What is a Medicaid work requirement?
Under a Medicaid work requirement, certain Medicaid enrollees must participate in “community engagement” activities1 (work, school, job training, volunteering, etc.) in order to maintain their health coverage. (“Medicaid work requirement” and “Medicaid community engagement requirement” both mean the same thing.)
In states that have expanded Medicaid, Medicaid provides coverage for adults ages 19 to 64, with household incomes up to 138% of the federal poverty level. This is the “expansion population.”
Under H.R.1 – the “One Big Beautiful Bill Act” enacted in 2025 – there will be a nationwide work requirement for the Medicaid expansion population, starting in 2027. The work requirement will apply to the partial Medicaid expansion programs in Georgia and Wisconsin, as well as the Medicaid expansion programs that are in place in 40 states and Washington, D.C.2
Under this requirement, non-exempt Medicaid expansion enrollees will have to work, volunteer, or attend school for 80 hours per month. As described below, some states are implementing this ahead of schedule, in 2026. States may also be able to delay the implementation until after the end of 2028, if they can show that they are “demonstrating a good faith effort to comply” with the new rules.3
For perspective, there were nearly 20 million people covered under Medicaid expansion in mid-2025, and more than 45 million people enrolled in traditional Medicaid.2 The traditional Medicaid population includes children, people over 65, people who are disabled, pregnant women, and parents/caretakers of minor children. But the H.R.1 work requirement is only applicable to the expansion population, and not to the traditional Medicaid population.
The federal work requirement will not apply to some members of the Medicaid expansion population, including American Indians, parents of children under the age of 14, and people who qualify for various other exemptions.4
But those who are not exempt will have to provide documentation of their community engagement activities (work, school, volunteering, etc.) or their income. Failure to do so will result in loss of Medicaid coverage.
The Congressional Budget Office (CBO) projects that about 18.5 million people will be subject to the work requirement, and that about 5.2 million people will lose their Medicaid coverage as a result of the work requirement.5
Although more than nine out of ten Medicaid expansion enrollees either have a job, are looking for a job, are students, are caring for family members, or are in fair/poor health or disabled, coverage losses would include some of those people due to failure to obtain exemptions or comply with reporting requirements.6
Note: South Carolina has not expanded Medicaid. But the state has submitted a proposal to CMS that, if approved, calls for the eligibility income limit for the parent/caretaker population to be increased to 100% of FPL (closing the “coverage gap” for parents/caretakers), but with a work requirement for those who would be newly eligible.7 This is separate from the H.R.1 Medicaid work requirement, as there is no Medicaid expansion population in South Carolina.
Are Medicaid work requirements in effect in any states in 2026?
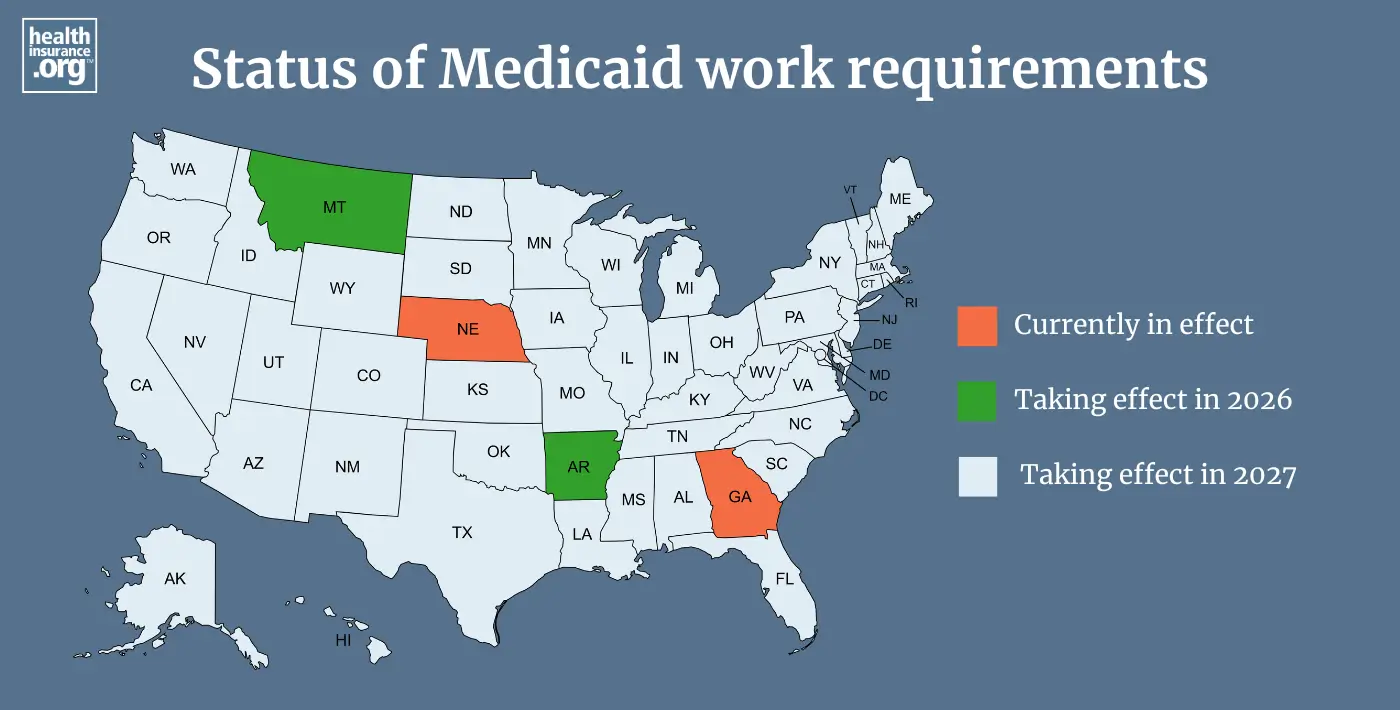
Although Medicaid expansion work requirements won’t take effect in most states until January 2027, some states have or will have work requirements for their Medicaid expansion populations in 2026. They include:
- Georgia, for the state’s partial Medicaid expansion population (Georgia Pathways to Coverage).8
- Nebraska, starting on May 1, 2026, for the Medicaid expansion population.9
- Montana, starting on July 1, 2026, for the Medicaid expansion population.10
- Arkansas, starting on July 1, 2026, for the Medicaid expansion population. But this will be a “soft implementation” and people will not be disenrolled or denied coverage for noncompliance until January 2027.11
- Iowa, starting December 1, 2026, for the Medicaid expansion population.12
Do Medicaid work requirements increase the number of people with jobs?
