy-eligible Connecticut Marketplace enrollees pay an average of $100/month in after-subsidy premiums in 2026.1
If your income is no more than 250% of the federal poverty level, you may qualify for cost-sharing reductions (CSR) to lower your deductibles and out-of-pocket costs.18
If you qualify for Covered Connecticut, the state will cover your portion of the monthly premiums and any expenses related to cost-sharing, such as your deductibles, copays, and co-insurance.
Covered Connecticut is available to enrollees with household income up to 175% of the poverty level (they must also not be eligible for Medicaid, which is available up to 138% of the poverty level).
Under the Covered Connecticut program, eligible enrollees must select a silver plan through Access Health CT and accept all of the federal subsidies available to them. Covered Connecticut then pays any remaining premiums and cost-sharing, resulting in a plan that has a $0 premium and $0 cost-sharing.19
As explained below, Connecticut is funding additional state subsidies for 2026, designed to mitigate some of the impact of the expiration of federal subsidy enhancements at the end of 2025.7

Source: CMS.gov1
How many insurers offer Marketplace coverage in Connecticut?
Three insurance companies offer individual/family coverage through the Connecticut exchange:20
- Anthem
- ConnectiCare Benefits
- ConnectiCare Insurance Company
Are Marketplace health insurance premiums increasing in Connecticut?
For 2026, the following average rate increases were approved for the insurers that offer individual/family health coverage via Access Health CT, amounting to an overall average rate increase of 16.8%, before subsidies are applied.4
Connecticut’s ACA Marketplace Plan 2026 APPROVED Rate Increases by Insurance Company |
|
|---|---|
| Issuer | Percent Increase |
| Anthem | 13.6% |
| ConnectiCare Benefits | 20.6% |
| ConnectiCare Insurance Company | 20.3% |
Source: Connecticut Insurance Department21
The rate changes noted above apply to full price premiums, before subsidies are applied. Most enrollees receive subsidies, but those subsidies are no longer available to anyone with a household income over 400% of the federal poverty level in 2026, and aren’t covering as much of the premium for everyone else, due to the failure of Congress to extend the federal subsidy enhancements that expired at the end of 2025.
But Connecticut Gov. Ned Lamont announced in December 2025, soon after the U.S. Senate failed to pass a bill that would have extended the subsidy enhancements, that Connecticut would use $70 million to offset some of the $295 million reduction in federal subsidies for 2026. This will help to keep 2026 net premiums in Connecticut more affordable than they would otherwise have been.6
Access Health CT announced the details of the new state subsidies in early January, 2026. The new state subsidy program will:7 Connecticut’s new state subsidies will:
- fully cover the reduction in federal subsidies for enrollees with household income between 100% and 200% of FPL (who aren’t enrolled in Covered Connecticut).
- cover 50% of the reduction in federal subsidies for enrollees with household income between 400% and 500% of FPL (the expiration of the federal subsidy enhancements resulted in these enrollees losing all of their federal subsidies).
For perspective, here’s an overview of how average unsubsidized premiums have changed in Connecticut’s individual/family market over the years:
- 2015: Average decrease of 1%.22
- 2016: Average increase of 3.5%.23
- 2017: Average increase of 24.8%.24
- 2018: Average increase of 28.4%.25
- 2019: Average insurance of 2.72%.26
- 2020: Average increase of 3.65%.27
- 2021: Average increase of 0.01%.28
- 2022: Average increase of 5.6%.29
- 2023: Average increase of 12.9%.30
- 2024: Average increase of 9.4%31
- 2025: Average increase of 5.9%32
How many people are insured through Connecticut’s Marketplace?
A record-high of more than 156,745 people enrolled in private plans through the Connecticut exchange during the open enrollment period for 2026 coverage.1
The enrollment growth was driven in part by the continued subsidy enhancements under the American Rescue Plan and Inflation Reduction Act, as well as the “unwinding” of the pandemic-era Medicaid continuous coverage rule, with some people transitioning from Medicaid to a Marketplace plan.
Access Health CT noted in 2024 that the enrollment growth was partially due to additional outreach and enrollment efforts by the Marketplace and local brokers.33 And 2025 enrollment ended up substantially higher than 2024 enrollment had been (see chart belot).
