Medicaid eligibility and enrollment in Hawaii

Hawaii now provides continuous Medicaid coverage for kids until age 6

Who is eligible for Medicaid in Hawaii?
Hawaii’s Medicaid/CHIP is called Med-QUEST (QUEST stands for Quality care, Universal access, Efficient utilization, Stabilizing costs, and Transforming the way health care is provided to recipients).
Hawaii’s Medicaid eligibility levels for children are much higher than the national average and about average for pregnant women and parents (these eligibility limits include a built-in 5% income disregard that’s used for income-based (MAGI) Medicaid eligibility determinations):
- Children ages 0-18 qualify with family income levels up to 313% of the federal poverty level (FPL). This includes new provisions, approved by the federal government in late 2024,1 to allow children to have continuous coverage — meaning they don’t need to have their eligibility redetermined each year:
- Children who are determined eligible before age 6 are continuously eligible until they turn 6.
- Children ages 6 to 19 only need their eligibility redetermined once every two years.
- Pregnant women qualify with family income up to 196% of FPL, and coverage for the mother continues for a year after the baby is born
- Parents and other adults qualify with family income up to 138% of FPL
Hawaii residents with low incomes and low asset/resource levels can qualify for Medicaid if they’re 65 or older, or if they’re blind or disabled. These enrollees are covered under fee-for-service (FFS) Medicaid, rather than the managed-care Med-QUEST program.
Hawaii also uses Medicaid funds to help cover premium costs for Hawaii residents who aren’t U.S. citizens but who are citizens of nations that have entered into the Compact of Free Association (COFA) with the U.S.
Apply for Medicaid in Hawaii
You can apply on-line at My Medical Benefits or by phone at 1-877-628-5076. Or, fill out an application.
Eligibility: Children with family income levels up to 308% of FPL. Pregnant women with family income up to 191% of FPL. Adults with family income up to 138% of FPL.



ACA’s Medicaid eligibility expansion in Hawaii
Hawaii adopted Medicaid expansion through the Affordable Care Act, extending eligibility for Medicaid to adults with income up to 138% of the poverty level (133% plus an automatic 5% income disregard). Medicaid expansion took effect in Hawaii in January 2014.
Starting in 2022, Hawaii extended postpartum Medicaid coverage so that it lasts for 12 months instead of 60 days, and the state also added adult dental benefits to Medicaid starting in 2023.
According to U.S. Census data, only 3.5% of Hawaii residents were uninsured as of 2016, down from 6.7% in 2013. Although the state’s uninsured rate was reduced by nearly half from 2013 to 2016, it was already less than half of the national average uninsured rate even in 2013, before the bulk of the ACA’s provisions had taken effect. Hawaii’s Prepaid Health Care Act, which has been in place since the 1970s, had already resulted in nearly all of the state’s population having insurance coverage, even before the ACA took effect.
466,437 people were enrolled in Medicaid/CHIP in Hawaii as of September 2023. Hawaii Medicaid/CHIP enrollment has grown by 62% since late 2013. That growth has been mainly due to Medicaid expansion and the COVID-related rule that prevented states from disenrolling anyone from Medicaid between March 2020 and March 2023.
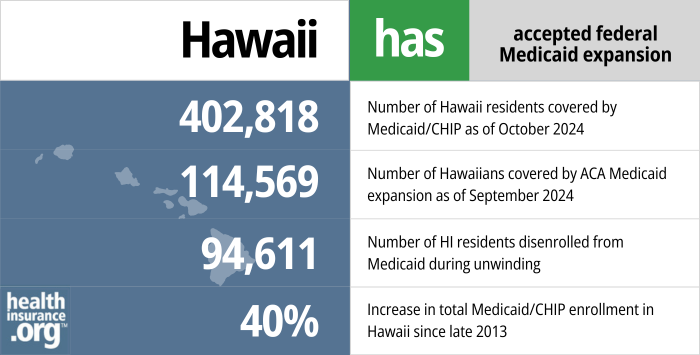
- 402,818 – Number of Hawaii residents covered by Medicaid/CHIP as of October 20242
- 114,569 – Number of Hawaiians covered by ACA Medicaid expansion as of September 20243
- 94,611– Number of HI residents disenrolled from Medicaid during unwinding4
- 40% – Increase in total Medicaid/CHIP enrollment in Hawaii since late 20133
Explore our other comprehensive guides to coverage in Hawaii

Hawaii utilizes a federally run health insurance Marketplace, which means residents enroll through HealthCare.gov, where two private insurers offer individual/family health plans for Hawaii residents. But Hawaii still oversees the plans sold in the exchange.


