Medicaid eligibility and enrollment in Mississippi
Mississippi’s 2025 Medicaid expansion bills died in committee, so a coverage gap continues for the states’s poorest residents


Who is eligible for Medicaid in Mississippi?
As published by CMS, these are the income limits for key coverage groups under Mississippi’s Medicaid program1 (note that these numbers include a built-in 5% income disregard that’s used for income-based Medicaid eligibility determinations):
- Adults with dependent children are eligible if their household income doesn’t exceed 24% of poverty level. This is about $488 per month for a family of three,2 one of the lowest thresholds in the country.
- Infants under one are eligible for Medicaid if their household income is up to 199% of poverty.
- Children 1 – 5 are eligible if their household income is up to 148% of poverty.
- Children 6 – 18 are eligible if their household income is up to 138% of poverty.
- Children with household incomes above the Medicaid thresholds are eligible for CHIP if their household incomes are up to 214% of poverty
- Pregnant women are eligible for Medicaid if their household income does not exceed 199% of poverty. (Postpartum coverage for the mother continues for 12 months after the birth;3 Mississippi enacted legislation in 2023 to extend it from the 60-day limit that was previously used.)
for 2026 coverage
0.0%
of Federal Poverty Level
Apply for Medicaid in Mississippi
You can enroll through HealthCare.gov or you can fill out a PDF of the Mississippi Medicaid Application Form. You can also enroll by phone at 800-318-2596.
Eligibility: Parents with dependent children are eligible with household incomes up to 22% of FPL. Children are eligible for Medicaid or CHIP with household incomes up to 209% of FPL, and pregnant women are eligible with household incomes up to 194% of FPL.



Has Mississippi expanded Medicaid eligibility?
No, Mississippi has not implemented Medicaid expansion under the ACA, despite the state medical association’s support of expansion going back to August 2016.4 So non-disabled adults without dependent children are not eligible for Medicaid in Mississippi regardless of how low their income is.
Several Medicaid expansion bills were introduced in Mississippi’s legislature in 2024 to expand Medicaid under the ACA, including HB 1725.5 That legislation passed in the Mississippi House in February 2024, and the Senate passed a different version in March, with a stronger work requirement that would have made expansion largely infeasible. The two chambers could not reconcile their differences by the end of 2024 the session, and the measure died.6
Lawmakers said that Medicaid expansion was likely to be considered again in the 2025 legislative session,7 and several new Medicaid expansion bills were filed in January 2025.8 But all of them had died in committee by early February, 2025.
Additionally, legislation was introduced in 2025 in Mississippi that would have directed the state to study the feasibility and impacts of implementing Medicaid expansion and work requirements, but those bills had also died in committee by early February.9
Mississippi is one of just 10 states that have not yet expanded Medicaid as of 2025.
2024 was the first year that any Medicaid expansion bill had advanced out of committee in Mississippi, after House Speaker Jason White clarified in the fall of 2023 that Medicaid expansion would be addressed by the legislature in 2024. White noted “I think we as Republicans have probably earned a little bit of the bad rap we get on health care in Mississippi. Part of that is that we haven’t had a full-blown airing or discussion of Medicaid expansion. We’ve just said, ‘No.’”10
The bill passed by the Mississippi House included a 20-hour-per-week work requirement, but it also noted that if CMS refused to approve the work requirement (as expected under the Biden administration), Medicaid expansion would still take effect from 2025 through early 2029 (a repeal clause in the bill would have ended expansion at that point, unless lawmakers reauthorized it).
But the Senate’s version of the bill included a 30-hour-per-week work requirement and would not have allowed expansion to be implemented if the work requirement wasn’t approved by CMS. That was essentially a poison pill for Medicaid expansion, as it was expected that the Biden administration would not approve a Medicaid work requirement.
