Home > States > Health insurance in Montana
See your Montana health insurance coverage options.

Find individual and family plans, small-group, short-term or Medicare plans through licensed agency partners.

Montana Health Insurance Consumer Guide
We’ve created this guide and the FAQs below to help you understand the health insurance options available to you and your family in Montana. An ACA Marketplace (exchange) plan – or Obamacare – is a good option for people who need to buy their own individual or family health coverage. This includes people who aren’t eligible for Medicaid, Medicare, or an affordable plan offered by an employer.
Montana uses the federally run Marketplace, which is HealthCare.gov. Three private insurance companies offer coverage in the Montana Health Insurance Marketplace,1 and unlike many states where coverage areas vary from one carrier to another, all three insurers offer Marketplace coverage statewide in Montana.2
Income-based subsidies are available through the Montana Marketplace: Most enrollees qualify for premium subsidies, and many also qualify for subsidies that reduce out-of-pocket medical costs.3
If the Marketplace determines that you or your kids are likely eligible for Medicaid or CHIP (Healthy Montana Kids), they will refer you to Montana Medicaid/CHIP.
Explore our other comprehensive guides to coverage in Montana
Dental coverage in Montana

Looking to improve your smile and save some money when you go to the dentist? You may want to consider a dental insurance policy, in addition to your health insurance. Our guide explores dental coverage options in Montana.

Montana’s Medicaid program

Medicaid expansion under the ACA took effect in Montana in 2016.4 Enrollment in Montana Medicaid has grown by 121% since 2013, largely as a result of Medicaid expansion and the three-year pandemic-related pause on Medicaid disenrollments.5 Medicaid disenrollments resumed in Montana in April 2023, and by May, more than 34,000 people had been disenrolled.6

Medicare coverage and enrollment in Montana

As of 2023, more than 253,000 Montana residents were covered under Medicare.7 Our guide explains what you need to know about Medicare coverage options and Medigap regulations in Montana.

Short-term coverage in Montana

At least three insurers offer short-term health insurance in Montana. The state allows these plans to follow federal duration rules, but all of the insurers that offer short-term health plans in Montana have chosen to cap their plans at six months in duration.8