Hoping to improve your smile? Dental insurance may be a smart addition to your health coverage. Our guide explores dental coverage options in Hawaii.


Use our guide to learn about Medicare, Medicare Advantage, and Medigap coverage available in Hawaii as well as the state’s Medicare supplement (Medigap) regulations.


Short-term health plans provide temporary health insurance for consumers who may find themselves without comprehensive coverage.

Frequently asked questions about Hawaii Medicaid eligibility and enrollment
How do I enroll in Medicaid in Hawaii?
You can apply for Med-QUEST:
- Online at My Medical Benefits or at Healthcare.gov (only apply through Healthcare.gov if you don’t have Medicare)
- Over the phone at 1-877-628-5076
- By mail. Download an application or call the appropriate eligibility office to have an application mailed to you. Complete the application and return it by mail to the office.
How does Medicaid provide financial help to Medicare beneficiaries in Hawaii?
Many Medicare beneficiaries receive assistance from Medicaid with Medicare premiums, prescription drug costs, and expenses not covered by Medicare – including long-term care.
Our guide to financial assistance for Medicare enrollees in Hawaii includes overviews of these programs, including Medicaid long-term care benefits, Extra Help, and eligibility guidelines for assistance.
Legislation was introduced in Hawaii in 2023 to remove the $2,000 Medicaid asset limit for people who are also enrolled in Medicare, but it did not advance. Most states use this same $2,000 asset limit for Medicaid eligibility for people who are 65 or older.5
How did Hawaii handle Medicaid renewals after the pandemic?
Throughout the pandemic, states received additional federal Medicaid funding, but on the condition that nobody be disenrolled from Medicaid. But that rule ended March 31, 2023, and states began a year-long process of “unwinding” the pandemic rules, gradually redetermining eligibility for everyone enrolled in Medicaid.
Hawaii began disenrolling ineligible Med-QUEST members (and those who didn’t respond to renewal packets) at the end of May 2023.
But due to the devastating Maui wildfire, Hawaii opted to pause all Med-QUEST eligibility redeterminations through the end of 2023. And for Maui residents, redeterminations did not resume until May 2024.6
Med-QUEST enrollment had peaked at about 468,000 people just before the start of the unwinding process, and had dropped to about 406,000 by the end of 2024, after eligibility determinations had been completed for all enrollees.7
Hawaii Med-QUEST has a useful overview page about the return to normal eligibility operations. It includes a dashboard of unwinding data, press releases, and copies of the letters that enrollees received.
Hawaii’s unwinding plan noted that the state would wait until the end of the unwinding period to process renewals for unhoused enrollees.
For those who are no longer eligible for Medicaid, coverage could be obtained from an employer (if available) or via the Hawaii Marketplace at HealthCare.gov. During the unwinding period, CMS reported that 5,152 Hawaii residents transitioned from Med-QUEST to a Marketplace plan.8
Hawaii Medicaid history and details
Medicaid expansion helped cement top-ranking health scores
Hawaii has a long history of supporting initiatives to make health insurance broadly available to residents. Hawaii was among the first six states that implemented a Medicaid program in January 1966, just six months after federal legislation authorizing the program was enacted. In 1974, Hawaii implemented its Prepaid Health Care Act, which mandated that most employers make health insurance available to employees who work at least 20 hours a week.
In conjunction with the Affordable Care Act (ACA), Hawaii initially implemented a state-run health insurance marketplace and adopted Medicaid expansion. The marketplace transitioned to a federally-supported state-run marketplace for 2016, and transitioned again to a fully federally-run exchange for 2017, largely in an effort to take advantage of the economies of scale that the federally-run exchange could bring to a state with low overall enrollment in the individual market (because of Hawaii’s Prepaid Health Care Act, nearly all non-elderly Hawaii residents get coverage from an employer, and relatively few need coverage under individual market plans). Nothing changed about Medicaid with the switch to Healthcare.gov though; the expanded Medicaid eligibility guidelines are still in effect in Hawaii.
Through its efforts, Hawaii consistently has low uninsured rates and high overall health scores. In 2018, Hawaii was ranked the healthiest state in the nation for the 7th year in a row according to the Gallup Healthways Physical Wellbeing Index, and the state consistently scores at or near the top in other ranking systems (number 1 in the America’s Health Rankings 2020 survey, and number 1 in the Commonwealth Fund’s 2020 Scorecard on State Health System Performance).
Hawaii Medicaid history
Hawaii implemented its Medicaid program in January 1966.
In the early 1990s, Hawaii implemented the State Health Insurance Program (SHIP) to cover people who weren’t eligible for Medicaid. Then, in 1994, CMS approved Hawaii’s section 1115 Medicaid waiver (one of the first in the nation) to wrap SHIP in with Medicaid in an effort to achieve universal insurance coverage (in combination with the state’s Prepaid Health Care Act). The result of the waiver was the creation of Hawaii’s MED-QUEST program, which initially covered low-income women and children, but has since expanded (as of 2009) to cover nearly all of Hawaii’s Medicaid beneficiaries. The MED-QUEST waiver is subject to renewal every five years.
Medicaid in Hawaii is separated into two different methods of providing services: the fee-for-service (FFS) program and the managed care program, called Med-QUEST or MQD. Under the FFS program, doctors and other healthcare providers bill Medicaid directly to be reimbursed for services provided to Medicaid beneficiaries. Under Med-QUEST, the state contracts with managed care plans that provide healthcare services to Medicaid beneficiaries.
Virtually all of the people enrolled in Hawaii’s Medicaid program are covered through managed care (Med-QUEST). Hawaii only uses fee-for-service Medicaid (ie, without managed care) for a handful of limited Medicaid programs. Hawaii Medicaid managed care members include people who are covered under Hawaii’s fully-state-funded Medicaid program, in addition to the majority of enrollees who are in regular Medicaid that’s funded partially by the state and partially by the federal government.
In August 2017, Hawaii submitted a waiver amendment to CMS in order to gain federal approval to use Medicaid funding to provide housing services to qualified Medicaid enrollees who are homeless and also have behavioral health and/or substance abuse problems. That waiver request was approved in October 2020.
Louise Norris is an individual health insurance broker who has been writing about health insurance and health reform since 2006. She has written dozens of opinions and educational pieces about the Affordable Care Act for healthinsurance.org.