The two chambers worked to reconcile their differences. The Senate offered a version with a 100-hour-per-month work requirement, but still with a clause that would prevent expansion if the federal government didn’t approve the work requirement. The House offered a proposal to put a referendum on the 2024 ballot in Mississippi, asking voters to weigh in on whether Medicaid should be expanded, and if so, whether there should be a work requirement. Senate Republicans were strongly opposed to the ballot referendum proposal, and a citizen-led Medicaid expansion ballot measure cannot be used in Mississippi to expand Medicaid the way several other states have done.11
Non-disabled adults without children are not eligible for Medicaid in Mississippi regardless of how low their income is, and parents with dependent children are only eligible with incomes that don’t exceed 24% of the poverty level (including a built-in 5% income disregard). This is one of the lowest eligibility caps in the country — only Texas and Alabama have lower limits.12
If Mississippi did expand eligibility for Medicaid as called for in the ACA, an estimated 123,000 currently uninsured adults would be newly eligible for coverage.13 And total Medicaid enrollment would grow by more than 240,000 people.14 Unfortunately, in the poorest, sickest state in the U.S., the majority of lawmakers and two governors have opted to reject federal funds that would provide health insurance for the state’s poorest residents.
Because Marketplace subsidies are only available in Mississippi for people whose household incomes are at least 100% of poverty, an estimated 74,000 people in Mississippi are in the coverage gap and have no realistic access to health insurance15 (some analyses indicate an even larger number of people in the coverage gap in Mississippi). They aren’t eligible for Medicaid, and they also aren’t eligible for subsidies.
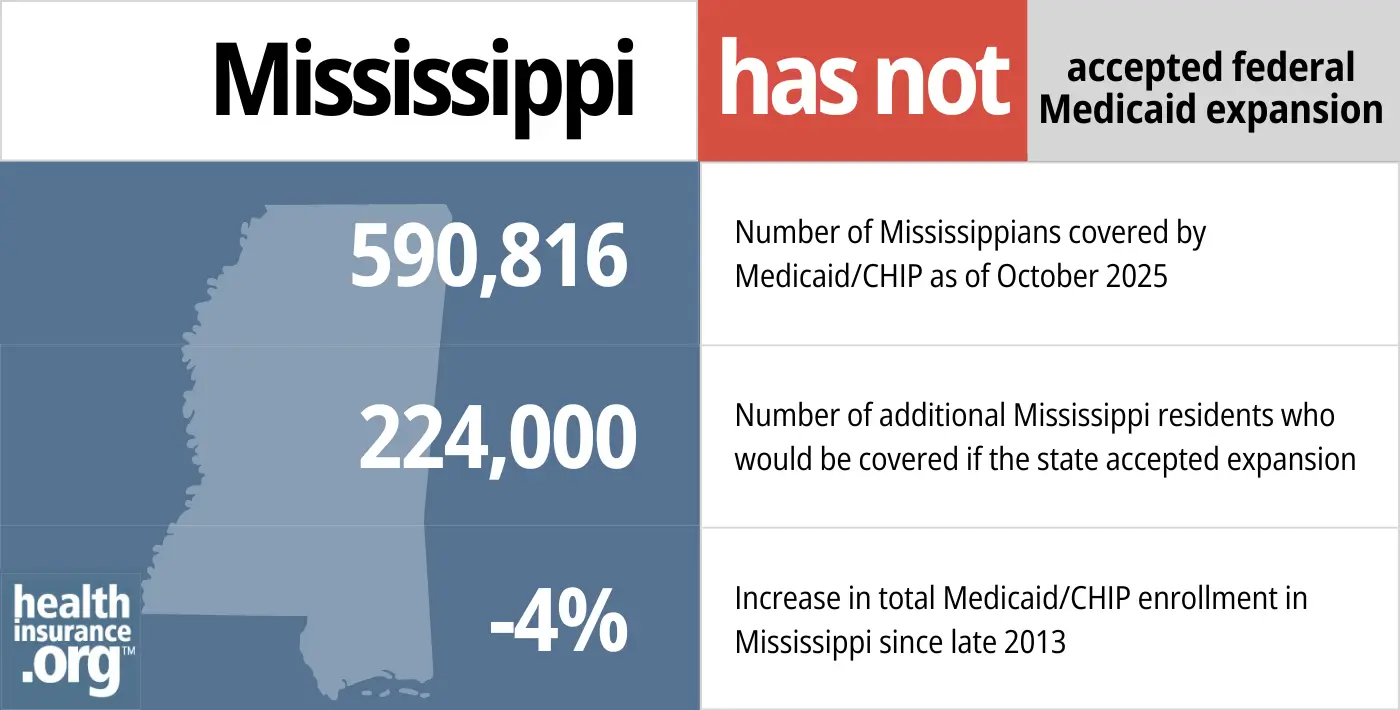
- 590,816 – Number of Mississippians covered by Medicaid/CHIP as of October 202516
- 224,000 – Number of additional Mississippi residents who would be covered if the state accepted expansion14
- -4% – Increase in total Medicaid/CHIP enrollment in Mississippi since late 201317
Explore our other comprehensive guides to coverage in Mississippi

The ACA Marketplace allows individuals and families to shop for and enroll in ACA-compliant health insurance plans. Subsidies may be available based on household income to help lower costs.
