Medicaid eligibility and enrollment in Texas
Lack of Medicaid expansion and stringent eligibility requirements drive highest uninsured rate in U.S.


Who is eligible for Medicaid in Texas?
In addition to those with low incomes who are aged, blind, or disabled (receiving SSI benefits), the following populations are eligible for Medicaid in Texas:1
- Children aged 0-1: 198% of the federal poverty level (FPL)
- Children aged 1-5: 144% of FPL
- Children age 6-18: 133% of FPL
- Pregnant women: 198% of FPL
- Adults caregivers of children or adult relatives: 12% of FPL
- Children are eligible for either Medicaid or CHIP if their household incomes are up to 201% of poverty
Texas has not expanded Medicaid under the ACA, so adults under 65 who aren’t disabled or raising a child are ineligible for Medicaid regardless of how low their income is.
for 2026 coverage
0.0%
of Federal Poverty Level
Apply for Medicaid in Texas
You can enroll through HealthCare.gov or the state Medicaid website. You can enroll by phone at 800-318-2596.
Eligibility: The aged, blind, and disabled. Also, parents with dependent children are eligible with household incomes up to 15% of FPL. Children are eligible for Medicaid or CHIP with household incomes up to 201% of FPL, and pregnant women are eligible with household incomes up to 198% of FPL.



Is the ACA’s Medicaid expansion implemented in Texas?
Texas has not expanded Medicaid under the Affordable Care Act (ACA). As a result, Texas has the biggest coverage gap in the country, with an estimated 570,000 residents ineligible for Medicaid and also ineligible for premium subsidies to offset the cost of private coverage in the exchange.2
Because Texas has chosen to not accept federal funds to expand Medicaid, enrollment in Texas Medicaid/CHIP was actually slightly lower in late 2024 than it had been in 2013 (nationwide, Medicaid enrollment has grown by 38% since then).3
Several Medicaid expansion (or partial Medicaid expansion or privatized Medicaid expansion) bills were introduced in the Texas legislature in early 2025, although all of them had died by mid-2025.4 One additional bill was introduced in July 2025, after the others had died.5 All previous legislative efforts to expand Medicaid in Texas have been unsuccessful.
Prior to 2014, Texas had the highest uninsured rate in the country, and that is still the case. The state’s uninsured rate stood at more than 16% in 2023, which was still the nation’s highest uninsured rate by a considerable margin.6
HHS reported that 45% of Texas adults (age 19-64) with income under 138% of the poverty level were uninsured as of 2020, which was the highest level in the country (that population would become Medicaid-eligible if Texas were to expand Medicaid). Various studies and reports show lagging health outcomes and a nationally high uninsured rate at least partly due to the decision against expanding Medicaid in Texas.
As the ACA was written, it called for Medicaid expansion in every state for legally present residents with incomes up to 133% of poverty (138%, with the built-in 5% income disregard). But in 2012, the Supreme Court ruled that states could not be penalized for opting out of expansion, and Texas has chosen to keep its pre-2014 Medicaid eligibility rules.
That means non-disabled adults without minor children are ineligible for Medicaid regardless of how low their income is. Parents with minor children are only eligible if the children are enrolled in Medicaid and if the household income doesn’t exceed approximately 12% of the poverty level (Texas uses a flat dollar amount for eligibility, but CMS converts that to a percentage). So for a single parent with two kids, the parent is only eligible for Medicaid if their total household income doesn’t exceed $230/month. This limit is so low that it essentially makes it impossible for the parent to hold even a part-time job, since they will lose their health coverage if their earnings go above that amount.
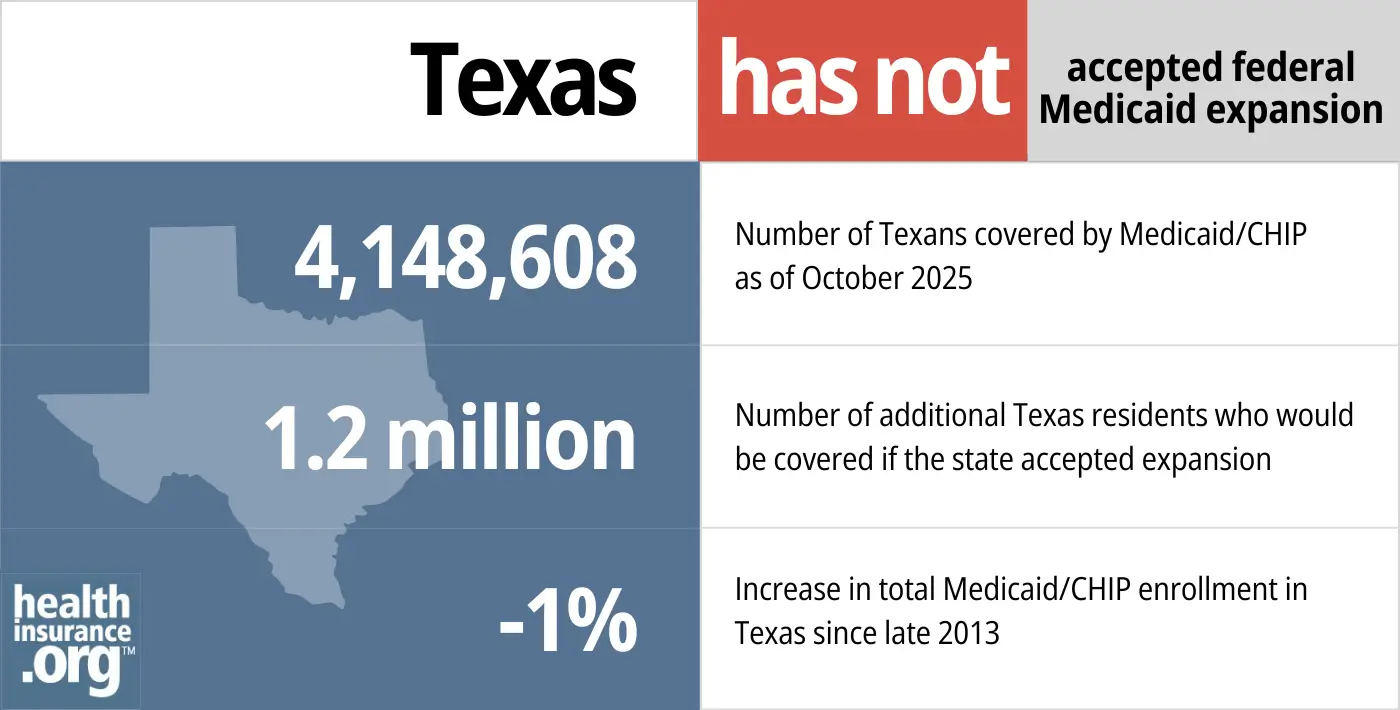
- 4,148,608 – Number of Texans covered by Medicaid/CHIP as of October 20257
- 1.2 million – Number of additional Texas residents who would be covered if the state expanded Medicaid8
- -1% – Increase in total Medicaid/CHIP enrollment in Texas since late 20139
Explore our other comprehensive guides to coverage in Texas

