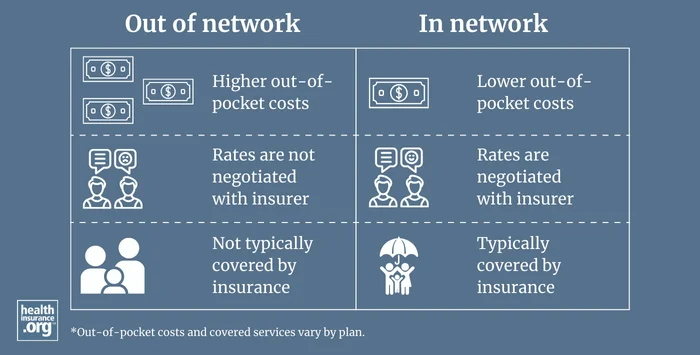
What does out-of-network mean?
This phrase usually refers to physicians, hospitals or other healthcare providers who do not participate in a health plan's provider network. This means that the provider has not signed a contract agreeing to accept the insurer's negotiated prices.
Is out-of-network care covered by health insurance?
Depending on an individual's health insurance plan, expenses incurred for services provided by out-of-network health professionals may not be covered at all unless it's an emergency. Or they may be covered but with higher out-of-pocket costs than the member would pay for the same care received from an in-network provider. The federal cap on out-of-pocket costs only applies to in-network care (and only care that's considered an essential health benefit). So out-of-pocket costs for covered out-of-network care can be much higher, or even unlimited.
And it's important to understand that out-of-network providers can and do balance bill patients for the remainder of the charges after the insurance company has paid its share. In-network providers have agreed to accept the insurance company's payment (plus the patient's pre-determined cost-sharing amount) as payment in full, but out-of-network providers have not signed any sort of agreement with the insurer. However, the No Surprises Act protects patients from surprise balance bills in emergencies or situations where the patient unknowingly received care from an out-of-network provider while at an in-network facility.
Learn more about HMOs, PPOs, EPOs, and POS plans, and what these managed care designations mean in terms of out-of-network coverage.
Health insurance plans that cover out-of-network care are much less common in the individual market1 than they are in the employer-sponsored group market.2
Footnotes
- “Insights into the 2022 individual health insurance market” McKinsey.com, Aug. 23, 2022 ⤶
- "2024 Employer Health Benefits Survey" KFF.org. Oct. 9, 2024 ⤶


