Home > Health Insurance Marketplace > South Dakota Heath Insurance Marketplace
Find South Dakota Health Insurance Marketplace Coverage for 2026

Compare ACA plans and check subsidy savings from a licensed third-party health insurance agency.

South Dakota Marketplace quick facts
South Dakota health insurance Marketplace guide
This guide, including the FAQs below, was developed to assist you in choosing the right South Dakota health insurance plan for you and your family. The options found in South Dakota’s ACA Marketplace (exchange) may be a good choice for many consumers, and we will guide you through the options below.
South Dakota uses the federally-facilitated HealthCare.gov exchange platform for residents to purchase its ACA Marketplace plans. The Marketplace provides access to health insurance products offered by three private insurers with varying coverage areas.4 (See below for details about premium changes for 2026; note that after-subsidy premiums have increased sharply because federal subsidy enhancements were allowed to expire at the end of 2025.)
Depending on your income and circumstances, you may qualify for federally-funded premium subsidies (premium tax credits) when you enroll in a health plan through the South Dakota Marketplace. Depending on your income and the plan you select, you may also find that you qualify for subsidies that will reduce your out-of-pocket expenses.
Frequently asked questions about health insurance in South Dakota
Who can buy Marketplace health insurance in South Dakota?
To qualify for health coverage through the South Dakota Marketplace, you must:5
- Live in South Dakota
- Be lawfully present in the United States
- Not be incarcerated
- Not be enrolled in Medicare
Eligibility for financial assistance (premium subsidies and cost-sharing reductions) depends on your household income. In addition, to qualify for financial assistance with your Marketplace plan you must:
- Not have access to an affordable employer-sponsored health insurance plan. If your employer offers coverage but you feel it’s too expensive, you can use our Employer Health Plan Affordability Calculator to see if you might qualify for premium subsidies in the Marketplace.
- Not be eligible for Medicaid or CHIP (note that Medicaid expansion took effect in South Dakota as of mid-2023, so people who are now eligible for Medicaid expansion are no longer eligible for premium subsidies).
- Not be eligible for premium-free Medicare Part A.6
- If married, file a joint tax return.7
- Not be able to be claimed by someone else as a tax dependent.7
When can I enroll in an ACA-compliant plan in South Dakota?
In South Dakota, the next open enrollment period for individual and family health coverage runs from November 1 to December 15, 2026. All policies selected during open enrollment will take effect January 1, 2027.
Outside of open enrollment, you’ll need a special enrollment period (SEP), triggered by a qualifying life event, to enroll or make changes to your coverage.
If you have questions about open enrollment, you can learn more in our comprehensive guide to open enrollment. We also have a comprehensive guide to special enrollment periods.
American Indians and Alaska Natives can enroll anytime, year-round.
How do I enroll in a South Dakota Marketplace plan?
To enroll in an ACA Marketplace plan in South Dakota, you can:
- Visit HealthCare.gov to access South Dakota’s health insurance Marketplace. Here you will find an online platform to shop, compare, and choose the best health plans.
- Purchase individual and family health coverage with the help of an insurance agent or broker, a Navigator or certified application counselor, or an approved enhanced direct enrollment entity.8
You can also call HealthCare.gov’s contact center by dialing 1-800-318-2596 (TTY: 1-855-889-4325). The call center is available 24 hours a day, seven days a week, but it’s closed on holidays.
How can I find affordable health insurance in South Dakota?
South Dakota uses the federally-facilitated exchange for individual market plans, so residents who buy their own health insurance enroll through HealthCare.gov.
During the open enrollment period for 2026 coverage, about 83% who enrolled through the South Dakota Marketplace qualified for premium subsidies. The subsidies averaged about $568/month, bringing the average subsidy-eligible enrollee’s monthly cost down to about $118/month.1
But coverage is less affordable in 2026, due to the expiration of federal subsidy enhancements at the end of 2025. Most enrollees still qualify for subsidies, but they don’t cover as much of enrollees’ premiums as they did in 2025.
People with household incomes up to 250% of the federal poverty level also qualify for cost-sharing reductions (CSR) that result in lower deductibles and out-of-pocket expenses for Silver plans.9
Between the premium subsidies and cost-sharing reductions, you may find that a South Dakota Marketplace plan provides the best value when you’re shopping for health coverage.

