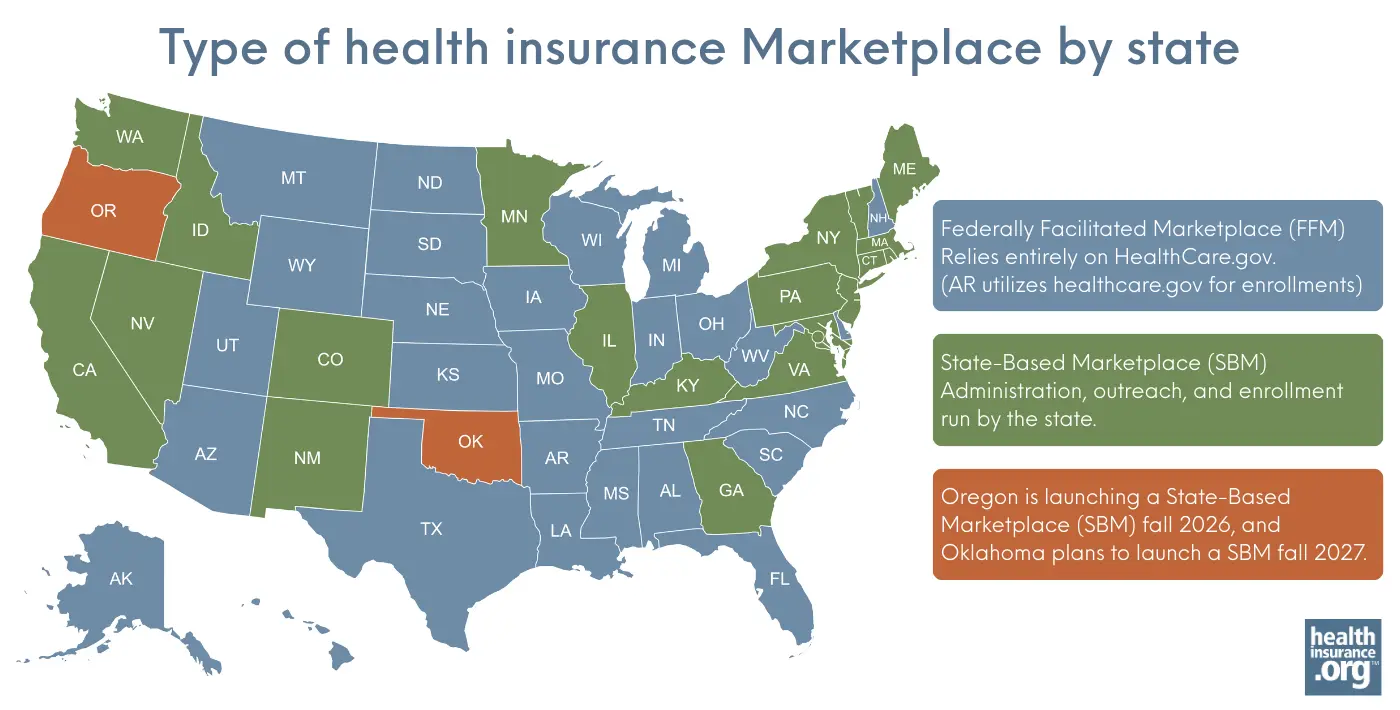
What type of health insurance exchange/marketplace does my state have?
For the 2026 plan year, there are:
- 21 fully state-run health insurance marketplaces (SBMs),
- 2 state-based marketplaces that use the federal platform (SBM-FP), and
- 28 federally-run marketplaces (FFMs).
Note that the federal platform is HealthCare.gov. And "Exchange" and "Marketplace" mean the same thing, so you'll also see people use the acronyms SBE, SBE-FP, and FFE.
