Who's paying for the ACA's Medicaid expansion? The federal government – or each state?
The cost of Medicaid expansion is paid by both the state and federal government, but the federal government pays 90% of the cost. The federal government paid the full cost of expansion for the first three years (2014 through 2016). The federal government's portion gradually dropped to 90% by 2020, and it now stays there permanently unless legislative changes are made.
That's in contrast to traditional Medicaid (the non-expansion population), where states can pay up to 50% of the cost.
For states that expand Medicaid, the federal funding they receive to cover the expansion population (adults with income up to 138% of the federal poverty level) will always dwarf the amount that the state has to spend. And although states have to cover 10% of the cost of Medicaid expansion, their net spending can be much less than that — even negative in some cases. There are a few reasons for that:1
- Medicaid expansion allows some states to shift certain populations from traditional Medicaid eligibility to the Medicaid expansion category, where the federal government pays a much larger portion of the cost.
- Medicaid expansion reduces the need for state spending on uncompensated care and mental health/substance abuse treatment for low-income residents, since fewer low-income people in the state are uninsured. It also allows states to use the Medicaid program to cover the cost of inpatient medical care for incarcerated people.
- The cost of Medicaid expansion can sometimes be offset by increased revenues for the state, including revenue from taxes/fees assessed on hospitals, medical providers, and insurers, increased tax revenue due to economic growth linked to Medicaid expansion, and premiums that a few states require some Medicaid expansion enrollees to pay.
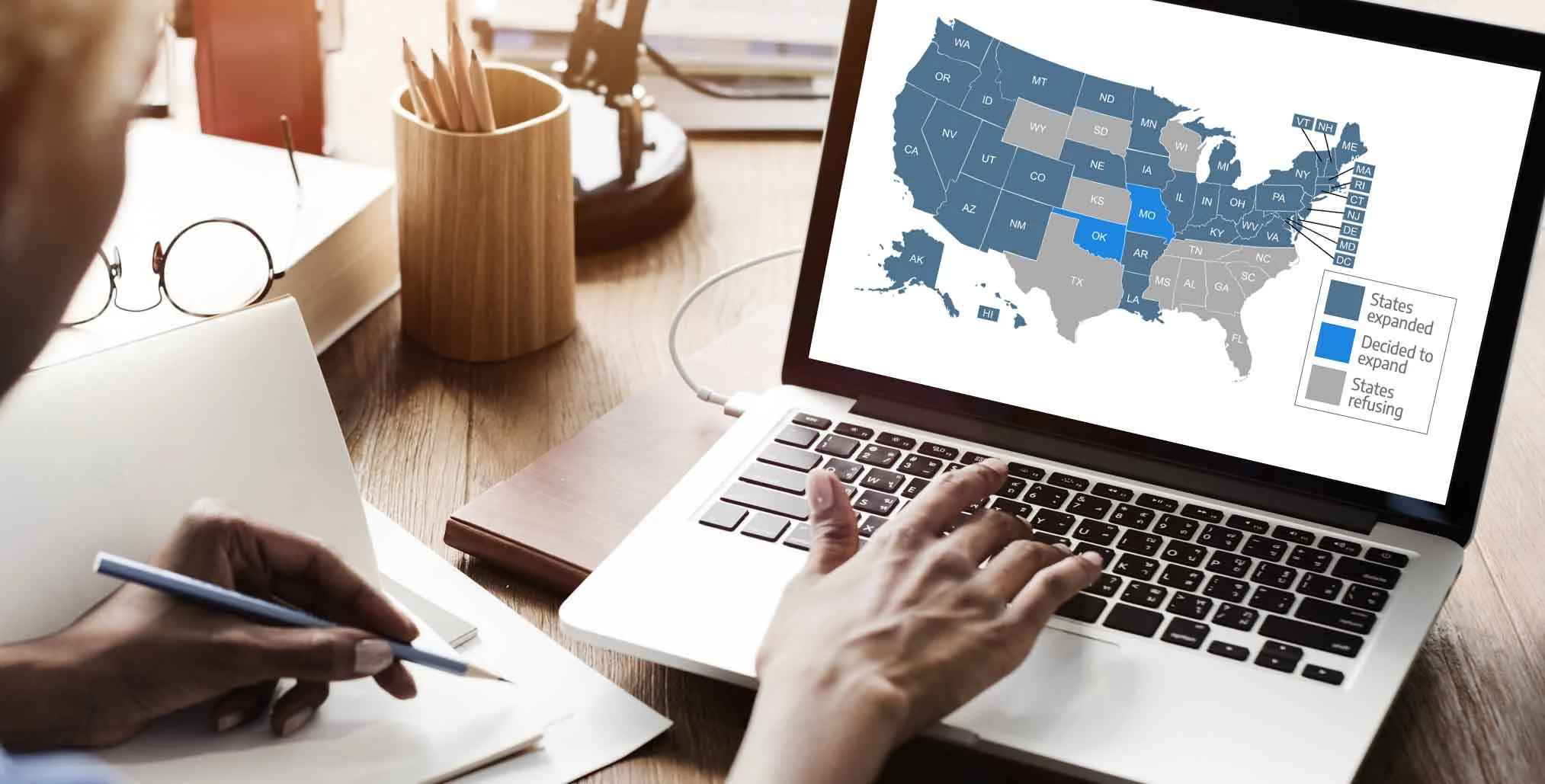
As of 2025, Medicaid expansion has been adopted by 40 states and the District of Columbia. Ten states have not expanded Medicaid. Two of them — Wisconsin and Georgia — have a partial Medicaid expansion, with coverage available up to 100% of the poverty level. But Georgia's program includes a work requirement, so enrollment has remained very low.2
Georgia and Wisconsin do not receive the enhanced federal funding for Medicaid expansion (ie, 90% of costs covered by the federal government) because states are required to fully expand Medicaid to 138% of the poverty level to qualify for the enhanced federal funding.
Footnotes
- "The Impact of Medicaid Expansion on States’ Budgets" The Commonwealth Fund. May 5, 2020 ⤶
- "Pathways Monitoring Reports, October 2024" Georgia Department of Community Health. Accessed June 10, 2025 ⤶