Looking for more information about other options in your state?
Need help navigating health insurance options in Hawaii?
Explore more resources for options in Hawaii including ACA coverage, short-term health insurance, dental insurance and Medicare.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- ”Biden-Harris Administration Announces Approvals in Five States that will Keep Eligible Children and Adults Enrolled in Medicaid and CHIP” Centers for Medicare & Medicaid. Nov. 14, 2024 ⤶
- ”October 2024 Medicaid & CHIP Enrollment Data Highlights” Medicaid.gov, Accessed January 2025 ⤶
- “Total Monthly Medicaid & CHIP Enrollment and Pre-ACA Enrollment”, KFF.org, Accessed Jan. 14, 2025 ⤶ ⤶
- “Medicaid Enrollment and Unwinding Tracker ” KFF.org, Accessed Jan. 14, 2025 ⤶
- ”Medicaid Eligibility for SSI Enrollees and Optional Seniors & People with Disabilities Up To 100% FPL” KFF.org. Accessed Jan. 14, 2025 ⤶
- ”Maui Fire Updates” Kaiser Permanente. Winter 2024. Accessed Jan. 14, 2025 ⤶
- ”Application and Enrollment Data Update” State of Hawai‘i Department of Human Services. Dec. 16, 2024 ⤶
- HealthCare.gov Marketplace Medicaid Unwinding Report. Centers for Medicare and Medicaid Services. Data through April 2024. Accessed Jan. 14, 2025 ⤶