The ACA Marketplace allows individuals and families to shop for and enroll in ACA-compliant health insurance plans. Subsidies may be available based on household income to help lower costs.


Hoping to improve your smile? Dental insurance may be a smart addition to your health coverage. Our guide explores dental coverage options in Texas.


Use our guide to learn about Medicare, Medicare Advantage, and Medigap coverage available in Texas as well as the state’s Medicare supplement (Medigap) regulations.


Short-term health plans provide temporary health insurance for consumers who may find themselves without comprehensive coverage.

Frequently asked questions about Texas Medicaid
How can I enroll in Texas Medicaid?
If you believe you may be eligible to enroll in Medicaid in Texas:
- You can start the process through HealthCare.gov, either online or by phone at 1-800-318-2596. (Use this option if you’re under 65 and don’t have Medicare; you will be directed to the Texas Medicaid agency if HealthCare.gov believes you’re eligible for that coverage.)
- You can enroll through the Medicaid website maintained by the Texas Health and Human Services Commission.
- You can also download and print a paper application, or request that one be mailed to you, by using this page on the Texas Medicaid website.
How does Medicaid provide financial assistance to Medicare beneficiaries in Texas?
Many Medicare beneficiaries receive Medicaid’s help with paying for Medicare premiums, affording prescription drug costs, and covering expenses not reimbursed by Medicare – such as long-term care.
Our guide to financial assistance for Medicare enrollees in Texas includes overviews of these benefits, including Medicare Savings Programs, long-term care coverage, and eligibility guidelines for assistance.
How many Texas residents lost their Medicaid after the pandemic?
In every state, Medicaid disenrollments were paused from March 2020 through March 2023, as a result of the COVID pandemic. Even if a Medicaid enrollee’s circumstances changed and they were no longer eligible, their coverage was not discontinued. But that ended March 31, 2023, and states resumed regular eligibility redeterminations.
In Texas, Medicaid enrollment grew steadily throughout the pandemic, increasing from about 4 million people in early 2020 to nearly 6 million by April 2023. Under federal rules, all Medicaid enrollees’ eligibility had to be redetermined at some point in the year-long “unwinding” period that began in the spring of 2023. Texas prioritized eligibility determinations for people they expected to no longer be eligible for Medicaid (including, for example, people who had aged out of the children’s eligibility category, or people who were covered due to pregnancy and had since given birth).
By the end of the year-long unwinding process, nearly 2.5 million people had been disenrolled from Texas Medicaid, and enrollment had dropped to about 4.2 million people.10
Most of the disenrollments — about 1.7 million people — were for procedural reasons. This means the state didn’t have enough information to determine whether the person was still eligible or not.10
Legislation impacting Texas Medicaid
Uncompensated care: Billons in federal funding each year
Political leaders in Texas have remained mostly uninterested in expanding Medicaid. Instead of pushing for legislation to expand Medicaid, Texas officials negotiated with CMS in an effort to secure ongoing funding to cover uncompensated care in the state. The state’s 1115 waiver was initially approved in 2011, and was intended to temporarily ensure funding for uncompensated care prior to the expansion of Medicaid. But after the Supreme Court’s 2012 ruling essentially made Medicaid expansion optional for states, Texas has rejected Medicaid expansion and instead continued to rely on the 1115 waiver’s federal funding to cover uncompensated care.
The Obama Administration had previously noted that uncompensated care funding would be largely unnecessary if states expanded Medicaid, but the Trump administration was more willing to work with states that had refused federal funding for Medicaid expansion.
Texas officials were successful in getting the Trump Administration to agree to a five-year extension of the state’s waiver for uncompensated care, and Texas received $25 billion in federal funding as a result, from 2018 through 2022. (The state’s 1115 waiver details are available here.) And in January 2021, the Trump administration agreed to extend the 1115 waiver out through 2030.
The Biden administration rescinded that extension soon after taking office. A few months later, however, a judge temporarily blocked the federal government from rescinding the 1115 waiver’s extension. But in September 2021, the federal government halted payments to the state over concerns about how Texas was funding its share of the cost. In March 2022, that funding — which amounts to $7 million per day — was restored.