No, Medicaid work requirements do not result in more people working. This is due in large part to the fact that most people with Medicaid are either already working, would qualify for an exemption from a work requirement, or face various barriers to employment.13
According to a 2023 study by the Congressional Budget Office, Medicaid work requirements result in fewer people with Medicaid, most of whom become uninsured after losing Medicaid. And they result in significant administrative expenses for a state’s Medicaid program.14
What is the history of Medicaid work requirements?
Georgia’s Medicaid work requirement took effect in July 2023, for people who want to enroll in the state’s partial Medicaid expansion, which is called Georgia Pathways to Coverage. This program is available to adults under age 65 with household income below the federal poverty level, but only if they’re working at least 80 hours per month and reporting their work to the state. (Over time, Georgia has scaled back the reporting requirement and is only verifying compliance at the time of application and renewals.)15
By March 2026, nearly three years after the program began, only 16,183 people were enrolled in Georgia Pathways.16 This extremely low enrollment is due in large part to the work requirement and associated paperwork.15 And the majority of the money the government has spent on the program has gone to administration rather than healthcare expenses,17 which is a cautionary tale as we head toward a nationwide Medicaid expansion work requirement under H.R.1.18
The Trump administration approved Georgia’s Medicaid work requirement in 2020, but the Biden administration subsequently revoked the approval. In 2022, however, a U.S. District Judge ruled that HHS acted in an “arbitrary and capricious” manner in revoking Georgia’s Medicaid work requirement approval. This cleared the way for Georgia to implement its Medicaid work requirement in conjunction with a partial expansion of Medicaid, starting in mid-2023.19
In April 2025, Georgia submitted its renewal proposal for the Georgia Pathways waiver to CMS,20 which was approved a few months later, allowing the Pathways to Coverage program to remain in place through the end of 2026. (After that, it will be replaced with the federal H.R.1 work requirement rules.)21 Notably, the waiver extension no longer includes monthly reporting of hours worked. Instead, enrollees must prove their work hours when they first enroll, and at each annual renewal, plus “periodic and random audits” to ensure compliance. Georgia noted in the extension proposal that the state had already stopped disenrolling people who failed to report their work hours.20
Although several states received approval for Medicaid work requirements under the first Trump administration, most were either never implemented or weren’t in effect long enough for anyone to lose coverage. Arkansas was the only state that disenrolled people from Medicaid due to an implemented work requiremen.. About 18,000 people lost coverage in Arkansas in 2018 as a result of the state’s short-lived work requirement, which was only in effect from June 2018 to March 2019, when it was overturned by a judge.22
Arkansas officials have noted that the state’s updated work requirement, set to “soft” launch in July 2026, “reflects lessons learned” from the 2018-2019 efforts to implement a Medicaid expansion work requirement.23 Under the new program, Arkansas will make use of data matching whenever possible, reducing the number of people who have to report information to the state. The state plans to communicate with enrollees during the second half of 2026, letting them know what the data matching process indicates about whether they’re in compliance with the work requirement, and clarifying that the work requirement to maintain coverage will be enforced starting in January 2027.24
In addition to Arkansas, four other states (Indiana, Michigan, New Hampshire, and Utah) implemented Medicaid work requirements between 2018 and 2020. But those work requirements weren’t in effect long enough to result in coverage losses.
