In this article
- When is the Affordable Care Act’s annual open enrollment period?
- How is the open enrollment schedule changing?
- What was the deadline to enroll in 2026 ACA-compliant health insurance coverage in the individual market?
- States that continued 2026 enrollment past the OEP deadline
- Outside of ACA’s open enrollment window, enrollment is only available with a special enrollment period
- Open enrollment schedule has varied over time
When is the Affordable Care Act’s annual open enrollment period?
The annual ACA open enrollment window for 2026 coverage ended in early 2026. The open enrollment period followed the same schedule that had been used for the last few years, with most states running open enrollment from November 1 through January 15.
Here’s everything we know right now about ACA open enrollment deadlines going forward:
How is the open enrollment schedule changing?
Starting in the fall of 2026, open enrollment will be shorter and will end on December 15 in many states. And all plans selected during open enrollment will take effect on January 1, as there will no longer be an option for a February 1 start date without a special enrollment period.
State-run exchanges have the option to extend their enrollment period later than December 15, but not later than December 31, and will have to ensure that all plans selected during open enrollment take effect on January 1.1
In all states except Idaho and Georgia, open enrollment for 2027 coverage will begin on November 1, 2026. (In Idaho, it will begin on October 15,2 and in Georgia it will begin on October 19).3
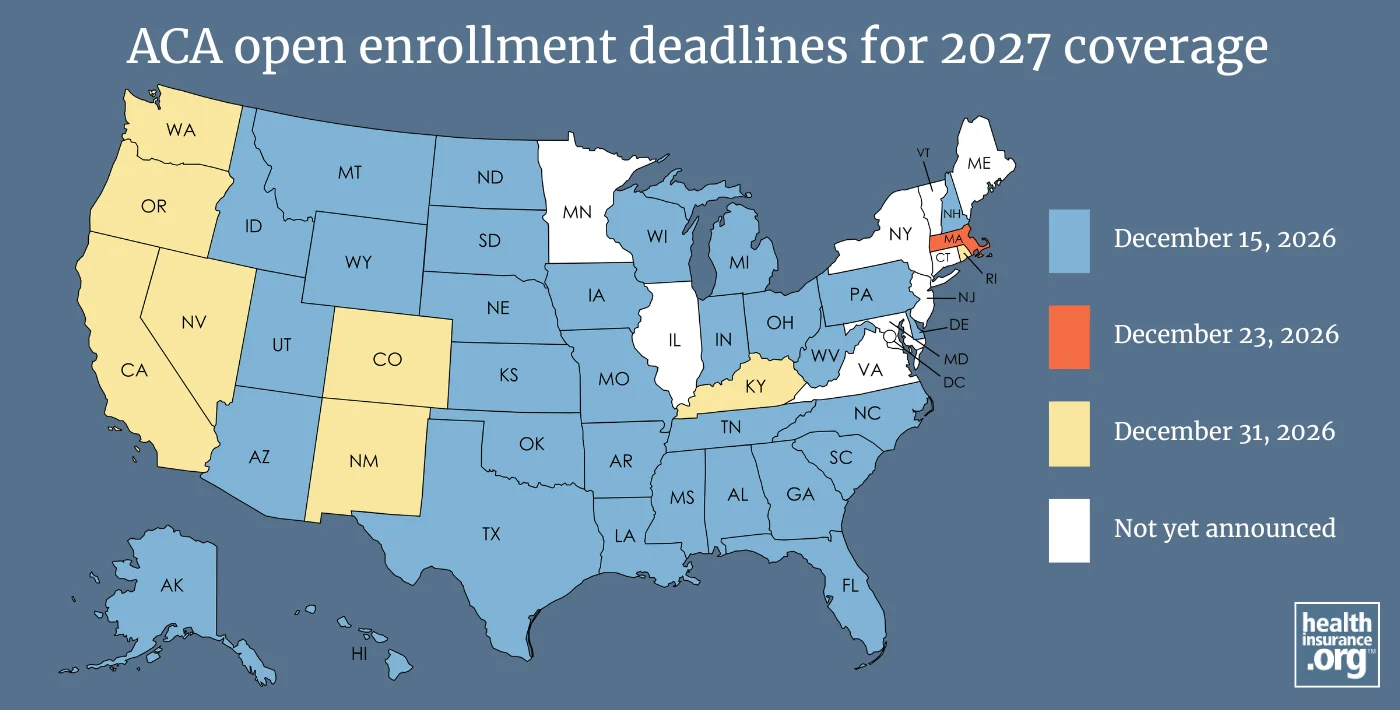
And although December 15, 2026 will be the enrollment deadline for 2027 coverage in most states (including the 29 states that will use HealthCare.gov for 2027 coverage), the following state-run exchanges have announced later enrollment deadlines:
- Massachusetts: December 234
- California: December 315
- Colorado: December 316
- Kentucky: December 317
- Nevada: December 318
- New Mexico: December 319
- Oregon: December 3110
- Rhode Island: December 3111
- Washington: December 3112
Pennsylvania’s exchange has proposed using a December 15 enrollment deadline,13 and Georgia's exchange has confirmed a December 15 enrollment deadline.3
We’ll continue to update this page as we get closer to open enrollment and more state-run exchanges announce the deadlines that they’ll be using for 2027 coverage.