There will be some changes for 2027 and 2028, discussed below. But here's how each state's health insurance exchange operates, as of the 2026 plan year:
SBMs: State-run marketplaces
For 2026, 21 states have their own enrollment websites, fund their own Navigator programs, create state-specific special enrollment periods (within various federal parameters), etc. Everything about the exchange is state-run, although they do have to comply with various federal rules. These states have the flexibility to create state-specific special enrollment periods, modify the open enrollment schedule, or offer additional state-funded subsidies through the exchange.
- California
- Colorado
- Connecticut
- District of Columbia
- Georgia
- Idaho
- Illinois (state-run platform starting with the 2026 plan year)1
- Kentucky
- Maine
- Maryland
- Massachusetts
- Minnesota
- Nevada
- New Jersey
- New Mexico
- New York
- Pennsylvania
- Rhode Island
- Vermont
- Virginia
- Washington
SBM-FPs: State-based marketplaces that use the federal enrollment platform (HealthCare.gov)
Two states administer their own exchanges and fund their own Navigator programs, but use the HealthCare.gov enrollment platform and call center (down from three in 2025, as Illinois transitioned from an SBM-FP to an SBM). So there are some limitations in terms of what they can do. For example, they cannot set state-specific special enrollment periods or offer additional state-funded subsidies via the exchange, since they are utilizing the same HealthCare.gov framework that's used in other states.
- Arkansas
- Oregon (Oregon plans to operate a state-run exchange platform starting in the fall of 2026,2 due to legislation enacted in 2023)3
FFMs: Federally-run marketplace (HealthCare.gov)
Twenty-eight states rely entirely on the federally run HealthCare.gov Marketplace (these are the same 28 states that had FFMs in 2025). They receive federal Navigator funding,4 and the federal government administers all aspects of the exchange. In most states, the state conducts the rate review process before plans can be approved for sale on the Marketplace. But even this process is run by the federal government in Oklahoma, Tennessee, and Wyoming.56
- Alabama
- Alaska
- Arizona
- Delaware
- Florida
- Hawaii
- Indiana
- Iowa
- Kansas
- Louisiana
- Michigan
- Mississippi
- Missouri
- Montana
- Nebraska
- New Hampshire
- North Carolina
- North Dakota
- Ohio
- Oklahoma (Oklahoma transitioned to an SBM-FP on May 1, 2026,7 and plans to become a fully state-run exchange starting in the fall of 2027, for coverage effective in 2028)8
- South Carolina
- South Dakota
- Tennessee
- Texas
- Utah
- West Virginia
- Wisconsin
- Wyoming
How does the exchange model affect open enrollment?
States that use the federally-run marketplace – including FFMs and SBM-FPs – have to follow the open enrollment schedule set by HHS. For the open enrollment period in the fall of 2026 (coverage effective in 2027), this will be November 1 through December 15, which is a month shorter than it was in recent years.
States that run their own exchange platforms have historically been allowed to set their own open enrollment schedules, as long as the final deadline wasn't earlier than December 15. But the federal rule change that was finalized in 2025 also calls for a shorter open enrollment period in most states that run their own exchanges. They will not be allowed to extend open enrollment past December 31, and all plans selected during open enrollment (in every state) will take effect on January 1 of the coming year.
How has management of the marketplaces changed over time?
The exchanges/marketplaces debuted in the fall of 2013, providing coverage for the 2014 plan year. Since then, several states have made changes to their marketplace management. There was initially a trend of states abandoning their own enrollment platforms and opting for HealthCare.gov instead. But we're seeing the opposite happening in the 2020s, with a growing number of states choosing to leave HealthCare.gov and operate their own exchanges with their own enrollment platforms. This gives a state added flexibility (for example, the opportunity to offer state-funded subsidies via the exchange, extend open enrollment, or create state-specific special enrollment periods such as a pregnancy SEP or an easy enrollment SEP) and control, and some states are finding that it's less costly to operate their own exchanges. Here's an overview of the states that have made changes to their marketplace management over the years:
For the 2015 plan year:
- Idaho used HealthCare.gov for enrollment in 2014, but switched to being a fully state-run exchange prior to the 2015 open enrollment period.