Learn about the health insurance Marketplace in Mississippi.


Hoping to improve your smile? Dental insurance may be a smart addition to your health coverage. Our guide explores dental coverage options in Mississippi.


Use our guide to learn about Medicare, Medicare Advantage, and Medigap coverage available in Mississippi as well as the state’s Medicare supplement (Medigap) regulations.


Short-term health plans provide temporary health insurance for consumers who may find themselves without comprehensive coverage.
Learn about short-term insurance regulations in Mississippi.

Frequently asked questions about Mississippi Medicaid eligibility and enrollment
How do I enroll in Medicaid in Mississippi?
If you are under 65 and don’t have Medicare:
- You can apply online at Access MS.
- You can begin the process at HealthCare.gov, either online or by phone at 1-800-318-2596. If you’re expected to be eligible for Medicaid, HealthCare.gov will send your information to Mississippi Medicaid, where you can finish the enrollment.
- You can fill out the PDF version of the Mississippi Medicaid Application Form and either click the application submit button, or save the completed PDF and email it to [email protected].
- You can also print out the PDF application, complete it by hand, and fax, mail, or deliver it in person. You can fax it to 601-576-4164. You can mail it to 550 High Street, Suite 1000, Jackson, MS 39201. Or you can take it to your nearest Mississippi Division of Medicaid regional office.
If you are 65 or older or have Medicare, use this website to apply for Medicaid.
How does Medicaid assist Medicare beneficiaries in Mississippi?
Many Medicare beneficiaries receive assistance through Medicaid with the cost of Medicare premiums, cost sharing, and services Medicare doesn’t cover — such as long-term care.
Our guide to financial assistance for Medicare beneficiaries in Mississippi explains these benefits, including Medicare Savings Programs, Extra Help, long-term care benefits, and income guidelines for assistance.
How did Mississippi handle Medicaid renewals after the pandemic?
Medicaid disenrollments were paused nationwide from March 202o through March 2023. Even if a person’s circumstances changed and they were no longer Medicaid-eligible, their coverage continued throughout the pandemic. Starting in early-mid 2023, states began checking the eligibility of everyone enrolled in Medicaid and disenrolling those who no longer met the eligibility criteria or who failed to respond to a renewal notice.
The first round of disenrollments in Mississippi came in June 2023, By the time the unwinding process ended in Mississippi in May 2024, 149,948 people had been disenrolled from Mississippi Medicaid.18
Mississippi continued to request eligibility verification from enrollees throughout the pandemic, as did many other states. But people who didn’t respond or who were no longer eligible could not be disenrolled unless they requested that. Instead, Mississippi moved these people from managed care plans to fee-for-service Medicaid during the pandemic. This saved the state some money, but potentially reduced some enrollees’ access to the supplemental services that the Medicaid managed care plans provide.
