Medicare in Kentucky
Original Medicare, Medicare Advantage, Part D prescription drug, and Medigap coverage in Kentucky

In this article
- Medicare enrollment in Kentucky
- Medicare Advantage plan availability and enrollment in Kentucky
- Medicare supplement (Medigap) plan availability in Kentucky
- Medicare Part D availability and enrollment in Kentucky
- What additional resources are available for Medicare beneficiaries and their caregivers in Kentucky?

Medicare enrollment in Kentucky
As of January 2026, there were 1,005,002 people enrolled in Medicare in Kentucky.1
Medicare eligibility depends mostly on age, but some beneficiaries are eligible because of a disability. About 86% of Kentucky’s Medicare population is eligible due to age (being at least 65), while the other 14% (about 145,000 people) are eligible due to a disability, including amyotrophic lateral sclerosis (ALS) or end-stage renal disease (ESRD).1 Nationwide, about 9% of Medicare beneficiaries are eligible due to a disability.2
Medicare Advantage plan availability and enrollment in Kentucky
About 55% of Kentucky Medicare beneficiaries were enrolled in private Medicare Advantage plans as of January 2026, which was a little higher than the national average of roughly 51%.12
The rest of the state’s Medicare beneficiaries – about 449,000 people – have opted instead for coverage under Original Medicare, which is Medicare Part A and Part B, administered directly by the United States government.3
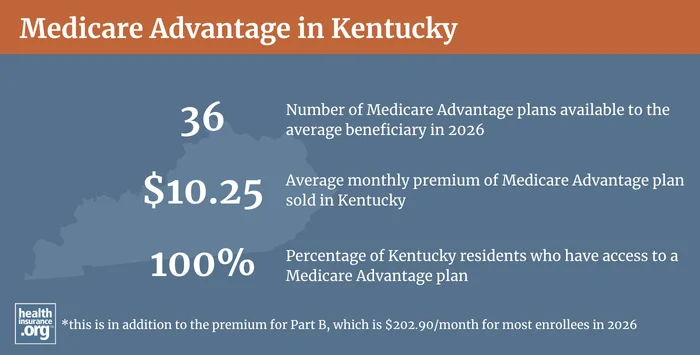
Medicare Advantage plans are offered by private health insurers that have varying service areas, so plan availability varies from one part of the state to another. The average Medicare beneficiary in Kentucky has access to 28 Medicare Advantage plans in 2026.4
Learn more about Medicare Advantage, Medicare’s annual open enrollment period, and the Medicare Advantage open enrollment period.
Learn about Medicare plan options in Kentucky by contacting a licensed agent.



Medicare supplement (Medigap) enrollment and regulations in Kentucky
There are 35 insurers that offer Medigap plans In Kentucky for 2026.5 And as of 2023, according to an AHIP analysis, there were 213,693 Kentucky residents enrolled in Medigap plans.6
Medigap plans are standardized under federal rules, and people are granted a six-month window, when they turn 65 and enroll in Original Medicare, during which coverage is guaranteed issue for Medigap plans.
But federal rules do not guarantee access to a Medigap plan if you’re under 65 and eligible for Medicare as a result of a disability. Most states have adopted rules have adopted rules to ensure at least some access to Medigap plans for disabled enrollees, and Kentucky joined them starting in 2024, due to legislation the state enacted in 2023.7
Under the terms of the 2023 legislation:5
- Kentucky Medigap insurers are required to offer guaranteed issue coverage to Medicare beneficiaries under age 65 who submit an application within the first six months after their Medicare begins. And the insurers cannot charge these applicants premiums higher than the weighted average rates that apply to people age 65 and older.
- Kentucky created a “birthday rule,” which allows a person with Medigap to switch to another insurer’s Medigap plan (same letter as the plan they already have) within 60 days of their birthday, on a guaranteed-issue basis.
Enrollees can call the Medigap insurers directly, or reach out to the Kentucky State Health Insurance Assistance Program for assistance.
Learn more about Medigap, including how it’s standardized and what it covers.
Medicare Part D plan availability and enrollment in Kentucky
As of early 2026, 361,790 Medicare beneficiaries in Kentucky were enrolled in stand-alone Medicare Part D plans. Another 473,778 had Medicare Part D prescription drug coverage incorporated with their Medicare Advantage coverage.1
For 2026 coverage, there are 10 stand-alone Medicare Part D plans available in Kentucky, with premiums starting at $0 per month.8
Learn how Medicare Part D prescription drug coverage works, what it pays for, how and when to enroll.

What additional resources are available for Medicare beneficiaries and their caregivers in Kentucky?
You can contact the Kentucky State Health Insurance Assistance Program for questions and information related to Medicare coverage in Kentucky, Medicare eligibility in Kentucky, or for help understanding your benefits or the process of filing for Medicare benefits.
The Kentucky Department of Insurance regulates and licenses the state’s health insurance companies and the brokers/agents who sell policies in Kentucky. They can answer questions, provide consumers with information and assistance, and address complaints about the entities they oversee.
This overview of how Kentucky Medicaid can help Medicare beneficiaries with low income and low asset levels is a useful resource for beneficiaries and their caregivers.
The Medicare Rights Center is a nationwide service, with a website and call center, that can provide assistance and information related to a variety of Medicare questions and scenarios.

Looking for more information about other options in your state?
Need help navigating health insurance options in Kentucky?
Explore more resources for options in KY including ACA coverage, short-term health insurance, dental and Medicaid.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- “Medicare Monthly Enrollment – Kentucky” Centers for Medicare & Medicaid Services Data. Accessed April 2026. ⤶ ⤶ ⤶ ⤶
- “Medicare Monthly Enrollment – US” Centers for Medicare & Medicaid Services Data, Accessed April 2026. ⤶ ⤶
- “Medicare Monthly Enrollment – Kentucky” Centers for Medicare & Medicaid Services Data. Accessed May 1, 2026 ⤶
- “Medicare Advantage 2026 Spotlight: First Look” KFF.org Dec. 9, 2025 ⤶
- “2026 Medicare Supplement Guide” Kentucky Department of Insurance. Accessed May 1, 2026 ⤶ ⤶
- “The State of Medicare Supplement Coverage” AHIP. May 2025 ⤶
- “Kentucky HB354” BillTrack50. Enacted Apr. 6, 2023 ⤶
- “Fact Sheet: Medicare Open Enrollment for 2026” Centers for Medicare & Medicaid Services. Sep. 26, 2025 ⤶