Source: CMS.gov1
The ACA’s Medicaid expansion took effect in South Dakota in mid-2023, due to a ballot measure that voters approved in the 2022 election. An estimated 52,000 low-income South Dakota residents were initially expected to enroll in Medicaid under the expanded eligibility guidelines, but enrollment has trended lower than expected. Only 31,202 people were enrolled in South Dakota’s Medicaid expansion as of March 2025.10
People with income between 100% and 138% of the poverty level were eligible for premium subsidies in the South Dakota Marketplace in 2023 and previous years. But they’re no longer eligible for subsidies, as they’re eligible for Medicaid expansion instead.
How many insurers offer Marketplace coverage in South Dakota?
Are Marketplace health insurance premiums increasing in South Dakota?
The following average rate changes were approved for 2026 for the insurers that offer health insurance through South Dakota’s Marketplace, amounting to a weighted average rate increase of 6.4%, before subsidies are applied.11
South Dakota’s ACA Marketplace Plan 2026 APPROVED Rate Increases by Insurance Company |
|
|---|---|
| Issuer | Percent Increase |
| Avera | 8.9% |
| Sanford Health Plan | 5.8% |
| Wellmark Blue Cross Blue Shield of SD | 1.2% |
Source: RateReview.HealthCare.gov11
Although average full-price premiums increased only modestly in South Dakota for 2026, after-subsidy premiums increased sharply due to the expiration of federal subsidy enhancements at the end of 2025.
The South Dakota Division of Insurance doesn’t publicize information about the rate review process until regulators have finalized the rates. However, regulators in South Dakota do have the authority to reject rate filings that aren’t justified, or to require insurers to make adjustments to proposed rates.12 (Under federal rules, this is not required, and insurers can implement rates even if they’re determined to be unreasonable.13 But states can go beyond the federal minimum rate review requirements.) However, rates in South Dakota have historically tended to be approved as filed, as was the case for 2026.
For perspective, here’s an overview of how full-price (unsubsidized) average premiums have changed over time in South Dakota’s individual/family market:
- 2015: Average decrease of 21%.14
- 2016: Average increase of 27.4%.15
- 2017: Average increase of 37.9%.16
- 2018: Average increase of 27.4%.17
- 2019: Average increase of 5.2%.18
- 2020: Average increase of 6.5%.19
- 2021: Average increase of 2.6%20
- 2022: Average decrease of 1.2%.21
- 2023: Average increase of 11.4%.22
- 2024: Average increase of 2.5%.23
- 2025: Average increase of 2.3%24
How many people are insured through South Dakota’s Marketplace?
During the open enrollment period for 2026 coverage, 50,951 people selected coverage through the South Dakota exchange.1
A record high of 54,721 people had enrolled the year before, for coverage effective in 2025.25 That was the fifth consecutive year of new record high enrollment for South Dakota’s exchange (see graph below).
The surge in enrollment during these years was due in part to the American Rescue Plan (ARP) which made ACA’s premium subsidies more substantial. Under the ARP – and extended through 2025 by the Inflation Reduction Act – premium subsidies were larger and more widely available than they were prior to 2021.26 But as noted above, that is no longer the case in 2026, and the reduced affordability resulted in a decline in enrollment for the first time in several years.