Frequently asked questions about health insurance in Montana
Who can buy Marketplace health insurance?
To enroll in private health coverage through Montana’s Marketplace (HealthCare.gov), you must:9
- Live in Montana and be lawfully present in the United States
- Not be incarcerated
- Not have Medicare coverage
So most people are eligible to enroll in Marketplace coverage. But qualifying for financial assistance (premium subsidies and cost-sharing reductions) is a bit more complex. Eligibility for financial assistance depends on your income, and you must also:
- Not have access to affordable health coverage offered by an employer. If you’re eligible to enroll in an employer-sponsored plan but it seems too expensive, you can use our Employer Health Plan Affordability Calculator to see if you might qualify for premium subsidies in the Marketplace.
- Not be eligible for Medicaid or CHIP (Montana Healthy Kids).
- Not be eligible for premium-free Medicare Part A.10
When can I enroll in an ACA-compliant plan in Montana?
You can sign up for an ACA-compliant individual or family health plan in Montana during the annual open enrollment period, which runs from November 1 through January 15. (For 2024 coverage, the deadline has been extended to January 16, 2024, due to the federal holiday on the 15th.)11
For coverage to take effect on January 1, you must complete your enrollment by December 15. If your application is submitted between December 16 and January 15, your coverage will take effect on February 1.9
Once the open enrollment window ends, you may still be eligible to enroll or make a plan change if you experience a qualifying life event, such as giving birth or losing other health coverage. Some people can enroll year-round even without a specific qualifying event.12
Enrollment in Montana Medicaid and Healthy Montana Kids (CHIP) is available year-round.13 If you’re eligible for either program, you can enroll anytime.
How do I enroll in a Marketplace plan in Montana?
To enroll in an ACA Marketplace (exchange) plan in Montana, you can:
- Visit HealthCare.gov, which is Montana’s Marketplace (exchange). This platform lets Montana residents comparison shop for health coverage, determine subsidy eligibility, and select the plan that best meets their needs.
- Enroll in Marketplace coverage with the help of an insurance agent or broker, or a Navigator or certified application counselor.
- Enroll via an approved enhanced direct enrollment entity (EDE).14 (EDEs can also offer off-exchange plans and non-ACA-compliant plans, so be sure to specify that you want to enroll in Marketplace/exchange coverage, as that’s the only way to obtain any subsidies for which you might be eligible.)
You can also call HealthCare.gov’s contact center by dialing 1-800-318-2596 (TTY: 1-855-889-4325). The call center is available 24 hours a day, seven days a week, except for holidays.
How can I find affordable health insurance in Montana?
You may find affordable health insurance coverage in Montana by enrolling through HealthCare.gov. This is especially true if you qualify for subsidies, and most enrollees in Montana are subsidy-eligible.
The Affordable Care Act created income-based premium subsidies called Advance Premium Tax Credits (APTC).15 If you’re eligible for APTC, it will reduce the amount you owe in premiums each month – sometimes even to $0, depending on your income and the plan you select.
Eighty-six percent of the Montana residents who selected a Marketplace plan during the 2023 open enrollment were eligible for premium subsidies. These subsidies paid an average of $491/month, reducing the average enrollee’s premium to about $133/month.16
In addition to premium subsidies, you may also qualify for cost-sharing reductions (CSR) if your household income isn’t more than 250% of the federal poverty level. CSR subsidies will make the deductible and other out-of-pocket expenses (for a Silver-level plan) smaller than they would otherwise be. Twenty-six percent of Montana’s Marketplace enrollees were receiving CSR benefits in 2023.17