If a person is no longer eligible for Medicaid and also not eligible for Medicare or an employer’s health plan, they will need to obtain their own replacement coverage. In most cases, the exchange/Marketplace is the best way to do this, and Mississippi uses HealthCare.gov as its marketplace.
CMS reported that more than 70,000 people had transitioned from Mississippi Medicaid to a Marketplace plan during the unwinding process.19
Because Mississippi has not expanded Medicaid under the ACA, the state does still have a coverage gap for adults with income below the poverty level. So it’s important for low-income residents to be aware of how to avoid this coverage gap.
Legislation impacting Mississippi Medicaid
Why did Mississippi's 2022 ballot not have a Medicaid expansion initiative?
In 2021, Medicaid expansion advocates in Mississippi began gathering signatures to get Initiative 76 on the 2022 ballot. This measure would have let the state’s voters decide whether Medicaid should be expanded, and it’s worth noting that this approach has resulted in Medicaid expansion in several other states — voters have never failed to pass a Medicaid expansion measure in any state when it has been on the ballot.
However, Initiative 76 was suspended in mid-2021, after it was determined that a state Supreme Court ruling in 2020 had invalidated the Mississippi ballot initiative process. So voters in Mississippi did not get a chance to weigh in on Medicaid expansion in the 2022 election.
As noted above, efforts to revive the citizen-led ballot initiative in Mississippi failed in the 2024 legislative session.11
Mississippi's proposed Medicaid work requirement
Even though Mississippi hasn’t expanded Medicaid and has some of the most stringent eligibility guidelines in the country, the state has sought federal approval to make it even harder for people to get Medicaid coverage in Mississippi.
In October 2017, Mississippi submitted a proposed 1115 waiver to CMS, detailing the work requirement that the state wants to implement. The waiver was still pending approval as of early 2025, before the second Trump administration took office.
The Biden administration had informed states that Medicaid work requirements were not compatible with the mission of Medicaid. The first Trump administration had approved several states’ proposed Medicaid work requirements, but the Biden administration revoked all of those approvals. Proposals like Mississippi’s, which were still pending when President Biden took office, were left pending throughout the Biden administration.
(Georgia implemented a work requirement in 2023, but only for the population that became newly eligible for the state’s partial Medicaid expansion at the same time. The work requirement in Georgia does not apply to anyone who was already eligible for coverage.)
Mississippi’s proposal would allow the state to require some Medicaid enrollees to work, volunteer, attend school, participate in substance abuse treatment, or otherwise fulfill the work requirement for at least 20 hours per week.
People would be exempt if they are disabled, physically or mentally unable to work, a primary caregiver for someone in need of care, elderly, under the age of 19, pregnant, Native American, or included in various other exempt populations. Since Mississippi has not expanded Medicaid under the ACA, the vast majority of the state’s Medicaid enrollees would already be exempt from the work requirement. The work requirement would really only apply to certain low-income parents and people receiving transitional medical assistance (a program that extends Medicaid coverage for up to 12 months for people who start earning too much money to continue to qualify for Medicaid).
Mississippi Medicaid covers more than 600,000 people, but only about 56,000 of them are in the low-income parent Medicaid eligibility category. And of those, most would have exemptions. About 15,000 to 20,000 people would end up having to work as a result of the work requirement, and many are already working.
Ultimately, about 5,000 people would be expected to lose coverage in Mississippi each year if the work requirement were to be approved and implemented (as noted above, that is not likely to happen under the Biden administration). According to the Clarion-Ledger, 91% of the people who would lose access to Medicaid under the proposed work requirement in Mississippi are low-income mothers. And more than two-thirds are African American.
These low-income parents are in a catch-22 situation: If they earn more than 27% of the poverty level (that works out to about $518/month for a household of three), they’d no longer be eligible for Medicaid. And if they don’t work, they’ll also lose access to Medicaid as a result of the work requirement. So in order to have health insurance, they would either have to maintain a job that provides health insurance coverage, or earn at least 100% of the poverty level so that they could obtain premium subsidies in the exchange and purchase an affordable individual health plan. One hundred percent of the poverty level is about $1,919/month for a household of three, so it’s a big jump from the Medicaid eligibility cutoff to the start of eligibility for premium subsidies.