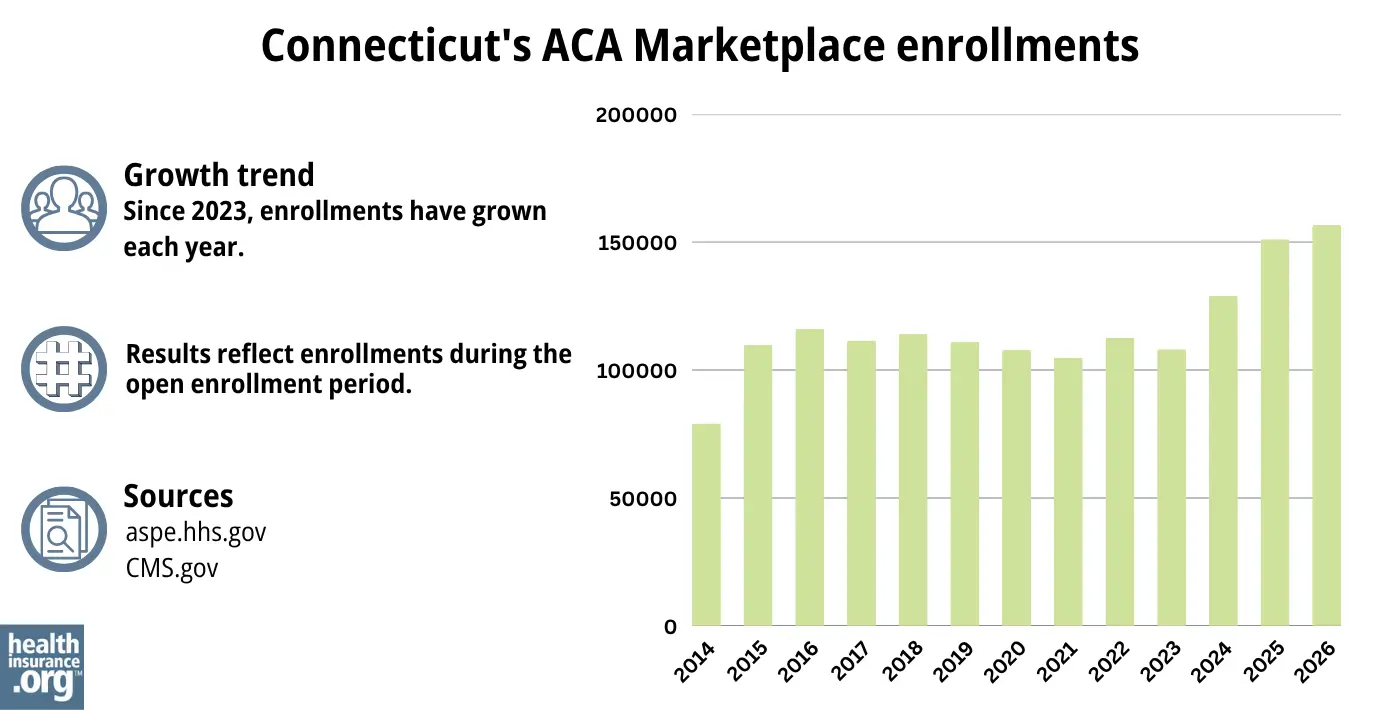
Source: 2014,34 2015,35 2016,36 2017,37 2018,38 2019,39 2020,40 2021,41 2022,42 2023,43 2024,44 202545 20261
What health insurance resources are available to Connecticut residents?
Access Health CT
This website is used by Connecticut residents to sign up for private individual market or small-group coverage and income-based Medicaid/CHIP coverage.
Connecticut CHOICES Program
Offers free enrollment counseling and assistance for older adults, people with disabilities, and their caregivers.
Connecticut Insurance Department
Regulates and licenses the state’s health insurance companies, brokers, and agents. They also address inquiries and complaints from consumers about entities under their regulation.
Husky Healthcare
Provides health coverage for Connecticut residents with lower and moderate incomes.
Medicare Rights Center
This nationwide service offers help and information to Medicare beneficiaries and their caregivers.

Looking for more information about other options in your state?
Need help navigating health insurance options in Connecticut?