- Nevada and Oregon both had state-run exchanges in 2014, but due to technical difficulties, they both opted to become federally-supported state-based exchanges (SBM-FPs) before the 2015 open enrollment period (Nevada has since switched back to having a fully state-run exchange).
For the 2016 plan year:
- Hawaii opted to transition to an SBM-FP, abandoning its state-run enrollment platform (as noted below, Hawaii dropped the state-run aspect altogether the following year).
For the 2017 plan year:
- Arkansas switched from the federally-run exchange to an SBM-FP (enrollment continued to be via HealthCare.gov, so there was no change from a consumer perspective).
- Hawaii switched from an SBM-FP to the federally-run exchange (enrollment continued to be via HealthCare.gov, so there was no change from a consumer perspective).
- Kentucky switched from a state-based exchange to an SBM-FP (Kentucky switched back to a fully state-run exchange and the Kynect enrollment platform in the fall of 2021).
For the 2020 plan year:
Exchange management stayed unchanged for a few years. But several changes took effect in the fall of 2019, for the 2020 plan year:
- Nevada switched to a fully state-run exchange, after having an SBM-FP since 2015. Nevada enrollees now use Nevada Health Link instead of HealthCare.gov.
- New Jersey transitioned to an SBM-FP, after having a federally-run marketplace since 2014 (New Jersey switched to a fully state-run exchange in the fall of 2020, for coverage effective in 2021).
- Pennsylvania also transitioned to an SBM-FP, after having a fully federally-run marketplace in previous years. (Like New Jersey, Pennsylvania stopped using HealthCare.gov in the fall of 2020).
For the 2021 plan year:
The following changes occurred in the fall of 2020:
- Pennsylvania transitioned to a fully state-run exchange, called Pennie (residents no longer use HealthCare.gov).
- New Jersey transitioned to a fully state-run exchange, utilizing the GetCoveredNJ platform (residents no longer use HealthCare.gov).
- Virginia transitioned to an SBE-FP (Virginia transitioned to a fully state-run exchange with its own enrollment platform in the fall of 2023).
- Maine transitioned to an SBM-FP (Legislation was enacted in Maine in 2020 to move forward with the process of creating a state-run exchange, and Maine transitioned to a fully state-run exchange in the fall of 2021.)
For the 2022 plan year:
- New Mexico, Maine, and Kentucky transitioned away from HealthCare.gov as of November 1, 2021, for people enrolling in coverage with a 2022 effective date. All three states had used SBM-FPs for the 2021 plan year.
For the 2024 plan year:
- Virginia has a fully state-run exchange that became operational in the fall of 2023.
For the 2025 plan year:
- Georgia has a fully state-run exchange platform that became operational in November 2024.
- Illinois transitioned to an SBM-FP starting in November 2024 (and an SBM starting in November 2025). This change was due to legislation the state enacted in 2023.9
For the 2026 plan year:
- Illinois has a fully state-run exchange platform (SBM) that became operational in November 2025.10 (legislation enacted in 2023 called for the creation of an SBM-FP by 2025 and an SBM by 2026; CMS confirmed that Illinois was no longer receiving federal Navigator funding as of the 2025 plan year,11 since the state began running an SBM-FP starting in November 2024. Illinois debuted a fully state-run exchange in the fall of 2025.)1
For the 2027 plan year:
- Oregon has an SBM-FP and plans to have a state-run exchange platform starting in the fall of 2026, for coverage effective in 20272 (under the terms of legislation enacted in 2023).12
For the 2028 plan year:
- Oklahoma transitioned to an SBM-FP on May 1, 2026,7 and will utilize that model for the remainder of the 2026 plan year and all of the 2027 plan year.13 But starting in November 2027, for coverage effective in 2028, Oklahoma will have a fully state-run Marketplace.8 This stems from legislation enacted in Oklahoma in May 2025 (which took effect without the governor's signature) that gives the Oklahoma Insurance Commissioner authority to create a state-run exchange.14
Possible changes in future years:
- Mississippi enacted legislation in 2024 that authorizes the Insurance Commissioner to create a state-run exchange. But the legislation (HB1647) became law without the governor's signature.15 Mississippi Insurance Commissioner Mike Chaney has long supported the idea of a state-run exchange,16 but he also clarified that he won't proceed without Governor Reeves's support.17 Nothing had changed about the Mississippi exchange as of 2026. Additional Mississippi legislation, which was approved by the state House of Representatives in February 2026 and sent to the Senate, would have required the state insurance commissioner to create a state-run exchange, but the legislation died in the state Senate.18
As of 2026, legislation was under consideration in North Carolina19 that would authorize the creation of a state-run exchange.