In 2021, the Biden administration officially withdrew federal approval for all of the previously approved Medicaid work requirement waivers, including those for states where the work requirement had not yet taken effect.25
Footnotes
- “CMS announces new policy guidance for states to test community engagement for able-bodied adults” Centers for Medicare & Medicaid Services. Jan. 11, 2018 ⤶
- “Tracking Implementation of the 2025 Reconciliation Law Medicaid Work Requirements” KFF.org. Mar. 30, 2026 ⤶ ⤶
- “H.R. 1, the One Big Beautiful Bill Act” (Section 71119). Congress.gov. Enacted July 4, 2025 ⤶
- “H.R. 1, the One Big Beautiful Bill Act” (Section 71119(a)(9)(a)(ii)). Congress.gov. Enacted July 4, 2025 ⤶
- “Estimated Effects on the Number of Uninsured People in 2034 Resulting From Policies Incorporated Within CBO’s Baseline Projections and H.R. 1, the One Big Beautiful Bill Act” Congressional Budget Office. June 4, 2025 ⤶
- “How Many Expansion Adults Could Lose Medicaid Under Federal Work Requirements?” Robert Wood Johnson Foundation. Mar. 17, 2025 ⤶
- “Public Notice for South Carolina Department of Health and Human Services Palmetto Pathways to Independence Demonstration Waiver” South Carolina DHHS. Accessed Apr. 27, 2026 ⤶
- “Eligibility Criteria” Georgia Pathways to Coverage. Accessed Apr. 27, 2026 ⤶
- “Work Requirements” Nebraska Department of Health & Human Services. Accessed Apr. 27, 2026 ⤶
- “Changes to Medicaid” Montana DPHHS. Accessed Apr. 27, 2026 ⤶
- “DHS to launch soft implementation of work and community engagement requirement starting July 1” Arkansas Department of Human Services. Feb. 23, 2026 ⤶
- "Iowa Health and Wellness Plan (IHAWP) Community Engagement Requirements" Iowa Health & Human Services. Accessed May 11, 2026 ⤶
- “Medicaid Work Requirements Would Do Little or Nothing to Increase Employment, but Would Harm People’s Health” Urban Institute. May 15, 2023 ⤶
- “Making Sense of Medicaid Work Requirements” KFF.org. Dec. 17, 2024 ⤶
- “Georgia Touts Its Medicaid Experiment as a Success. The Numbers Tell a Different Story” ProPublica. Feb. 19, 2025 ⤶ ⤶
- “Georgia Pathways Data Tracker” GeorgiaPathways.org. Mar. 31, 2026 ⤶
- “Georgia’s Medicaid Work Requirement Program Spent Twice as Much on Administrative Costs as on Health Care, GAO Says” ProPublica. Sep. 24, 2025 ⤶
- “CMS’s Georgia Waiver Extension Underscores the Failure of Medicaid Work Requirements” Georgetown University Center for Children and Families. Oct. 30, 2025 ⤶
- “Case Summary: Georgia v. Brooks-LaSure--Medicaid Work Requirements Reappear” National Health Law Program. Nov. 4, 2022 ⤶
- “Georgia Pathways to Coverage” Centers for Medicare & Medicaid Services. Accessed July 14, 2025 ⤶ ⤶
- “CMS Approves Georgia Pathways to Coverage™ Extension, Further Validates Innovative Approach” Georgia Governor Brian Kemp. Sep. 25, 2025 ⤶
- “5 Key Facts About Medicaid Work Requirements” KFF.org. Feb. 18, 2025 ⤶
- “Pathway to Prosperity Waiver” Arkansas Governor Sarah Huckabee Sanders. Jan. 28, 2025 ⤶
- “Arkansas to “soft launch” upcoming Medicaid work requirement checks” Arkansas Advocate. Feb, 20, 2026 ⤶
- “Biden Administration Withdraws Medicaid Work Requirements Guidance and More” Georgetown University, McCourt School of Public Policy. Feb. 17, 2021 ⤶