That’s more than $2.5 billion in annual federal funding. But it’s worth noting that Texas would receive an estimated $6 billion in annual federal funding by expanding Medicaid, and the effect of that influx of federal money would have a ripple effect on the state’s economy that would amount to $100 billion over ten years. Expanding Medicaid would be a financial boon to Texas.
Missing out on billions in federal funding
By refusing Medicaid expansion under the ACA, Texas has already missed out on billions in federal funding that would otherwise have flowed to the state to provide medical care for their low-income residents. The current estimate is that Texas is rejecting between $5 billion and $6 billion in federal funds every year that the state refuses to implement Medicaid expansion.11
In addition, the state’s emergency rooms are providing $5.5 billion in uncompensated care each year, treating patients who don’t have health insurance (as noted above, the state is receiving about $2.5 billion in annual federal funding to cover uncompensated care). If Medicaid eligibility had been expanded, uncompensated care would have dropped considerably, so hospitals and business groups across the state have been pressuring lawmakers to relent on their opposition to Medicaid expansion.
Because Texas has refused to expand Medicaid, the federal government has warned the state that continued access to federal funding to help cover uncompensated care is in jeopardy (since Medicaid expansion would solve much of the uncompensated care problem). But Governor Greg Abbott has continued to reject Medicaid expansion, and described the federal government’s tactics as “coercive”
Since residents in states not expanding Medicaid still have to pay federal taxes, there has been a significant outflow from Texas residents to fund Medicaid expansion in other states.
Texas Medicaid history
During the 2013 legislative session, Republican John Zerwas sponsored HB3791, which would have directed the state to craft a “Texas solution” to Medicaid expansion. But it did not pass. The bill called for reforming the state’s Medicaid system while also accepting federal funding to expand the program. It also included “personal responsibility” measures like copays and deductibles, and would have included premium assistance programs to help people purchase private insurance as a preferable alternative to traditional Medicaid.
But also in 2013, Republican lawmakers in Texas passed a measure that requires the state Health and Human Services Commission to receive approval from the legislature before any future Medicaid expansion decisions could be made. So ultimately, even if a governor were to support Medicaid expansion, the decision rests with the Texas Legislature. This makes expansion very unlikely in the near future, given lawmakers’ general rejection of the idea.
As long as Medicaid eligibility continues to be unchanged from 2013 guidelines, the cost of uncompensated care in Texas hospitals is roughly $5.5 billion a year, and it’s largely paid by tax dollars and higher health insurance premiums for people who do have coverage, in addition to federal funding that the state has secured via an 1115 waiver.
Former Governor Rick Perry repeatedly rejected Medicaid expansion. During the 2014 Governor’s race, Republican Greg Abbott (who won by a significant margin) agreed with Perry and expressed his opposition to accepting federal funding to expand Medicaid (both men claimed that the eventual 10% of the cost that the state would pay by 2020 would be too much for the budget). Democratic candidate Wendy Davis was in favor of Medicaid expansion in Texas, but she lost the election.
In late 2014, Abbott expressed interest in Utah’s Medicaid expansion waiver (Utah ultimately ended up seeking federal approval to expand Medicaid only to the poverty level, but voters took the matter into their own hands in 2018, passing a ballot initiative that ultimately resulted in Utah fully expanding Medicaid as of 2020). And while that instilled hope that Abbott might soften his stance towards Medicaid expansion, he remains opposed to it.
It’s noteworthy that in November 2014, a 15-member board of medical professionals appointed by Governor Perry recommended that the state move forward with Medicaid expansion. The Texas Institute of Health Care Quality and Efficiency board has recommended Medicaid expansion as a solution to what they called an “unacceptable” number of people without health insurance in Texas.
State lawmakers only meet in odd-numbered years in Texas. Numerous bills were introduced in 2015 in an effort to expand coverage, but none were successful. While multiple bills were filed in 2019, they were not passed. And Medicaid expansion legislation in 2021 was also unsuccessful. Several bills related to Medicaid expansion were filed in 2023, including HB1062, HB1144, and SB343, but none were successful. As noted above, additional Medicaid expansion bills have been introduced in 2025, but experts doubt they will be successful.8