Legislation was introduced in 2026 that called for the creation of a state-run exchange in Florida20 and Wisconsin,21 but the measures failed to advance. And legislation was introduced in Missouri that would have repealed the state's existing prohibition on the creation of a state-run exchange, but the bills did not advance.22
Lawmakers in Texas have considered legislation to create a state-run exchange in previous years, but the bills have died in committee.23
Michigan's Senate passed legislation in 2024 that would have directed the state to create a state-run exchange, but the measure did not advance in the state House.24
Lawmakers in North Carolina25 and Arizona also considered legislation in 2024 that would have created state-run exchanges, but the measures did not advance.26
Rules when transitioning to a state-run exchange
In the rulemaking process for 2024 coverage, HHS finalized a more lenient approval process timeline for states that wish to transition away from the federally-run exchange to establish their own exchange and/or exchange platform. Some additional rules were finalized for the 2025 plan year, but CMS has adopted a more lenient approach starting with the 2027 plan year.
The previous rules (pre-2024) required a state to have federal approval or conditional approval at least 14 months before the start of open enrollment to transition from an SBM-FP to an SBM, and at least three months before the start of open enrollment if transitioning from the FFM to an SBM-FP.
Under the new rules, the approval or conditional approval simply has to be received before the start of open enrollment. States continue to go through the same intensive process of working with HHS to ensure a smooth transition and well-functioning exchange, but no longer have to obtain approval more than a year in advance to establish an SBM.
HHS finalized a rule change for 2025 and future years, requiring a state to operate an SBM-FP for at least one year (including the open enrollment period for that year) before operating a new SBM. This prohibited a state from transitioning directly from the FFM to an SBM.27
But CMS has finalized a rule change for 2027 and future years that eliminates the requirement that a state operate an SBM-FP for a least one year before transitioning to a fully state-run Marketplace.28
CMS had also proposed a new option called the "State Exchange Enhanced Direct Enrollment option" (SBE-EDE), which would have allowed a state-run exchange to "rely exclusively on web-brokers to operate the consumer-facing websites that facilitate the applicant eligibility and enrollment process," as opposed to the exchange running its own consumer-facing enrollment website.29 But this provision was not finalized, so all states will continue to have an exchange, run either by the state or the federal government.30
Change to SHOP (small business) exchange management
Arkansas, Mississippi, and Utah previously ran their own SHOP exchange (the platform for small businesses to enroll in coverage), but switched to using the federal platform or a direct-to-carrier process by 2018. But by that point, even the federal platform for small business enrollment was no longer functioning as it had in past years, and small group enrollment had switched to a direct-to-carrier process in nearly every state. New Mexico was still running its own SHOP exchange platform as of early 2023, but switched to a direct-to-carrier system in mid-2023.