You can combine APTC and CSR benefits if you’re eligible for both, as long as you select a Silver-level plan (APTC can be used with plans at any metal level, but CSR benefits are only available on Silver plans).
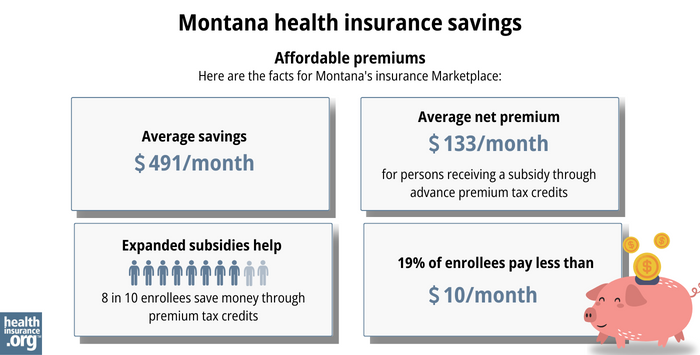
Source: CMS.gov16
Montana implemented a reinsurance program in 2020, which resulted in overall average rate decreases that year and relatively flat rates the following year.18 So if you’re not eligible for premium subsidies in Montana, the reinsurance program does ensure that your premiums are lower than they would otherwise be.
Depending on your income and circumstances, you may find that you’re eligible for free or low-cost health coverage through Montana Medicaid or Healthy Montana Kids (CHIP). Check to see if you meet the criteria for these programs in Montana.
How many insurers offer Marketplace coverage in Montana?
Three private insurance companies offer Marketplace health insurance coverage in Montana,1 and all three have statewide coverage areas.2
One of Montana’s insurers, Montana/Mountain Health CO-OP, is among just three ACA-created CO-OPs still in operation nationwide.
Are Marketplace health insurance premiums increasing in Montana?
Montana’s individual/family health insurers implemented the following average rate changes for 2024,19 which amount to a weighted average rate increase of 4.9%, before any subsidies are applied.20
Montana’s ACA Marketplace Plan 2024 Approved Rate Increases by Insurance Company |
|
|---|---|
| Issuer | Percent Increase |
| BCBS of Montana (Health Care Service Corporation, or HCSC) | 4.9% |
| Montana Health CO-OP | 6.4% |
| PacificSource | 1.5% |
Source: Federal rate review database1
Average rate increases are for full-price plans. But 87% of Marketplace enrollees in Montana receive premium tax credits that cover some or all of their monthly premium costs.17
These subsidies are adjusted each year to match changes in the benchmark plan (the second-lowest-cost Silver plan) in each area. As a result of the American Rescue Plan and the Inflation Reduction Act, subsidies are larger and more widely available than they were in the past, and that will continue to be true at least through 2025.21
For perspective, here’s an overview of how average full-price premiums have changed in Montana’s individual/family health insurance market over the years:
- 2015: Average increase of 3%.22
- 2016: Average increase of 25.9%.23
- 2017: Average increase of 47.6%.24
- 2018: Average increase of 19.5%.25
- 2019: Average increase of 5.7%.26
- 2020: Average decrease of 13.1%.27 (reinsurance program took effect)
- 2021: Average increase of 1.4%.28
- 2022: Average increase of 0.5%.29
- 2023: Average increase of 9.6%.30
How many people are insured through the Marketplace in Montana?
Nearly 54,000 people enrolled in private plans through the Marketplace in Montana during the open enrollment period for 2023 coverage.21
Effectuated enrollment is always a little lower than the number of people who initially select plans. As of early 2023, nearly 52,000 people were enrolled in coverage through Montana’s Marketplace.31
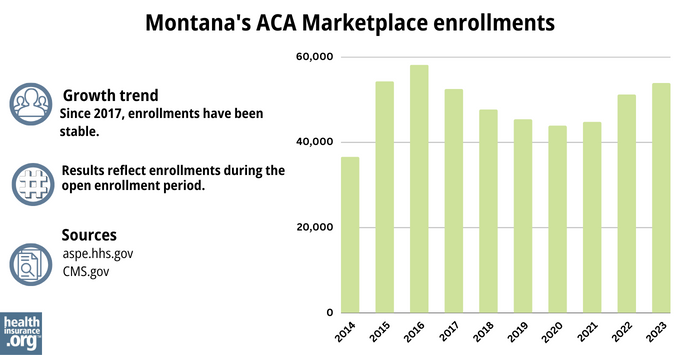
Source: 2014,32 2015,33 2016,34 2017,35 2018,36 2019,37 2020,38 2021,39 2022,40 202321
What health insurance resources are available to Montana residents?
HealthCare.gov: The Marketplace in Montana, where residents can enroll in individual/family health coverage and receive income-based subsidies. You can reach HealthCare.gov at 800-318-2596.
Montana Commissioner of Securities and Insurance: Licenses and regulates health insurance companies, agents, and brokers; can provide assistance to consumers who have questions or complaints about entities the Commissioner regulates.
Montana Primary Care Association: Montana’s federally funded Navigator organization