Looking for more information about other options in your state?
Need help navigating health insurance options in Texas?
Explore more resources for options in TX including ACA coverage, short-term health insurance, dental and Medicare.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- ”Medicaid, Children’s Health Insurance Program, & Basic Health Program Eligibility Levels” Medicaid.gov. Accessed May 12, 2026 ⤶
- ”How Many Uninsured Are in the Coverage Gap and How Many Could be Eligible if All States Adopted the Medicaid Expansion?” KFF.org. Feb. 25, 2025 ⤶
- ”Total Monthly Medicaid & CHIP Enrollment and Pre-ACA Enrollment” KFF.org. Accessed Feb. 4, 2025 ⤶
- ”Texas HB4910” and “Texas HB2627” and “Texas HB2604” and “Texas SB232” and “Texas SB657” and “Texas SB289” and “Texas HB3216” and “Texas HB2939” and “Texas HB3072” and “Texas HB1903” BillTrack50. Bills died June 2025 ⤶
- ”Texas HB72” BillTrack50. Introduced July 14, 2025 ⤶
- ”Health Insurance Coverage and Type by State” U.S. Census Bureau. Sep. 12, 2024 ⤶
- “October 2025 Medicaid & CHIP Enrollment Data Highlights”, Medicaid.gov, Accessed February 2026 ⤶
- ”Will 2025 be the year Texas expands Medicaid? Not likely, advocates say” Kera News. Jan. 7, 2025 ⤶ ⤶
- ”Total Monthly Medicaid & CHIP Enrollment and Pre-ACA Enrollment” KFF, Accessed February 2026 ⤶
- ”Medicaid Enrollment and Unwinding Tracker (Texas)” KFF.org. Jan. 31, 2025 ⤶ ⤶
- ”Fact-check: Did Texas turn down $100 billion when Republicans rejected Medicaid expansion?” Austin-American Statesman. Jan. 9, 2025 ⤶