Explore more resources for options in CT including short-term health insurance, dental, Medicaid and Medicare.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- ”2026 Marketplace Open Enrollment Period Public Use Files” CMS.gov. April 2026 ⤶ ⤶ ⤶ ⤶ ⤶ ⤶
- ”Health Insurance Rates for 2026” Connecticut Insurance Department. Accessed Aug. 25, 2025 *The above is based on the most current data available. ⤶
- ”2026 Marketplace Open Enrollment Period Public Use Files” and “Marketplace 2025 Open Enrollment Period Report: National Snapshot” Centers for Medicare & Medicaid Services, April 2026 ⤶
- ”Health Insurance Rates for 2026” Connecticut Insurance Department. Accessed Aug. 25, 2025 ⤶ ⤶
- Covered Connecticut Program. Access Health CT. Accessed Dec. 14, 2025 ⤶
- ”Lamont pledges $70M for health care after US Senate deadlocks” CT Mirror. Dec. 11, 2025 ⤶ ⤶
- ”Deadline to Enroll in Health and Dental Coverage Through Access Health CT Has Been Extended to Jan. 31” Access Health CT. Jan. 2, 2026 ⤶ ⤶ ⤶
- ”Access Health CT to Offer Special Enrollment Period for Eligible Customers to Enroll in Coverage with New State Subsidy” Access Health CT. Jan. 23, 2026 ⤶
- ”What is Access Health CT?” Access Health CT. Accessed Dec. 14, 2025 ⤶
- Medicare and the Marketplace, Master FAQ. Centers for Medicare and Medicaid Services. Accessed Dec. 14, 2025 ⤶
- Premium Tax Credit — The Basics. Internal Revenue Service. Accessed Dec. 14, 2025 ⤶ ⤶
- Updates to frequently asked questions about the Premium Tax Credit. Internal Revenue Service. February 2024. ⤶
- “Open Enrollment Dates and Hours of Operation” Access Health CT. Accessed Jan. 5, 2026 ⤶
- Special Enrollment Periods. Access Health CT. Accessed Dec. 14, 2025 ⤶
- “Who doesn’t need a special enrollment period?“ healthinsurance.org, Accessed August 2023 ⤶
- ”Covered Connecticut Program” Connecticut.gov. Accessed Dec. 14, 2025 ⤶
- “Get Help” Access Health CT, Accessed Dec. 14, 2025 ⤶
- “Federal Poverty Level (FPL)” HealthCare.gov, 2023 ⤶
- Covered Connecticut Program. Access Health CT. Accessed November 2023. ⤶
- ”Insurance Companies” Access Health CT. Accessed Dec. 14, 2025 ⤶
- ”Health Insurance Rates for 2026” Connecticut Insurance Department. Accessed Dec. 14, 2025 ⤶
- Analysis Finds No Nationwide Increase in Health Insurance Marketplace Premiums. The Commonwealth Fund. December 2014. ⤶
- Connecticut: *Approved* 2016 Weighted Avg. Rate Hikes: +3.5%, -2.9% Sm. Group. ACA Signups. September 2015. ⤶
- Avg. UNSUBSIDIZED Indy Mkt Rate Hikes: 25% (49 States + DC). ACA Signups. October 2016. ⤶
- 2018 Rate Hikes. ACA Signups. October 2017. ⤶
- Health Insurance Rates for 2020. Connecticut Insurance Department. September 2018. ⤶
- Health Insurance Rates for 2020. Connecticut Insurance Department. September 2019. ⤶
- Health Insurance Rates for 2021. Connecticut Insurance Department. September 2020. ⤶
- Health Insurance Rates for 2022. Connecticut Insurance Department. September 2021. ⤶
- Many CT health insurance plans will see double-digit rate hikes in 2023. Connecticut Mirror. September 2022. ⤶
- “Health Insurance Rates for 2024” Connecticut Insurance Department, Accessed September 2023 ⤶
- ”Health Insurance Rates for 2025” Connecticut Insurance Department. Sep. 6, 2024 ⤶
- ”Record Number 0f Connecticut Residents Enroll in Health Insurance Plans Through Access Health CT for 2024” Access Health CT. January 18, 2024. ⤶
- “ASPE Issue Brief (2014)” ASPE, 2015 ⤶
- “Health Insurance Marketplaces 2015 Open Enrollment Period: March Enrollment Report”, HHS.gov, 2015 ⤶
- “HEALTH INSURANCE MARKETPLACES 2016 OPEN ENROLLMENT PERIOD: FINAL ENROLLMENT REPORT” HHS.gov, 2016 ⤶
- “2017 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2017 ⤶
- “2018 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2018 ⤶
- “2019 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2019 ⤶
- “2020 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2020 ⤶
- “2021 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2021 ⤶
- “2022 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2022 ⤶
- “2023 Marketplace Open Enrollment Period Public Use Files” CMS.gov, March 2023 ⤶
- ”HEALTH INSURANCE MARKETPLACES 2024 OPEN ENROLLMENT REPORT” CMS.gov, 2024 ⤶
- “2025 Marketplace Open Enrollment Period Public Use Files” CMS.gov, May 2025 ⤶