Montana State Health Insurance Assistance Program: A local service that provides assistance and enrollment counseling for Medicare beneficiaries and their caregivers.
Montana Medicaid and Healthy Montana Kids (Montana’s Children’s Health Insurance Program)
Louise Norris is an individual health insurance broker who has been writing about health insurance and health reform since 2006. She has written dozens of opinions and educational pieces about the Affordable Care Act for healthinsurance.org.
Footnotes
- “Montana Rate Review Submissions” HealthCare.gov, 2023 ⤶ ⤶ ⤶
- Plan Year 2024 Qualified Health Plan Choice and Premiums in HealthCare.gov Marketplaces. Centers for Medicare and Medicaid Services. October 25, 2023. ⤶ ⤶
- 2023 Marketplace Open Enrollment Period Public Use Files. CMS.gov, Accessed September 2023. ⤶
- “Medicaid Expansion Information for Stakeholders” Montana.gov, Accessed September 2023 ⤶
- “Total Monthly Medicaid & CHIP Enrollment and Pre-ACA Enrollment” KFF.org, April 2023 ⤶
- “Montana Medicaid Redetermination” Montana.gov, Aug. 22, 2023 ⤶
- “Medicare Monthly Enrollment” CMS.gov, April 2023. ⤶
- “Availability of short-term health insurance in Montana” healthinsurance.org, March 8, 2023 ⤶
- “A quick guide to the Health Insurance Marketplace®” HealthCare.gov, Accessed August, 2023 ⤶ ⤶
- Medicare and the Marketplace, Master FAQ. Centers for Medicare and Medicaid Services. Accessed November 2023. ⤶
- Biden-Harris Administration Launches Window-Shopping Ahead of 11th ACA Marketplace Open Enrollment Period. Centers for Medicare and Medicaid Services. October 2023. ⤶
- “Who doesn’t need a special enrollment period?“ healthinsurance.org, Accessed August 2023 ⤶
- “Montana Medicaid and Healthy Montana Kids (HMK) Plus” Montana.gov, Accessed September 2023 ⤶
- “Entities Approved to Use Enhanced Direct Enrollment” CMS.gov, April 28, 2023 ⤶
- “APTC and CSR Basics” CMS.gov, June 2023 ⤶
- “2023 Marketplace Open Enrollment Period Public Use Files” CMS.gov, Accessed September 2023. ⤶ ⤶
- “Effectuated Enrollment: Early 2023 Snapshot and Full Year 2022 Average” CMS.gov, March 15, 2023 ⤶ ⤶
- Montana Individual Health Reinsurance. Montana Reinsurance Association. Accessed December 2023. ⤶
- “Montana Rate Review Submissions” HealthCare.gov, 2023 ⤶
- So How’d I Do On My 2024 Avg. Rate Change Project? Not Bad At All! ACA Signups. December 2023. ⤶
- “Health Insurance Marketplaces 2023 Open Enrollment Report” CMS.gov, 2023 ⤶ ⤶ ⤶
- Analysis Finds No Nationwide Increase in Health Insurance Marketplace Premiums. The Commonwealth Fund. December 2014. ⤶
- FINAL PROJECTION: 2016 Weighted Avg. Rate Increases: 12-13% Nationally* ACA Signups. October 2015. ⤶
- Avg. UNSUBSIDIZED Indy Mkt Rate Hikes: 25% (49 States + DC). ACA Signups. October 2016. ⤶
- 2018 Rate Hikes. ACA Signups. October 2017. ⤶
- 2019 Rate Hikes. ACA Signups. October 2018. ⤶
- 2020 Rate Changes. ACA Signups. October 2019. ⤶
- 2021 Rate Changes. ACA Signups. October 2020. ⤶
- 2022 Rate Changes. ACA Signups. October 2021. ⤶
- “Montana: Final Avg. Unsubsidized 2023 #ACA Rate Change: +9.6% (Up From +8.9%)” ACASignups.net, Oct. 12, 2022 ⤶
- “Effectuated Enrollment: Early 2023 Snapshot and Full Year 2022 Average” CMS.gov, March 15, 2023. ⤶
- “ASPE Issue Brief (2014)” ASPE, 2015 ⤶
- “Health Insurance Marketplaces 2015 Open Enrollment Period: March Enrollment Report”, HHS.gov, 2015 ⤶
- “HEALTH INSURANCE MARKETPLACES 2016 OPEN ENROLLMENT PERIOD: FINAL ENROLLMENT REPORT” HHS.gov, 2016 ⤶
- “2017 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2017 ⤶
- “2018 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2018 ⤶
- “2019 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2019 ⤶
- “2020 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2020 ⤶
- “2021 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2021 ⤶
- “2022 Marketplace Open Enrollment Period Public Use Files” CMS.gov, 2022 ⤶