What was the deadline to enroll in 2026 ACA-compliant health insurance coverage in the individual market?
In most states, open enrollment for individual/family health coverage for 2026 ended on January 15, 2026, although it ended in December 2025 in Idaho, and there are several states where it continued until January 31, 2026. Washington, D.C. had the latest enrollment deadline of February 4, which was a last-minute extension.14
States that continued 2026 enrollment past the OEP deadline
Although open enrollment for 2026 coverage has ended in Connecticut, people who are eligible for Connecticut’s new state-funded subsidies have a special enrollment period that began February 1, 2026.15 This special enrollment window was still ongoing as of mid-April 2026.16
And in Illinois, people whose 2025 coverage automatically renewed – and who had not claimed their Get Covered Illinois account by February 1, 2026 – had a special enrollment period that continued through March 31, during which they could select a different plan to cover them for the rest of 2026.17
(Illinois transitioned from HealthCare.gov to the Get Covered Illinois platform for the 2026 plan year. Illinois residents with HealthCare.gov were assigned Get Covered Illinois accounts as part of the transition, but some enrollees didn’t visit the new site and let their coverage auto-renew instead. These people were eligible for the special enrollment period.)
Outside of ACA’s open enrollment window, enrollment is only available with a special enrollment period
After open enrollment ends, people can normally only purchase coverage if they have a special enrollment period (SEP) triggered by a qualifying life event. You can learn more about special enrollment periods in our Special Enrollment Guide.
Read: Who doesn’t need a qualifying life event to enroll in health insurance outside of open enrollment?
Open enrollment schedule has varied over time
In the federally run Marketplaces, the following enrollment windows have been used (with some last-minute extensions, and with somewhat different schedules used by the state-run Marketplaces):
- 2014 coverage: October 1, 2013 through March 31, 2014
- 2015 coverage: November 15, 2014 through February 15, 2015
- 2016 coverage: November 1, 2015 through January 31, 2016
- 2017 coverage: November 1, 2016 through January 31, 2017
- 2018 coverage: November 1, 2017 through December 15, 2017
- 2019 coverage: November 1, 2018 through December 15, 2018
- 2020 coverage: November 1, 2019 through December 15, 2019
- 2021 coverage: November 1, 2020 through December 15, 2020
- 2022 coverage: November 1, 2021 through January 15, 2022
- 2023 coverage: November 1, 2022 through January 15, 2023
- 2024 coverage: November 1, 2023 through January 16, 2024 (one-day extension due to a federal holiday)
- 2025 coverage: November 1, 2024 through January 15, 2025
- 2026 coverage: November 1, 2025 through January 15, 2026
- 2027 coverage: November 1, 2026 through December 15, 202618
Footnotes
- “Patient Protection and Affordable Care Act; Marketplace Integrity and Affordability” Federal Register, U.S. Department of Health & Human Services. June 25, 2025 ⤶
- “How to Enroll” Your Health Idaho. Accessed Apr. 15, 2026 ⤶
- "Georgia Access Plan Year (PY) 2027 Qualified Health Plan (QHP) Application Instructions for Issuers" Georgia Access. Mar. 30, 2026 ⤶ ⤶
- "When is Open Enrollment and when do Health Connector plans start?" Massachusetts Health Connector. Accessed Apr. 22, 2026 ⤶
- “Federal Changes to Your Health Insurance” Covered California. Accessed Apr. 15, 2026 ⤶
- Confirmed via email by Connect for Health Colorado, Apr. 28, 2026 ⤶
- "Open Enrollment has ended!" Kentucky Health Benefit Exchange. Accessed Apr. 28, 2026 ⤶
- “When can I enroll?” Nevada Health Link. Accessed Apr. 15, 2026 ⤶
- “Federal and State Policy Changes” BeWellnm. Accessed Apr. 15, 2026 ⤶
- "April board meeting" (starting at the 51-minute mark). Oregon Health Insurance Marketplace. Apr. 16, 2026 ⤶
- “Open Enrollment operated differently this year. Stay connected to us… and stay covered.” Health Source RI. Accessed Apr. 15, 2026 ⤶
- “Enrollment Periods” Washington Healthplanfinder. Accessed Apr. 15, 2026 ⤶
- “Pennie Board of Directors Meeting” Pennie.com. Feb. 2026 ⤶
- “DC Health Link Enrollment Deadline Extended” HillRag. Feb. 2, 2026 ⤶
- “Access Health CT to Offer Special Enrollment Period for Eligible Customers to Enroll in Coverage with New State Subsidy” Access Health CT. Jan. 23, 2026 ⤶
- “Special Enrollment Period, Other Opportunities to Enroll” Access Health CT. Accessed Apr. 15, 2026 ⤶
- “Limited-time marketplace transition year Special Enrollment Period” Get Covered Illinois. Accessed Feb. 6, 2026 ⤶
- “Patient Protection and Affordable Care Act; Marketplace Integrity and Affordability” Federal Register, U.S. Department of Health & Human Services. June 25, 2025 ⤶