The enrollment spike in 2024 was also due to the “unwinding” of the pandemic-era Medicaid continuous coverage rule. By April 2024, nearly 8,000 South Dakota residents had transitioned from Medicaid to a Marketplace plan during the unwinding process.27
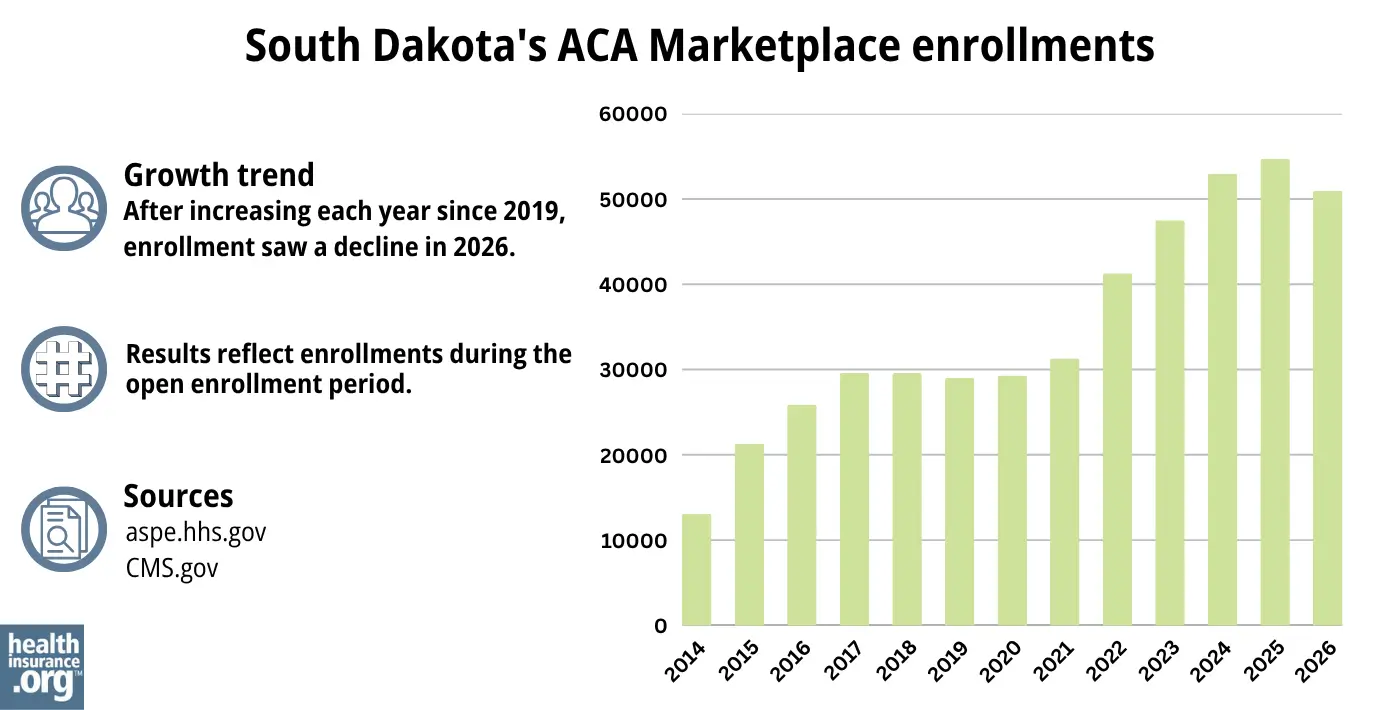
Source: 2014,28 2015,29 2016,30 2017,31 2018,32 2019,33 2020,34 2021,35 2022,36 2023,37 2024,38 202525 20261
What health insurance resources are available to South Dakota residents?
HealthCare.gov
800-318-2596
South Dakota Division of Insurance
Regulates health plans sold in the SD Marketplace, approves premiums, and licenses and oversees health insurers as well as agents and brokers.
State Exchange Profile: South Dakota
The Henry J. Kaiser Family Foundation overview of South Dakota’s progress toward creating a state health insurance exchange.

Looking for more information about other options in your state?
Need help navigating health insurance options in South Dakota?