To address these concerns, the state proposed an additional 12 months of transitional Medicaid coverage for people who remain in compliance with the work requirement for the full 24 months. Georgetown University’s Joan Alker describes this as a “wholly inadequate solution.” It’s temporary, doesn’t provide any sort of solution after the 24 months of transitional Medicaid coverage ends, and hinges on the unrealistic expectation that low-income, working parents will not experience even one month of unemployment during their 24 months of transitional Medicaid.
CMS had initially opened a comment period in early 2018 for Mississippi’s waiver proposal. But after the state revised the proposal to add 12 months of transitional Medicaid coverage, the comment period was re-opened. During the re-opened comment period, 320 comments were submitted, and 319 of them were in opposition to the state’s proposed Medicaid work requirement. The revised proposal was still under review by CMS as of early 2025.
Mississippi Medicaid enrollment numbers
Total Mississippi Medicaid/CHIP enrollment was 602,825 as of October 2024,20 including 518,360 people with Medicaid and 84,465 children with health insurance coverage under CHIP.
Total enrollment in Mississippi Medicaid/CHIP was 2% lower in October 2024 than it had been in late 2013.21 Mississippi was one of only three states where enrollment had declined from late 2013 to late 2024; nationwide, total enrollment had grown by 38% during that timeframe.
Missing out on billions in federal funding
As the ACA was written, it called for Medicaid expansion in every state for residents with incomes up to 133% of poverty (plus a 5% income disregard, bringing the effective eligibility threshold to 138% of the poverty level). But in 2012, the Supreme Court ruled that states could not be penalized for opting out of expansion, and Mississippi is one of only ten states that have not yet expanded Medicaid.
In states that expand Medicaid, the federal government paid the full cost of expansion through 2016. After that, states gradually began to pay a share of the expansion cost, but the federal government will always pay at least 90%. As a result, states that reject Medicaid expansion are leaving billions of dollars on the table.
From 2013 through 2022, Mississippi gave up $14.5 billion in federal funding that would otherwise have been available to the state to help provide medical care for low-income residents. And states that newly expand Medicaid after April 2021 are eligible for two years of additional federal Medicaid funding under the American Rescue Plan, but Mississippi has not yet taken advantage of that.
Since residents in states not expanding Medicaid still have to pay federal taxes, Mississippi residents have been subsidizing Medicaid expansion in other states. Over a decade, people in Mississippi are paying $1.7 billion in federal taxes that are used to pay for Medicaid expansion in other states.
Will Mississippi expand coverage?
Governor Tate Reeves, who assumed office in 2020, campaigned in opposition to Medicaid expansion. His viewpoint is consistent with former Governor Phil Bryant. Bryant claimed that the state wouldn’t be able to bear the cost if the federal government were ever unable to uphold its promise to pay at least 90% of the cost, and referred to accepting Medicaid expansion as a “fool’s errand.”
Mississippi’s share of traditional Medicaid costs climbed from fiscal year 2012 to fiscal year 2017. Lawmakers have highlighted this as a reason for not expanding coverage, but they’re missing the point (whether purposely or not) that Medicaid expansion is funded under different rules from traditional Medicaid. Under Medicaid expansion, the cost to cover newly eligible residents was fully funded by the federal government through the end of 2016. In 2020 and forward, states pay 10% of costs associated with the Medicaid expansion population.
And of particular importance, states that have expanded Medicaid have seen substantially smaller growth in state Medicaid spending than states that haven’t expanded Medicaid.
In June 2013, Republicans in both chambers of the Mississippi legislature voted against Medicaid expansion. They did vote to continue the state’s existing Medicaid program, which came within days of expiring and had to be dealt with in a special legislative session called by Bryant. The issue of Medicaid expansion might not have even made it to a vote except that Democrats threatened to withhold their votes for renewing the existing Medicaid program unless Republicans would agree to take the issue of Medicaid expansion to a vote. No Republicans voted for Medicaid expansion, although one, Senator Billy Hudson of Hattiesburg, said that he would eventually vote for Medicaid expansion, “but not today.”