Footnotes
- "Illinois Department of Insurance Releases 2026 Plan Year Rates for the Get Covered Illinois Marketplace" Illinois.gov. Sep. 5, 2025 ⤶ ⤶
- "State-based Marketplace Project" Oregon.gov. Accessed Feb. 3, 2026 ⤶ ⤶
- Oregon Senate Bill 972. BillTrack50. Enacted August 2023. ⤶
- "In-Person Assistance in the Health Insurance Marketplaces; Navigators" Centers for Medicare & Medicaid Services. Accessed Apr. 16, 2025 ⤶
- "State Effective Rate Review Programs" Centers for Medicare & Medicaid Services. Accessed Apr. 16, 2025 ⤶
- "Plan Year 2026 Individual Market Rate Filing Instructions" Centers for Medicare & Medicaid Services. May 2, 2025 ⤶
- "Oklahoma Health Insurance Marketplace Transition Effective May 1, 2026" Oklahoma Insurance Department. May 1, 2026 ⤶ ⤶
- "Oklahoma Insurance Department Announces Transition to Health Insurance State-Based Exchange" Oklahoma Insurance Department. Feb. 11, 2026 ⤶ ⤶
- "Get Covered Illinois Transitions to a State-Based Marketplace this November" Get Covered Illinois. Aug. 11, 2025 ⤶
- "Get Covered Illinois Transitions to a State-Based Marketplace this November" Get Covered Illinois. Aug. 11, 2025 ⤶
- "2024-2025 CMS Navigator Cooperative Agreement Awardees" Centers for Medicare & Medicaid Services. Aug. 26, 2024 ⤶
- Oregon Senate Bill 972. BillTrack50. Enacted August 2023. And Oregon Health Plan (OHP) Bridge Frequently Asked Questions. Oregon Health Authority. May 3, 2024 ⤶
- "Frequently Asked Questions (FAQs), Oklahoma Insurance Department’s Transition to a State-Based Exchange" Oklahoma Insurance Department. Accessed Feb. 17, 2026 ⤶
- "Oklahoma HB1512" BillTrack50. Passed May 8, 2025 ⤶
- "Mississippi HB1647" BillTrack50. Enacted May 14, 2024 ⤶
- "Legislature considering creating a state-based healthcare exchange" WLBT3. April 15, 2024 ⤶
- "Commissioner won’t create Mississippi health insurance exchange unless governor approves" SunHerald. June 20, 2024 ⤶
- "Mississippi HB605" BillTrack50. Died Mar. 3, 2026 ⤶
- "North Carolina S418" and "North Carolina S852" BillTrack50. Accessed May 13, 2026 ⤶
- "Florida H1531" and "Florida H1533" BillTrack50. In committee Jan. 15, 2026 ⤶
- "Wisconsin AB1216" and "Wisconsin AB1153" and "Wisconsin SB1100" BillTrack50. In committee Mar. 2026 ⤶
- "Missouri SB848" and "Missouri HB3136" BillTrack50. Introduced Jan. 2026 ⤶
- "Texas HB5455" and "Texas HB700" and "Texas HB2554" and "Texas SB344" BillTrack50. Introduced 2023 and 2025 ⤶
- "Michigan SB633" BillTrack50. Accessed March 21, 2024. ⤶
- "North Carolina S.789" BillTrack50. Accessed June 26, 2024 ⤶
- "Arizona SB1069" BillTrack50. Accessed June 27, 2024. ⤶
- Patient Protection and Affordable Care Act, HHS Notice of Benefit and Payment Parameters for 2025; Updating Section 1332 Waiver Public Notice Procedures; Medicaid; Consumer Operated and Oriented Plan (CO-OP) Program; and Basic Health Program. U.S. Department of the Treasury; U.S. Department of Health and Human Services. April 2, 2024. ⤶
- "Patient Protection and Affordable Care Act, HHS Notice of Benefit and Payment Parameters for 2027; and Basic Health Program" Centers for Medicare & Medicaid Services, May 15, 2026 ⤶
- "Patient Protection and Affordable Care Act, HHS Notice of Benefit and Payment Parameters for 2027; and Basic Health Program" (Page 444) and "HHS Notice of Benefit and Payment Parameters for 2027 Proposed Rule" Centers for Medicare & Medicaid Services, Feb. 9, 2026 ⤶
- "Patient Protection and Affordable Care Act, HHS Notice of Benefit and Payment Parameters for 2027; and Basic Health Program" Centers for Medicare & Medicaid Services, May 15, 2026 ⤶