Explore more resources for options in SD including short-term health insurance, dental, Medicaid and Medicare.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- ”2026 Marketplace Open Enrollment Period Public Use Files” CMS.gov. April 2026 ⤶ ⤶ ⤶ ⤶ ⤶
- ”South Dakota Rate Review Submissions” RateReview.HealthCare.gov. Accessed Sep. 14, 2025 *The above is based on the most current data available. ⤶
- ”2026 Marketplace Open Enrollment Period Public Use Files” and “Marketplace 2025 Open Enrollment Period Report: National Snapshot” Centers for Medicare & Medicaid Services, April 2026 ⤶
- ”Companies with Plans Certified to Sell in the General Market – 2026” South Dakota Division of Insurance. Accessed Feb. 3, 2026 ⤶ ⤶ ⤶
- ”A quick guide to the Health Insurance Marketplace” HealthCare.gov ⤶
- Medicare and the Marketplace, Master FAQ. Centers for Medicare and Medicaid Services. Accessed Feb. 3, 2026 ⤶
- Premium Tax Credit — The Basics. Internal Revenue Service. Accessed Feb. 3, 2026 ⤶ ⤶
- “Entities Approved to Use Enhanced Direct Enrollment” CMS.gov, Dec. 8, 2025 ⤶
- APTC and CSR Basics. Centers for Medicare and Medicaid Services. Oct. 2025 ⤶
- ”Medicaid Enrollment Data Collected Through MBES” and
“Medicaid Enrollment – New Adult Group” Centers for Medicare & Medicaid Services. Data for March 2025. Accessed Feb. 3, 2026 ⤶ - ”2026 FINAL Rate Changes – South Dakota: +6.4% (updated)” ACA Signups. Aug. 29, 2025 ⤶ ⤶
- Division of Insurance – Health Rate & Form Filing Requirements. 58-17-4.1 and 4.2. South Dakota Department of Labor and Regulation. Accessed November 2023. ⤶
- Rate Review Instructions Manual State Rate Review Determination Instructions and Reporting Requirements. Centers for Medicare and Medicaid Services. Accessed November 2023. ⤶
- Medicare and the Marketplace, Master FAQ. Centers for Medicare and Medicaid Services. Accessed November 2023. ⤶
- FINAL PROJECTION: 2016 Weighted Avg. Rate Increases: 12-13% Nationally* ACA Signups. October 2015. ⤶
- 2017 Rate Project State Roundup: IN, IA, ME, MA, MT, ND, SD, TN. ACA Signups. September 2016. ⤶
- 2018 Rate Hikes. ACA Signups. October 2017. ⤶
- South Dakota: *APPROVED* 2019 #ACA Rate Increases: 5.2% (Vs. Likely 4.8% *Drop* W/Out #ACASabotage). ACA Signups. September 2018. ⤶
- South Dakota: *Final* Avg. Unsubsidized 2020 #ACA Premium Changes: 6.5% Increase. ACA Signups. October 2019. ⤶
- South Dakota: Preliminary Avg. 2021 #ACA Premium Changes: +2.6% Individual Market; +2.8% Sm. Group. ACA Signups. October 2020 (for weighted average). And Companies with Plans Certified to Sell in the General Market, 2021 (SERFF Filings). South Dakota Division of Insurance. Accessed November 2023 (for confirmation that rates were approved as filed). ⤶
- South Dakota: Approved Avg. 2022 #ACA Rate Changes: -1.4% Indy; +4.0% Sm. Group (Updated). ACA Signups. October 2021. ⤶
- South Dakota: Final Avg. Unsubsidized 2023 #ACA Rate Changes: +11.4% (Updated). ACA Signups. August 2022. ⤶
- South Dakota: *Final* Avg. Unsubsidized 2024 #ACA Rate Changes: +2.5%. ACA Signups. November 2023. ⤶
- ”South Dakota: Preliminary avg. unsubsidized 2025 #ACA rate changes: +2.3%; Medica leaving sm. group market?” ACA Signups. Sep. 16, 2025 ⤶
- “2025 Marketplace Open Enrollment Period Public Use Files” CMS.gov, May 2025 ⤶ ⤶
- “Health Insurance Marketplaces 2023 Open Enrollment Report” CMS.gov, 2023 ⤶
- ”HealthCare.gov Marketplace Medicaid Unwinding Report” Centers for Medicare & Medicaid Services. Data through April 2024; Accessed Aug. 1, 2024. ⤶
- “ASPE Issue Brief (2014)” ASPE, 2015 ⤶
- “Health Insurance Marketplaces 2015 Open Enrollment Period: March Enrollment Report”, HHS.gov, 2015 ⤶
- “HEALTH INSURANCE MARKETPLACES 2016 OPEN ENROLLMENT PERIOD: FINAL ENROLLMENT REPORT” HHS.gov, 2016 ⤶
- “2017 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2017 ⤶
- “2018 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2018 ⤶
- “2019 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2019 ⤶
- “2020 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2020 ⤶
- “2021 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2021 ⤶
- “2022 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2022 ⤶
- “Health Insurance Marketplaces 2023 Open Enrollment Report” CMS.gov, Accessed August 2023 ⤶
- ”HEALTH INSURANCE MARKETPLACES 2024 OPEN ENROLLMENT REPORT” CMS.gov, 2024 ⤶