The Mississippi State Medical Association put forth a resolution in August 2016 calling for “expanded coverage” but didn’t use the words “Medicaid expansion” in their draft, knowing that the issue was too politically charged.
As described above, Mississippi lawmakers finally considered Medicaid expansion during the 2024 legislative session, but were unable to come to an agreement. And legislation has been introduced to reconsider the issue in 2025. But for now, in the nation’s poorest state, the poorest residents have no access to health coverage at all.

Looking for more information about other options in your state?
Need help navigating health insurance options in Mississippi?
Explore more resources for options in MS including ACA coverage, short-term health insurance, dental and Medicare.
Speak to a sales agent at a licensed insurance agency.
Footnotes
- ”Medicaid, Children’s Health Insurance Program, & Basic Health Program Eligibility Levels” Centers for Medicare & Medicaid Services. Dec. 1, 2023. ⤶
- Income Limits for Medicaid and CHIP Programs. Mississippi Division of Medicaid. Accessed January 2024. ⤶
- MS SPA 23-0015 Postpartum Coverage approved by CMS. Mississippi Division of Medicaid. Accessed January 2024. ⤶
- ”Medicaid expansion should be explored” Hattiesburg American. Aug. 31, 2016 ⤶
- ”Mississippi House Bill 1725” BillTrack50. Accessed May 9, 2024 ⤶
- ”‘Stupidity of politics’: Medicaid expansion effort dies in Mississippi” MPB. May 6, 2024 ⤶
- ”MS lawmakers looking to pass income tax changes, Medicaid expansion in 2025. See why” Mississippi Clarion Ledger. May 8, 2024 ⤶
- ”Mississippi HB706” and “Mississippi HB466” and “Mississippi HB427” and “Mississippi HB132” and “Mississippi HB55” and “Mississippi HB125“BillTrack50. Accessed Feb. 6, 2025 ⤶
- ”Mississippi SB2888” and “Mississippi HB1591” BillTrack50. Introduced Jan. 20, 2025 ⤶
- Are Republicans about to leave Gov. Tate Reeves behind on Medicaid expansion? Mississippi Today. September 2023. ⤶
- ”Mississippi Keeps the Door Firmly Shut on Ballot Initiatives” Bolts. April 4, 2024 ⤶ ⤶
- Medicaid, Children’s Health Insurance Program, & Basic Health Program Eligibility Levels. Centers for Medicare and Medicaid Services. Dec. 1, 2023. ⤶
- ”A Closer Look at Medicaid Expansion Efforts in Mississippi” KFF.org. Mar. 12, 2024 ⤶
- ”A Fiscal and Economic Analysis of Medicaid Expansion in Mississippi Under the Patient Protection and Affordable Care Act” Mississippi State Institutions of Higher Learning. June 2024 ⤶ ⤶
- How Many Uninsured Are in the Coverage Gap and How Many Could be Eligible if All States Adopted the Medicaid Expansion? KFF. Feb. 26, 2024 ⤶
- “October 2025 Medicaid & CHIP Enrollment Data Highlights”, Medicaid.gov, Accessed February 2026 ⤶
- Total Monthly Medicaid & CHIP Enrollment and Pre-ACA Enrollment, KFF.org, Accessed February 2026 ⤶
- ”Medicaid Enrollment and Unwinding Tracker” KFF.org. Jan. 8, 2025 ⤶
- HealthCare.gov Marketplace Medicaid Unwinding Report. Centers for Medicare and Medicaid Services. Accessed Jan. 16, 2025 ⤶
- ”October 2024 Medicaid & CHIP Enrollment Data Highlights” Medicaid.gov, Accessed Jan. 16, 2025 ⤶
- Total Monthly Medicaid & CHIP Enrollment and Pre-ACA Enrollment. KFF. October 2024. Accessed Jan. 16, 2025 ⤶

